This is a single centered retrospective study in a cohort of 16 patients,
9 males and 7 females,
during the last 12 months,
between 54-82 years old with ascites who underwent image – guided hepatic biopsy in order to be determined the cause oh hepatic failure and to diagnosed a focal hepatic lesion or diffuse impairment of the hepatic parenchyma.
Each patient was fully informed over the necessity of the biopsy,
the procedure and the possible complications.
A written consent from each patient was signed.
Common practice includes measurement of the complete blood count,
including platelet count and prothrombin time (PT)/international normalized ratio (INR),
especially in patients with background of cirrhosis and impaired coagulation tests.
Patients that were receiving antiplatelet or anticoagulation medication were recommended to discontinue several to 10 days before the biopsy as antiplatelet medication was concerned,
at least 5 days prior to biopsy for warfarin and heparin/related products were discontinued 12-24 hours prior to biopsy.
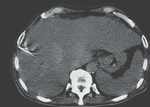
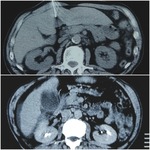
All patients before the CT-guided biopsy were evaluated by ultrasound in order to evaluate the amount and the type of ascites.
The amount of perihepatic ascites was classified as moderate,
sever or slight (<2 cm).
Interventional management,
drainage by placing catheter or without placing catheter was conducted in patients that was necessary so that the biopsy could be performed.
Preliminary 5mm collimation axial slices were obtained to confirm the location of the target lesion,
to determine the optimal entry site of the needle and consequently to select the appropriate patient positioning.
The type of the ascites,
free or encapsulated,
in these patients was a great indicator for detailed mapping and selecting the most suitable position of the patient.
Patients were positioned in the supine,
or lateral decubitus position with the right hand placed gently behind the head in a comfortable position.
A pre – biopsy nonenhanced CT scan (16 multidetector CT scan) in most cases was sufficient regarding the patients who had already undergone diagnostic contrast-enhanced CT.
However,
in cases that it was necessary to delineate anatomical structures in the projected needle path,
intravenous contrast (50-100cc) was injected and the biliary system was identified as well as the great vessels and their branches.
Local anesthesia with 1% xylocaine and antiseptic (povidone iodine-draping) were routinely used with continuous pulse oximetry and noninvasive blood pressure monitoring.
Transmission precautions in the CT suite were taken according to the CDC guidelines.
5 patients had Hepatitis B,
7 had Hepatitis C and one had both.
Depending on the depth of the target lesion we selected a 18/9 or a 18/15 G Tru-Cut ( Cook,
Bloomington Indiana U.S.A )needle.
Due to liver movement we trained out patients concerning breathing during the procedure in order to place the needle in the proper position.
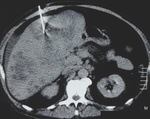
A site with the least amount of perihapatic ascites was selected and the needle was advanced at least 3cm into the parenchyma to minimize the risk of bleeding when considered diffuse biopsy or at the most medial part of the lesion.
When a focal lesion was to be biopsied the shortest pathway was selected.
One needle pass was performed in all patients.
When the procedure ended,
the tissue sample was directly sent to the lab,
while a pathologist was not present in the CT-suite,
a post biopsy scan was performed in order to assess the liver,
vital signs of the patient were obtained.
Post biopsy patients without ascitic fluid lie on their right lateral side to encourage local compression,
however a small sized cirrhotic liver with the presence of ascites does not contribute to the tamponade and the patient’s position post biopsy is not needed to be on the right side of the patient.
However,
a normal sized liver,
whilst the presence of ascites,
on a right lateral side displays the fluid and favours the direct pressure from the abdomen wall towards the site of needle puncture.
The patients were under observation for 24 hours post biopsy.