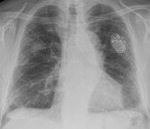
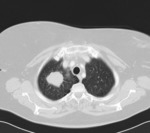
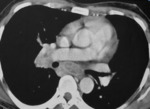
Primary tuberculosis (Figure 1,3,4,5,6)
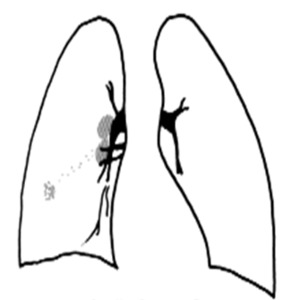
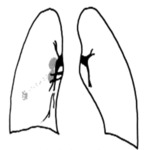
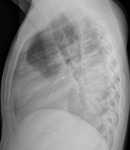
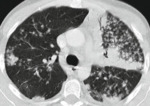
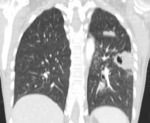
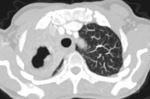
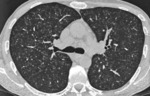
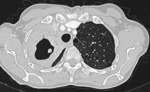
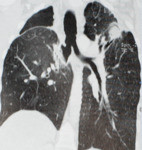
Fig. 1: Primary tuberculosis.
o Round infiltrates and consolidations
o Especially right lung
o Especially basal lower lobe,
middle lobe and anterior upper lobe
o Lymph node enlargement (90 - 95% in children,
10 - 30% in adults)
o Obstructive atelectasis (up to 30%)
o Pleural effusion (5 - 10% in children,
30 - 40% in adults)
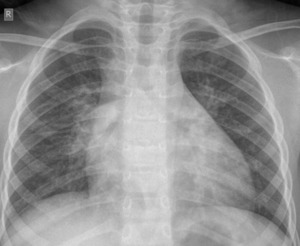
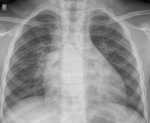
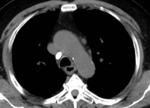
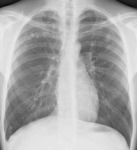
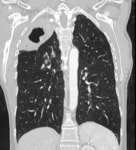
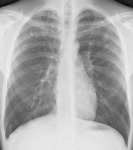
Fig. 3: PA CXR showing RT hilar enlargement secondary to lymphadenopathy, suggestive of primary tuberculosis in 25 month old child.
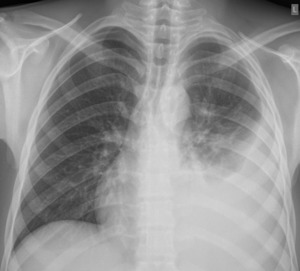
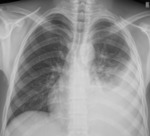
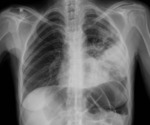
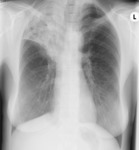
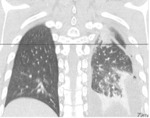
Fig. 4: PA CXR showing Pleural effusion in a 19 years old Patient affected by Tuberculosis.
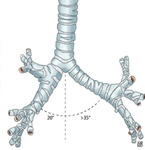
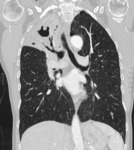
Anatomically the right bronchus bifurcates at an angle of about 70 degrees,
giving a greater volume and respiratory capacity to the right lung. (Figure 2)
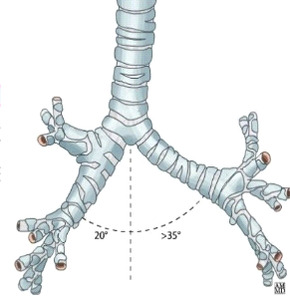
Fig. 2: Bronchial Anatomy
For this reason,
primary tuberculosis,
with round infiltrates and consolidations,
is most frequently found in the right lung,
in the basal portions of the lower and middle lobe and in the anterior segment of the upper lobe.
Residues of primary tuberculosis (Figure 7).
● Calcified lung granulomas
● Grossly calcified hilar or mediastinal lymph nodes
Postprimary Tuberculosis
The term postprimary tuberculosis is generally used to refer to both reinfection with and reactivation of tuberculosis. It occurs in patients previously sensitised to M tuberculosis.
(Figure 8 ).
Characteristic of postprimary tuberculosis
● Caverns,
typically thick-walled
● Signs of endobronchial scattering with tree-in-bud (characteristic of active tuberculosis,
but not pathognomonic) or centrilobular nodules
● Pleural effusion
Typical are centrilobular nodules with a diameter of 2 - 4 mm and branched linear structures ("tree bud sign" or tree-in-bud sign); distinct bronchial wall thickening with or without bronchiectasis.
(Figure 9).
Caverns (Fig.
10,11,12,13)
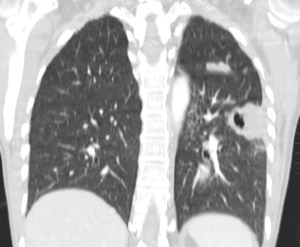
Fig. 10: Cavern links in a patient with pulmonary tuberculosis.
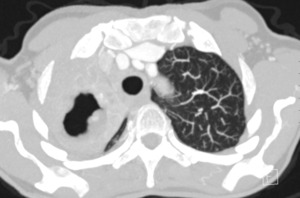
Fig. 13: MIP axial Large TBC cavern in the CT-scan.
● Are an important hallmark of postprimary tuberculosis
● Caused by attachment of a caseating consolidation to the bronchial system
● In 40-45% of patients with post-primary tuberculosis,
one or more cavities are detectable
● Caverns are an important activity marker in patients with tuberculosis
● Are typically thick-walled and irregularly contoured,
less often thin-walled and smoothly bounded
● In 9-21% of patients there is a secretion-air-level in the cavern as an indication of a bacterial / mycotic superinfection
Miliary tuberculosis (Fig.14)
Miliary tuberculosis is an uncommon pulmonary manifestation of tuberculosis.
It represents haematogeneous dissemination of uncontrolled tuberculous infection and carries a relatively poor prognosis.
It is seen both in primary and post-primary tuberculosis and may be associated with tuberculous infection in numerous other tissues and organs (for example,
CNS,
liver,
spleen).
The sputum typically does not show any mycobacteria.
Tuberculomas (Fig.15,
16)
Tuberculomas are detectable in 3 - 6% of patients with post-primary tuberculosis.
Their diameter is 0.5 - 4 cm,
usually it is sharply defined.
Tuberculomas can sometimes be calcified,
typically solitary or may have smaller satellites.
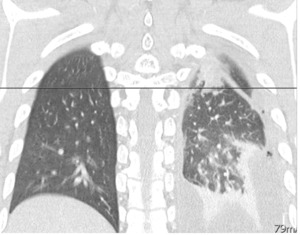
Fig. 16: Tuberculomas. PA CXR.
Differential diagnosis: Excavating bronchial carcinoma (squamocellular or microcellular); Lung abscess; localised pleural empyema; infected emphysematous bullae; cavitary pneumoconiosis; Hiatus hernia; pulmonary hematoma; Hydatid cyst of lung; cavitary infarcts of lung; Wegener’s granulomatosis.
Diagnostic bronchoscopy is a part of diagnostic protocol for taking the material for microbiological examination.
Sputum examination is useful for identification of microbiological agents or confirmation of bronchial carcinoma.
Chronic changes in postprimary tuberculosis (Fig.
17,18)
In up to 40% of patients,
scarring-fibrotic changes are detectable:
● atelectatic structural compaction
● Volume reduction of the upper lobes
● Hilus lift and compensatory hyperinflation of the corresponding lower lobes
● bronchiectasis / parenchymal destruction ("destruction lung")
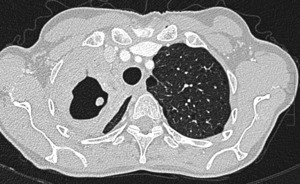
Fig. 17: Scarring-fibrotic changes postprimary tuberculosis CT scan.
After primary infection,
reactivation occurs at about 5% after years.
One risk factor for reactivation is immunosuppression: immunomodulating therapies,
HIV,
or chronic diseases (silicosis,
diabetes,
renal insufficiency,
malignancy,
alcoholism,
cachexia).
Interested are:
Lymph nodes (11%),
pleura (8%),
intrathoracic lymph nodes (6%),
genitourinary tract (4%),
peritoneum (3%),
disseminated tuberculosis (2%),
spinal column (2%),
bone (without water) ( 2%),
CNS (1%) and others (1%).
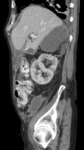
• Kidney:
- 30% bilateral
- Calyx system dilated,
irregularly bounded
- Stenosis,
strictures,
with consecutive ecstasy of the sepals to hydronephrosis.
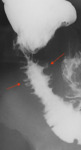
• Ureters:
- descending infection
- Corkscrew-like changes or stenosis and dilatations.
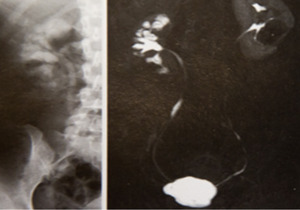
Fig. 19: Patient affected by Tuberculosis.
Bladder - tubercular cystitis:
- reduced volume of bubbles,
- wall thickening
- late stage: calcifications
- DD: toxic cystitis,
DD: bladder carcinoma.
Adrenal gland:
- Very rare.
- Organ enlargement central necrosis,
- 90% bilateral,
- End stage: organ specification.
Penile tuberculosis: very rare.
Penile TB mimics carcinoma penis,
granulomatous penile ulcer,
genital herpes simplex,
inguinal granuloma and HIV infection.
Lymph node (Fig.20)
- common: cervical,
supraclavicular
-rare: axillary,
inguinal abdominal.
-Morphological stages:
1.
Non-specific morphology
2.
Centrally fused,
enlarged lymph nodes with peripheral contrast enhancement.
3.
Cold abscess:
• progressive central necrosis and fusion of individual lymph nodes.
• Unequal thick Contrast-receiving membrane
• Course: increasingly solid and calcifications
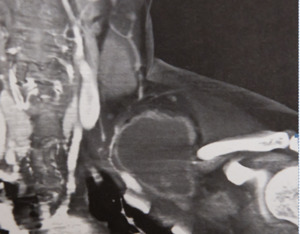
Fig. 20: Patient affected by Tuberculosis.
• Cardiac tuberculosis (0,
5% Cases)
Tuberculosis is rare and affects the pericardium,
causing pericarditis.
Myocarditis rarely occurs,
mostly with a Miliary tuberculosis.
Sometimes we can find pleural effusions,
pericardial calcifications,
dilated V.
cava inferior and a pericardial effusion.
• Tubercular spondylodiscitis (50% of musculoskeletal Tuberculosis cases)
- Morphology:
• the anterior portion of the vertebral body with calcium reduction (early sign) CT!
• the length of the intervertebral disc is preserved
• subligamentous extension along the longitudinal anterior ligament
• discontinuous multisegmental affection
• progressive reduction of the ventral vertebral body
- CT,
MRI.
Investigate whole neuroaxis!
Pott's Disease
Pott’s Disease,
also known as tuberculosis spondylitis,
is a combination of osteomyelitis and arthritis which involves multiple vertebrae.
Clinical Case
81-year-old woman suffered for four months from back pain,
fever to 39 ° C ,
weight loss of 7 kg,
increased flatulence and transient leg edema,
CRP of 132 mg / L.
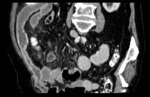
The computed tomography of the abdomen showed a significant destruction from L1 to the base of Th12 (Figure 22).
At the same height there was a paravertebrale,
peripheral contrast-receiving Liquid collection with maximum diameter of 7 x 2.6 cm.
In addition,
enlarged lymph nodes paraaortally left.
(Figure 21).
The most obvious was the finding compatible with spondylodiscitis tuberculosis.
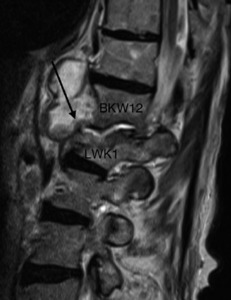
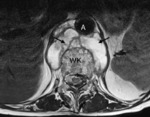
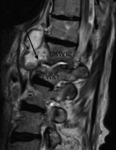
Fig. 22: Destruction of L1 and basis of Th12.
References: Manifestationen der extrapulmonalen Tuberkulose- F Marti, T Bregenzer
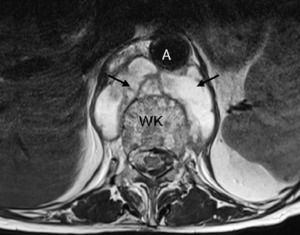
Fig. 21: Aorta (A), ventral fluid collection (Arrows). WK = vertebral body.
References: Manifestationen der extrapulmonalen Tuberkulose- F Marti, T Bregenzer
Tuberculous osteomyelitis
• extremities
• Metaphysis
• Initial osteoporosis -> osteolysis -> low periosteal reaction.
• Clinical differentiation: lack of pain and fever
Tuberculous arthritis:
Weight bearing joints e.g.
knee
• monoarticular affection.
• Morphology:
- Thickening of the synovium
- joint space Reduction.
Joint osteoporosis
- erosion of bare areas
• Tuberculous Peritonitis (Fig.
23)
(30% of all extrapulmonary tuberculosis)
Peritonitis is thought to originate primarily from hematogenous spread; however,
it may be secondary to a ruptured lymph node or gastrointestinal deposit or to fallopian tube involvement.
The condition is subdivided into three main types:
1-Wet Type Peritonitis (90% of cases):
It is characterized by large amounts of free or localized ascites,
which,
at CT,
is usually slightly hyperattenuating (20–45 HU) relative to water due to its high protein and cellular content.
2-Fibrotic Type Peritonitis (60% of cases of peritonitis):
It is characterized by large omental and mesenteric cakelike masses with matting of bowel loops.
At CT,
it manifests as mottled low-attenuation masses with nodular soft-tissue thickening.
Omental thickening and caking can also be seen at US.
Dry Type Peritonitis (10% of cases)
It is characterized by mesenteric thickening,
fibrous adhesions,
and caseous nodules.
Its imaging manifestations are highly suggestive of,
but not specific for,
tuberculosis.
- DD peritoneal carcinomatosis.
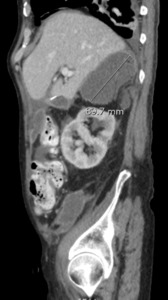
Fig. 23: Wet type tuberculous peritonitis. Contrast-enhanced CT scan shows ascites.
- Additional centered melted lymph nodes and missing malignant diagnosis.
• Material extraction: peritoneum biopsy! Ascites puncture (sensitivity below 20% of cases)
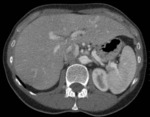
Tuberculosis of the liver
• Morphology:
- forms:
• Micronodular shape
- hepatomegaly
- Micronodular shape partially masked in the sectional imaging.
• Macronodular shape
- Rare
- hepatomegaly
- multiple tuberculomas up to 3 cm
• similar changes in the spleen.
Tuberculosis of the pancreas
Very rare.
Not to be distinguished from pancreatic carcinoma.
Melted lymph nodes peripankreatic
Intestinal tuberculosis (Fig.
26)
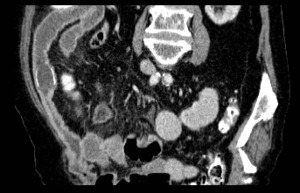
Fig. 26: Patient affected by Tuberculosis. Contrast-enhanced CT scan shows wall thickening in the bowel loops.
• Localisation
- especially in the ilio-coecal transition.
• Morphology
- mucosal irregularities
- circular wall thickening
- Ascites
- lymphadenopathy
- Late stage: fibrosis with intestinal stenosis,
fistulas
• DD: Crohn's disease
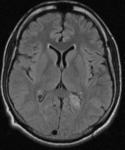
Tuberculosis of the CNS (Fig.
27,
28)
Forms :
- Tuberculous meningitis
• in basal cisterns
• Increased Contrast-Enhancement of the Meninges
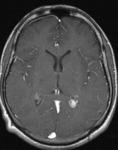
- Tuberculomas or neurotuberculosis
• Measuring from mm up to 4 cm
• often solitary
• CT: hypodense with peripheral contrast enhancement
• MRI: depending on the degree of central necrosis.
Surrounding edema.
• Complications:
- Hypdrocephalus
- Cerebral infarctions
- rarely cerebritis and / or abscesses
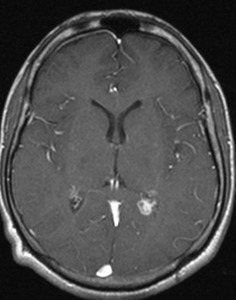
Fig. 27: MRI 24 year old patient affected by Tuberculosis -T1 SE Transversal.
Complications of Tuberculosis
1- Aspergillosis: predisposing caverns and bronchiectasis,
often asymptomatic for years,
hemoptysis,
thickened cavern wall,
thickened pleura.
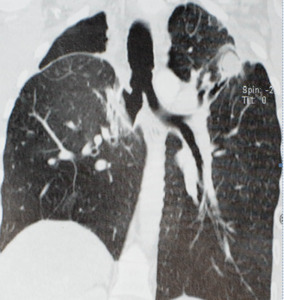
Fig. 29: 43 year old patient affected by Aspergillosis after Tuberculosis Infection.
2- Bronchial Cancer
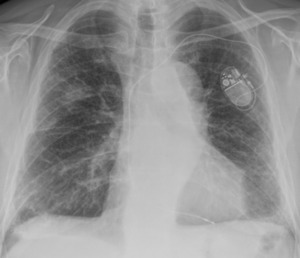
Fig. 30: 55 year old patient presenting Nodules in the Lung after a Tuberculosis Infection when he was 33.
Course of tuberculosis under therapy
• Regression mostly after 3 months
• Recovery period may take months to years
• lymphadenopathy can persist over years
• in case of missing therapy response -> suspected Multi Drug Resistant Tuberculosis
Tuberculosis in HIV affected Patients
• HIV: 50-200 times higher risk
• atypical courses e.g. Consolidations bds.
• Lymphadenopathy
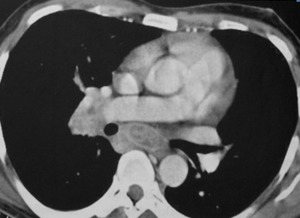
Fig. 32: 37 year old HIV affected patient with Lymphadenopathy, after diagnostic was confirmed Tuberculosis Infection.
- Lymph nodes border with contrast enhancement in HIV patients -> Tuberculosis suspicion!