Ectopic Pregnancy
Although transvaginal US is the gold standard modality,
it may occasionally be difficult to image the implantation site.
Therefore,
the MR can contribute for a more accurate diagnosis.
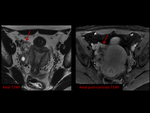
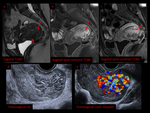
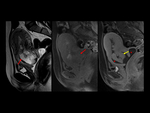
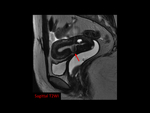
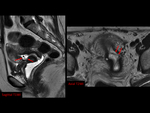
MRI findings of ectopic pregnancy (EP) include gestacional sac-like structure,
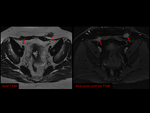
an adnexal or abdominal hematoma,
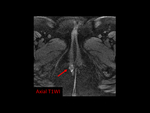
tubal dilatation due to hemosalpinx,
and tubal wall enhancement.
The ectopic gestacional sac (GS) is defined as a round or oval cystic structure with low signal intensity on T1WI and high signal intensity on T2WI,
and may present fresh hemorrhage areas.
Contrast-enhanced MRI has also been reported to be useful for the diagnosis of EP because it demonstrates enhancement in the GS and the affected tubal wall
The differential diagnosis of a GS is the corpus luteum cyst.
On MRI,
the distinction may be facilitated by focusing on the signal intensity of the peripheral area,
location (intra-ovarian or extra-ovarian),
and enhancement pattern.
A corpus luteum images as an intraovarian cystic-like structure with a thickened wall and homogeneous enhancement.
Although a GS also images as a cystic-like structure,
it usually locates extra-ovarian and the dot-like enhancement pattern is specific for a GS.
EP locations:
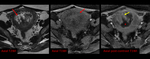
1) Tubal Pregnancy: Approximately 98% of ectopic pregnancies occur in the fallopian tubes,
with the ampullary portion being the most common location,
followed by the isthmus.
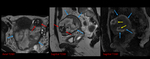
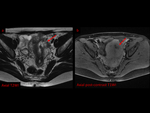
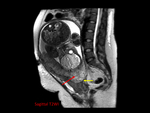
The finding of a dilated tubal wall is another key MRI finding: this is suspicious for a tubal pregnancy and may reflect increased vascularity of the tubal wall following implantation.
A small amount of hemorrhagic fluid can be observed as a localized adnexal hematoma and is not necessarily indicative of tubal rupture. Fig. 5 Fig. 6 Fig. 7
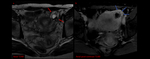
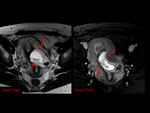
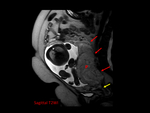
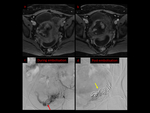
2) Non-tubal Ectopic Pregnancy: Nearly two percent of all ectopic pregnancies become established in other areas including cornual,
ovarian,
cervical,
cesarian scar or intra-abdominal region. Fig. 8 Fig. 9
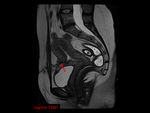
3) Heterotopic pregnancy: A GS inside the uterus and another outside of the structure.
Gestational Trophoblastic Disease
Results from the abnormal proliferation of trophoblastic tissue and encompasses a wide spectrum of diseases.
The MR imaging appearance of it is nonspecific,
and differentiation between its various types is limited.
MR imaging features include a sharply marginated or ill-defined mass centered within the myometrium that distorts or displaces the junctional zone.
Such a mass is usually isointense on T1-weighted images and hyperintense on T2-weighted images,
relative to the normal myometrium,
with avid enhancement after intravenous administration of gadolinium contrast material. Fig. 10 Fig. 11
Placenta Previa
Placenta previa occurs when placental implantation in the lower uterine segment results in partial or complete covering of the internal cervical os.
Types of placenta previa:
- low-lying placenta: lower placental edge is within 2cm from the internal os.
- marginal previa: placental edge extends to the margin of the internal os,
but does not cover it.
- complete previa: placenta completely covers the internal os. Fig. 12
- central previa: the midportion of the placenta completely covers the internal os.
Placenta Accreta Spectrum Disorder
Placenta accreta vera,
placenta increta,
and placenta percreta represent a continuum under the broader category of placental accrete spectrum disorder.
In placenta accreta vera,
chorionic villi attach to but do not invade myometrial tissue.
In placenta increta,
villi invade partially though the myometrium,
and in the most severe form,
placenta percreta,
villi penetrate through the entire myometrial thickness and may extend through the serosa into adjacent structures. Fig. 13
Retained Products
Retained products of conception (RPOC) are a common and treatable complication after delivery or termination of pregnancy.
The pathologic diagnosis of RPOC is made based on the presence of chorionic villi,
which indicates persistent placental or trophoblastic tissue.
The imaging findings of RPOC overlap with the diagnostic pitfalls which include scar ectopic,
pseudo aneurysms,
true arteriovenous malformations,
invasive moles,
blood clots and sub involution of placental implantation site. Fig. 14 Fig. 15
Uterine Arteriovenous Malformation
Uterine arteriovenous malformation (AVM) consists of a proliferation of vascular channels with fistula formation and an admixture of small,
capillary-like channels.
The size of these vessels can vary considerably.
They are classified as congenital or acquired.
The latter is more common and is often described as a uterine arteriovenous fistula.
MR imaging is a non-invasively method to diagnose uterine AVM.
Multiple serpentine flow-related signal voids are typically seen in the uterine wall,
endometrial cavity,
and parametrium on T1 and T2 weighted images.
Contrast-enhanced dynamic MR angiography can depict complex serpentine abnormal vessels that enhance as intensely as normal vessels and show early venous return. Fig. 16
Post-partum Scar Complications
Uterine Dehiscence: characterized by incomplete rupture of the uterine wall,
usually involving the endometrium and myometrium but with an intact overlying serosal layer. Fig. 17
Cesarean Scar Defect/ Niche: In some women,
there is tethering of the endometrium in the region of the old cesarean scar,
creating a potential reservoir or “niche” that accumulates fluid or blood. Fig. 18 Fig. 19
Endometrial Implants: Abdominal wall endometrial implantation is estimated to occur in 0.03%–1% of patients who undergo cesarean delivery.
On average,
there is a 3.6-year delay between the inciting surgery and the development of symptoms from abdominal wall endometriosis. Fig. 20 Fig. 21