DEFINITION OF PERITONEAL CARCINOMATOSIS:
Peritoneal carcinomatosis is any tumor spread that affects the serosa of the peritoneum and the intraperitoneal organs in a localized or massive way.
Classically,
this disease has been considered an advanced and incurable tumor stage,
treated palliatively and with fatal outcome.
Since the 1980s,
different therapeutic proposals have emerged for these patients,
with intraperitoneal and hyperthermic chemotherapy (HIPEC) offering the most favorable results to date.
VIEWS OF DISSEMINATION OF PERITONEAL CARCINOMATOSIS AS A METASTATIC DISEASE:
- Hematogenous route: main form of dissemination of tumors with a high degree of malignancy.
- Contiguity
- Lymphatic route
- Locoregional spread: due to redistribution and peristaltic movement.
FORMS OF PRESENTATION: findings in the CT.
Ascites: Free or loculated.
Present in 70% of cases.
A loculated ascitis requires ruling out PC.
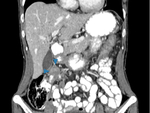
Affectation of the greater omentum: micronodular formations in initial stages to constitute solid and heterogeneous masses in more advanced phases (omental cake).
Fig. 1
Mesentery invasion: Includes attachment of small bowel loops to each other,
thickening of the gastric wall,
involvement of mesenteric fat and formation of small nodules.
Peritoneal implants: Soft tissue lesions with variable appearance depending on their histological origin,
the presence or absence of necrosis,
their location,
the confluence of the lesions and possible previous treatments of the primary tumor.
They can be identified as solid,
cystic,
mixed and / or calcified lesions forming nodules,
masses,
plaques and / or infiltrating lesions.
Fig. 2
Their most frequent locations are: paracolic gutters (right overcoat),
recto-uterine pouch,
sigmoid mesocolon,
ileo-cecal junction in anterior parietal peritoneum.
A festooning of the hepatic and / or splenic surface (which could mimic metastasis),
in the context of a known CP,
suggests involvement of the perihepatic or perisplenic peritoneum. Fig. 3
CALCULATION OF THE PERITONEAL CARCINOMATOSIS INDEX (PCI)
First we must divide the abdomen into 9 quadrants by drawing the following lines Fig. 4 :
- Medioclavicular line,
obtaining two sagittal planes.
- A line that crosses both iliac spines and another line that crosses through the lower region of the rib cage,
thus obtaining two transversal planes.
The abdomen is now divided into nine quadrants that number from 0 to 8,
assessing in each of them the presence or not of nodules / tumor masses.
Subsequently,
each quadrant is punctuated as follows:
0 points: absence of tumor lesions.
1 point: tumor mass <0.5 cm.
2 points: tumor mass> 0.5 cm.
3 points: tumor mass> 5 cm.
We must also assess four more regions:
- proximal jejunum
- distal jéjunum
- proximal ileum.
- and distal ileum.
These regions are numbered from 9 to 12 respectively.
Subsequently,
these regions are valued like the others (0,
1,
2 or 3 points)
The sum of the points of each one of the regions determines the PCI,
obtaining values from 0 to 39 points at the most.
TREATMENT.
Dr.
Paul Sugarbaker described a line of multidisciplinary treatment for patients with PC based on three pillars:
- A radical surgery or cytoreduction,
very aggressive,
including peritonectomies and visceral resections.
- Locoregional chemotherapy directed,
administering it directly in the peritoneum to maximize its effectiveness and aggressiveness.
- Hyperthermia,
at 40-42ºC,
with cytotoxic effects.
Process:
Cytoreductive surgery seeks to reduce the disease in the abdominal cavity to the minimum possible amount.
First,
the tumor stage of the patient is evaluated and the carcinomatosis index (PCI) is obtained by a CT with intravenous contrast. Fig. 5
After surgery,
the presence or absence of macroscopic implants is evaluated according to the following classification:
- CCO: absence,
complete cytoreduction.
- CC1: presence of implants less than 25 mm
- CC2: implants greater than 25 mm.
After the cytoreduction,
four suction catheters are placed,
two subdiaphragmatic and two pelvic catheters,
in addition to another catheter necessary for postoperative chemotherapy.
The central temperature is monitored by means of an esophageal thermometer,
two intraperitoneal thermometers and another additional thermometer that will control the temperature at the entrance of the perfusion.
The abdominal cavity is isolated by means of a bell-shaped plastic and inside there is a fume aspirator that will collect the vapors generated during the perfusion with the chemotherapy.
A hole in said plastic,
will allow the surgeon access and manual control of the distribution of the fluids inside the abdominal cavity.
Infusion with hyperthermia is done for 30-90 minutes.
The flow of the perfusion ranges between 500 and 1000 ml / minute to which the cytostatic agent is added.
The circuit passes through the heat exchanger to achieve a temperature in the input catheter of 43º-44º.
Throughout the procedure there must be a special control and monitoring of the patient's constants.
OUR RESULTS:
We performed a retrospective study of the CT imaging findings of these patients with the results obtained during the surgical procedure.
We describe and localize the peritoneal implants visualized in the CT and later those identified in the surgery comparing both results.
With the results obtained,
a Wilcoxon type statistical study is carried out evaluating:
- the correlation between the radiological PCI / surgical PCI. Fig. 6
- the correlation of PCI in the small intestine.
Fig. 7
- the correlation if the PCI is less than 15. Fig. 8
- the correlation if the PCI is greater than 15. Fig. 9
- the correlation in solid tumors. Fig. 10
- the correlation in non-solid tumors. Fig. 11
Other significant data obtained from the observational study of our patients:
- Micronodular dissemination was the main diagnostic challenge of peritoneal carcinomatosis both by imaging and surgically.
The grouping of micronodules in the peritoneum may go unnoticed in the radiological report,
resulting in a nonspecific finding.
The macroscopic findings of these micronodular groupings during the surgical act are as non-specific as the information provided by the CT.
Only an anatomo-pathological confirmation would confirm the presence or not of tumor disease.
- The size of the implant is inversely proportional to the possibility of being identified on CT.
This statement already described in several studies of peritoneal carcinomatosis has also been observed in our series of cases.
- The subphrenic regions,
especially the left one according to our study,
are regions where the presence of peritoneal implants is commonly overlooked by CT.
However,
these regions are better explored during the surgical act,
identifying implants in these locations not visualized by CT. Fig. 12
- The paracolic gutters and the greater omentum are the areas where least difficulty was found to identify the presence of implants by CT.
No large differences were observed with the results obtained in the surgery.
- The proximity of the small bowel loops to the implants makes it difficult to diagnose using CT.
It was observed that in the surgery implants were identified in this location that were unnoticed by imaging tests. Fig. 13