Normal Pregnancy Imaging Findings
The radiologist must be familiar with normal gravid uterus,
adnexa and placental anatomy in order to recognize pathologic conditions.
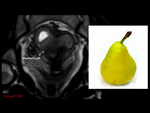
The normal gravid uterus has an inverted pear-shape appearance,
with the fundus and body being wider than the lower uterine segment.
The uterine contour is usually smooth with no focal bulges.
The myometrium normally exhibits a tri-layer appearance on T2WI—the middle layer is thicker and has an intermediate signal,
with multiple flow voids representing the normal myometrial vascularity; it is surrounded on either side by thin low signal intensity inner and outer layers .
As the fetus grows and the normal myometrium thins later in pregnancy,
the tri-layer appearance may not be perceivable; however,
the myometrium should not demonstrate focal bulges or areas of mural disruption. Fig. 1
Gestational sac can be identified at 4.5–5 weeks gestational age using T2 images.
As in ultrasound (US),
the mean sac diameter and gestational sac volume have a significantly correlation with gestational age.
The yolk sac may not be identified on MRI because of image resolution,
whereas it is usually visible at 5–6 weeks on transvaginal US.
While the yolk sac is not seen,
fetal tissue,
either a fetal pole or a more developed fetus with limb buds,
should be seen on MRI when the mean sac diameter measures 1.7 cm,
or if the estimated gestational age is 6.4 weeks or more.
Corpus luteum reaches its maximum size by 10 weeks and involutes by 16-20 weeks.
It can hemorrhage and/or rupture - causing pelvic pain.
It is characterized by a cystic structure with thickened and irregular wall,
and avid rim enhancement,
in the ovary.
Corpus luteum may be morphologically difficult to differentiate from intra-ovarian ectopic pregnancy,
which is exceedingly rare,
however.
The utero-placental interface is normally seen as a thin,
smooth,
uninterrupted and gently curved hypointense interface on T2WI.
The normal placenta has a discoid appearance with gentle lobulations,
and present a fetal and a maternal surfaces.
It attaches to the anterior or posterior aspect of the uterus,
extending onto the lateral walls,
and has homogeneous intermediate signal intensity,
which is usually clearly distinct from the underlying myometrium.
Normal placental septa and linear areas of decreased T2 signal intensity are found running through the myometrium.
The normal subplacental vascularity can be seen as numerous flow voids under the placenta and are usually in the vicinity of the insertion point of the umbilical cord.
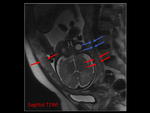
The mid portion of the placenta typically measures between 2 and 4 cm in thickness,
and the placenta undergoes changes during gestation Fig. 2 .
Placental thinning has been described in systemic vascular and hematologic disorders that result in microinfarctions.
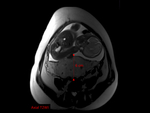
Thicker placenta >4 cm are seen in ante-partum infection,
maternal diabetes,
fetal hydrops and maternal anemia Fig. 3.
Note that placental thickening can be simulated by myometrial contractions and underlying fibroids.
The umbilical cord normally inserts centrally on the placenta,
but can be marginal (inserting less than 2 cm from placental edge) or velamentous (inserting on chorioamniotic membranes rather than directly on placental tissue).
The latter scenario results in umbilical vessels which extend for a variable length between the amnion and chorion and are at risk for injury because they are unprotected by Wharton’s jelly.
Umbilical cord insertion is typically evaluated with second trimester US,
but is also well seen on T2WI.
Normal Post-Partum Imaging Findings
The postpartum period is defined as beginning immediately after the delivery of the infant and placenta and typically is considered to continue for 6–8 weeks as the physiologic changes of pregnancy slowly revert to baseline.
The appearance of the uterus therefore varies according to the time after delivery.
In the early stage the uterine myometrium undergoes contraction to stop bleeding.
This brings the anterior and posterior uterine walls and the decidua (endometrium of the pregnant uterus) together,
thereby forming a thick and possibly irregular stripe.
As the uterus progresses,
there is an evolution of this material within the endometrial cavity with healing at the site of placental insertion and the formation of a new layer of endometrium.
Myometrium has an intermediate and heterogeneous T2W signal intensity due to increased water content.
The normal zonal anatomy often is restored after about 6 months post-partum.
On the other hand,
the zonal anatomy of the cervix persists in the post-partum period.
The content of the endometrial cavity may be variable in amount and appearance: the presence of T2W hyperintensity was consistent with retained fluid: blood or lochias (blood in 64% of cases).
Endometrial fluid usually resolves after 1 week.
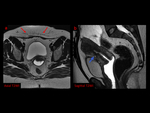
It is of equal importance to appreciate the normal appearances post-cesarean section. The appearance of the scar is variable and depends on hemoglobin degradation stage and edema.
A hypointense oval-shaped structure at the site of incision or just next to the site of incision presumably corresponds to a hematoma.
A common pitfall is to misinterpret normal post-cesarean appearances as a collection,
hematoma or other pathological findings. Fig. 4