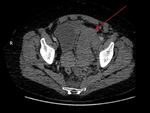
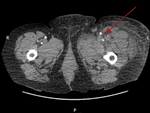
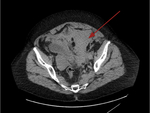
All cases had confirmed retroperitoneal haemorrhage on CT over a three year period.
All three cases where left sided in middle aged females.
None of the patients received anti-coagulation treatment before the SRH was diagnosed.
In all three patients,
there were no clear aetiology of the SRH,
with no indentifiable risk factors for developing SRH.
Case 1: 70 year old female
PC: Left leg swelling and mottled,
hypotensive and left iliac fossa mass
Ultrasound in ED by a non-radiologist revealed a non-compressible left common femoral vein and a left iliac fossa mass.
A DVT suspected and was treated with antiocoagulation.
The next day the patent developed hypotensive shock and a CT demonstrated a large RPH.
The patient was started on unfractioned heparin with close monitoring of clotting function and haemodynamic stability.
An IVC filter was also inserted.
The patient was resuscitated and remained haemodynamically stable for the rest of her admission,
she was discharged home with anticoagulation 9 days later.
A repeat CT showed no change in the haematoma.
Case 2: 60 year old female
PC: Severe left iliac fossa and left leg pain.
Hypotensive shock and weak peripheral pulses.
A ruptured abdominal aortic aneurysm was suspected in ED,
a CT angiogram showed a large left RPH.
Duplex confirmed a left ileo-femoral DVT.
The patient was started on tranexamic acid and an urgent IVC filter was inserted.
The patient was admitted to critical care.
3 days after admission she was haemodynamically stable and started on anticoagulation,
with careful monitoring of Hb and clotting.
The patient was discharged home 13 days after admission on a divided anticoagulation regime.
It was noted from an old CT pelvis,
that the patient had prominent peri-vesical varices in a similar location to the RPH.
It was postulated an obstructing clot could increase pressure within a variceal collateral,
that could lead to spontaneous bleeding.
Case 3: 57 year old female
PC: Severe left iliac fossa pain and hypotensive.
The patient had a raised lactate of 5.3.
Differential diagnosis in ED were ruptured ovary or ureteric colic.
The patient soon developed shock and a CT was requested which showed a large left sided RPH.
The patient continued to deteriorate with a HB drop and hypotensive shock. The patient was transferred to the interventional suite for a diagnostic angiogram.
No active bleeding was identified.
Her left leg was becoming increasingly swollen,
a bedside duplex showed a left femoral DVT.
Due to persistent hypotension despite resuscitation,
the surgical team performed a diagnostic laparotomy.
1.2L haematoma was evacuated and the cavity was packed.
No clear source of bleeding was identified,
but presumed venous.
2 days after surgery an IVC filter was inserted.
The patient remained haemodynamically stable and anticoagulation was commenced.
She was discharged home 16 days after admission.
The patient developed post thrombotic syndrome as a sequela.