NCI can be divided into infectious colitis,
vasculitis,
bowel ischemia,
radiation enteritis,
drug-related enteritis,
endometriosis,
eosinophilic gastroenteritis,
ileitis associated with spondyloarthropathies.
NCI show non specific CT-E and MR-E findings such as bowel-wall thickening,
obstruction or ascites.
Differential diagnosis can be done observing specific radiological signs and clinical correlations (concomitant reactive arthritis) or patients associated treatment (drugs or radiation therapy).
Enhancement CT may detect mesenteric vessels engorgement and abnormal bowel-wall enhancement in case of vasculitis.
Bowel ischemia may present altered enhancement and submucosal oedema.
We can find trans-mural hypertrophy and a fibrotic reaction in the bowel wall in case of endometriosis.
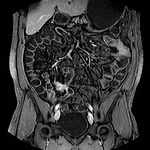
INFECTIOUS COLITIS (Fig 1):
There are many causes of infectious colitis that include Shigella,
Salmonella,
Yersinia,
Staphylococcus, histoplasmosis,
herpesvirus,
cytomegalovirus,
and many other.
Amebiasis and tuberculosis can also cause a colitis,
which can resemble inflammatory bowel disease.
At CT,
patients with infectious colitis from any cause typically have wall thickening,
which usually demonstrates homogeneous enhancement.
Ascites or inflammation of the pericolic fat may also be present.
Multiple air-fluid levels may be present in the colon due to increased fluid and fluid feces.
Speaking specifically:
-Yersinia causes mucosal ulceration,
neutrophil invasion,thickening of the ileal wall and nodular mucosal pattern of the terminal ileum.
The ulcers are mostly uniform in size and shape in contrast to CD.
-Tuberculosis is characterized by asymmetric wall thickening and the common feature of enlarged necrotic lymph nodes.
The ileum is the most commonly-affected site,
either in isolation or with the involvement of the adjacent bowel segments,
especially the cecum.
Depending on the stage of the disease,
findings may range from normal appearance to small polyps or nodules to extensive ulcerations,
hypertrophic,
ulcerohypertrophic and fibrotic lesions resulting in strictures,
causing bowel obstructions and fistulae formations.
In CD lymphadenopathies are frequent,
but they never show necrotic inner core.
Peritoneal involvement can be seen on TBC (in the form of peritoneal caseous nodular implants).
-Clostridium difficile causes thickening of the colonic wall,
which may be circumferential or eccentric.
In general,
the amount of bowel wall thickening in pseudomembranous colitis is greater than in any other inflammatory or infectious disease of the colon except Crohn disease; this is a helpful differential poin.
At CT,
the wall thickening is often irregular and shaggy and in patients with pseudomembranous colitis,
the bowel wall may have low attenuation due to edema or may enhance significantly after intravenous administration of contrast material secondary to hyperemia.
-typhlitis is characterized by intramural bacterial invasion without a specific inflammatory reaction.
This eads to ileo-cecal thickening,
sometimes associated with fat stranding,
oedematous thickening and induration of the caecal wall.
The presence of intramural attenuation due to hemorrhage and/or pneumatosis may aid in correct diagnosis.
The inflammation can be so severe that transmural necrosis and perforation may occurs,
that’s the reason why,
when it is suspected,
CT should be preferred to endoscopy,
because of the higher risk of perforation.
-Anisakis causes violent and relatively acute epigastric or abdominal pain by penetration of larvae through the stomach or lower small intestine mucosa,
especially the ileum.
Chronic infection may provoke an eosinophilic granulomatous response in the ileocecal region,
causing masses with obstruction,
or may produce nonspecific abdominal symptoms.
-Histoplasma capsulatum causes GI involvement,
characterized by diarrhea,
weight loss,
fever,
and/or abdominal pain.
Patients may also have GI bleeding,
bowel perforation,
or obstruction from ileocecal masses or enlarged retroperitoneal lymph nodes.
It characterized by segmental or continuous superficial mucosal ulcerations with erythema or edema,
to deep ulcers with or without frank perforation.
Intraabdominal lymphadenopathy is seen on CT in two thirds of patients.
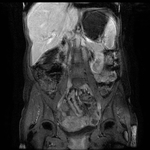
PRIMARY INTESTINAL LYMPHOMA (Fig 2): Small bowel lymphoma originates in the lymphoid follicle of the submucosal layer,
tends to be a large and soft tumor and may present as a solitary form,
that tends to encircle the boweland,
and a diffuse form that shows multisegment involvement with terminal numerous polypoidal excrescences.
These excrescences may be detected,
together with rare ulcerations of the affected bowel loops with formation of a fistulous tract,
thus leading to a more difficult differential diagnosis.
VASCULITIS: Vasculitis represent a rare cause of ileitis and they are characterized by abdominal pain,
nausea,
vomiting,
diarrhea,
and GI bleeding.
Plain radiographic studies may reveal nondiagnostic findings such as segmental bowel dilation,
air-fluid levels,
“thumbprinting” or narrowing of the lumen,
and pseudoobstruction.
Contrast-enhanced CT may show engorgement of mesenteric vessels (comb sign),
multisegmental areas of symmetric bowel thickening,
abnormal bowel-wall enhancement (a double halo or target sign),
and ascites.
BOWEL ISCHEMIA: Ischemic colitis results when blood flow to the colon is compromised,
usually as a result of hypoperfusion and vasospasm of the splanchnic arteries.
In patients with colonic ischemia,
contrast-enhanced CT typically reveals patent mesenteric vessels and circumferential,
symmetric wall thickening with fold enlargement,
and a double halo or target sign may also be present.
The wall may demonstrate low attenuation due to edema or high attenuation,
which indicates intramural hemorrhage.
Furthermore ancillary findings may be present like transmural hemorrhage or transmural/portal pneumatosis.
RADIATION ENTERITIS: Radiation therapy can result in injury to the colon which manifests as pain,
diarrhea,
tenesmus,
and rectal bleeding.
Acute radiation injury to the small intestine and colon occurs during or within a few weeks of radiation exposure and is characterized,
at CT examination,
by nonspecific wall thickening,
peri-enteric fat reaction ,
perirectal fibrous tissue,
and as well as possible complications such as strictures and fistulas.
In these cases clinical history is diriment.
DRUG-RELATED ENTERITIS: The largest number of drug-related reactions are associated with NSAIDs treatments and in severe cases leads to mucosal inflammation,
ulceration and diaphragmatic strictures.
There are often multiple,
2-3 mm thick septae,
and they can noticeably reduce the intestinal lumen caliber.
These diaphragm strictures are thin and easily missed on enteroclysis,
where they may resemble plicae circularis.
Other drugs that may cause ileitis include oral contraceptives,
ergotamine,
digoxin,
and enteric-coated hydrochlorothiazide with potassium.
ENDOMETRIOSIS: Endometriosis is defined by the presence of endometrium outside the uterus,
and most commonly involves nulliparous women 25 to 45 years of age.
This insidious disease can cause intestinal obstruction,
and the diagnosis is often made postoperatively.
The muscularis propria is involved,
there is a marked transmural hypertrophy and a fibrotic reaction in the bowel wall,
leading to bowel segmental narrowing.
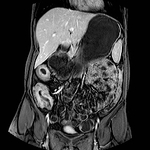
EOSINOPHILIC GASTROENTERITIS (Fig 3): Eosinophilic gastroenteritis (EG) is a rare disorder characterized by prominent eosinophilic infiltration of the GI tract in the absence of known causes of eosinophilia (eg,
parasitic infection,
malignancy,
and drug reaction).The proposed pathogenesis is alteration in the mucosal integrity,
resulting in localization of various antigens in the gut wall,
thereby inducing tissue and blood eosinophilia.
Radiographic changes are variable,
but may show bowel wall thickening,
obstruction,
or ascites.
Ileal strictures and bowel obstruction may occur with muscle layer involvement,
and eosinophilic ascites manifests if the serosa is affected,
furthermore diffuse enteritis with complete loss of villi,
submucosal edema,
and fibrosis may be present.
Multiple biopsies are required because of the patchy nature of the disease,
and full-thickness surgical biopsies may be necessary if disease is confined to the muscle layer.
ILEITIS ASSOCIATED WITH SPONDYLOARTHROPATIES: Spondyloarthropathies (SpA) are characterized by inflammation of axial joints,
asymmetric oligoarthritis,
and enthesitis.
In most cases inflammation is subclinical and escapes detection unless colonoscopic biopsy is warranted by symptoms.
The histologic appearance of lesions is either acute or chronic,
and is not related to disease duration.
The acute form is mainly seen in patients with reactive arthritis and mimics bacterial ileitis (preserved architecture and neutrophil dominance).
The chronic form is more prevalent in AS and undifferentiated SpA,
and may be indistinguishable from CD (disturbed mucosal architecture,
irregular and blunted villi,
distorted crypts,
and lymphocyte dominant).
In some cases,
aphthoid ulcers and sarcoid-like granulomas are present.