This is a single centered retrospective study in a cohort of 36 patients referred to our department the last 24 months ( October 2016- October 2018) with a diagnosed mediastinal lesion,
between 32-74 years old,
21 males and 15 females.
32 lesions were located in the anterior mediastinum and 4 in the posterior.
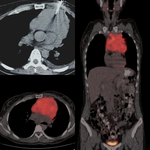
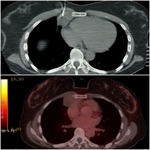
A pre biopsy PET/CT scan was available in 19 out of these 36 patients.
All patients were informed about the necessity of obtaining tissue sample from the lesion,
the procedure of CT – guided percutaneous mediastinal biopsy as well as the potential complications and informed consent was obtained.
Prothrombin time,
partial thromboplastin time and platelet count were assessed for bleeding disorders before the biopsy,
which are included in the exclusion criteria of performing a percutaneous biopsy.
Patients that were receiving antiplatelet or anticoagulation medication were recommended to discontinue several to 10 days before the biopsy as antiplatelet medication was concerned,
at least 5 days prior to biopsy for warfarin and heparin/related products were discontinued 12-24 hours prior to biopsy.
Preliminary 5mm collimation axial slices were obtained to confirm the location of the target lesion,
to determine the optimal entry site of the needle and consequently to select the appropriate patient positioning.
Patients were positioned in the supine,
prone,
or lateral decubitus position depending on the lesion location and the biopsy approach.
A pre – biopsy nonenhanced CT scan (16 multidetector CT scan) in most cases was sufficient regarding the patients who had already undergone diagnostic contrast-enhanced CT.
However,
in cases that required delineation of anatomical structures in the projected needle path,
intravenous contrast (100cc) was injected and mediastinal vessels were identified and differentiated from lymph nodes.
Local anesthesia with 1% xylocaine and antiseptic (povidone iodine-draping) was routinely used with continuous pulse oximetry and non invasive blood pressure monitoring.
Transmission precautions in the CT suite were taken according to the CDC guidelines.
A 16 or 18-gauge needle,
9cm or 15 cm in length ( Cook,
Bloomington Indiana U.S.A ) was used.
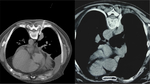
31/32 mediastinal biopsies of the anterior mediastinal lesions were performed using the parasternal approach and the remaining biopsy was conducted via a trans pulmonary approach.
3/4 mediastinal biopsies of the posterior mediastinum were performed using the paravertebral approach and 1/4 using the transpulmonary approach.
The angle and tract of our needle were calculated from the small anaesthesia needle that proceeded for local anaesthesia.
Concerning the parasternal approach,
the patient was in a supine position and the needle was inserted lateral to the sternum,
medially or laterally to the mammary vessels,
through the parasternal muscles and mediastinal fat into the target.
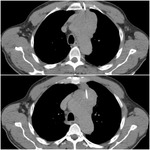
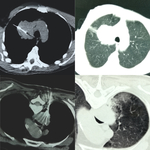
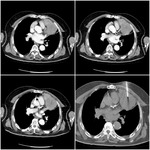
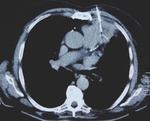
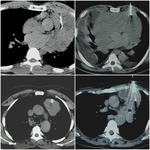
In one case a question arised between parasternal and transpulmonary approach,
due to the presence of subpleural emphysema cysts and the potential risk of pneumothorax,
the parasternal approach was selected (Figure 2).
In the transpulmonary approach,
the needle was slowly inserted through subpleural emphysematous cysts.
The fissures were avoided in order to minimize the risk of pneumothorax.
The paravertebral approach was performed for the lesions located in the posterior mediastinum and all patients were placed in a prone position.
The needle was advanced immediately lateral to the vertebral body between the endothoracic fascia and the parietal pleura.
The intercostal nerve and artery,
the azygos vein,
and the esophagus were avoided [1,4].
A pathologist was not present in the CT suit to evaluate the tissue specimen and the tissue sample was directly sent to the laboratory in formalin solution.
Tissue aspiration guided only by anatomical data can lead to placement of the needle into an area of necrosis and subsequent inadequate tissue sampling with potential false negative results.
However,
the presence and the amount of malignant cells may vary across the target lesion,
whilst the mediastinal lesions may contain solid areas mixed with cystic necrotic or fibrotic areas characterized by the absence of malignant cells [2] .
In our department regarding the patients without a pre-biopsy FDG-PET/CT (17/36) the most solid areas within the lesion was selected and averagely two passes for improving the positive rate of our tissue sample were performed in 13/17 patients.
Current studies assess whether information provided by FDG-PET/CT will decrease the false negative rate and thus improve the accuracy of CT-guided biopsy.
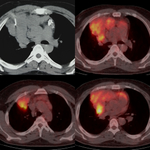
Information with respect to the lesion’s metabolic characteristics are provided in FDG images including differentiation of metabolic from non metabolic areas ( FDG-avid ,
FDG- non-avid).
Moreover,
by PET/CT safer and easier accessible areas with FDG uptake can be revealed and the CT-guided biopsy plan can change.
Tissue sampling of the area with the highest suspicion of malignancy is important to ensure accurate FNB results[2,3].
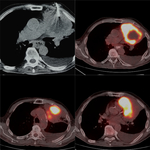
In 19 out of 36 patients a pre-biopsy FDG-PET/CT with time interval of 30 days from the biopsy was available.
The team of radiologists performing the biopsy assessed the data from the PET/CT images,
particularly the areas with the highest SUV max representing the highest metabolic areas and tailored the most appropriate location for needle biopsy.
In all patients a post-biopsy CT- scan was performed in order to evaluate the lung and mediastinum.
The procedure was well tolerated by 35/36 patients,
while a patient with a lesion in the posterior mediastinum,
which proved to be a neuroma,
due to the excessive pain lost consiousness temporarly.
Small area with hematoma of soft tissue was descibed in the needle pathway.
All patients complained of mild post procedural pain and consequently mild shortness of breath with no varietion of pre-biopsy clinical status.
No major complications were reported.
In both patients,
where transpulmonary approach was selected,
on the post biopsy CT scan alveolar haemorrhage was seen along the needle pathway.
The patients were observed after the procedure to ensure their hemodynamic stability and a chest x-ray was obtained immediately and 3-5 hours after the biopsy.