Keywords:
Cancer, Computer Applications-Detection, diagnosis, MR, Neuroradiology brain, CNS, Artificial Intelligence
Authors:
M. D. Patel1, J. Zhan2, K. Natarajan1, R. Flintham3, N. Davies 3, P. Sanghera1, A. Peet1, V. Duddalwar4, V. Sawlani1; 1Birmingham/UK, 2Qingdao/CN, 3Birmingham /UK, 4Los Angeles/US
DOI:
10.26044/ecr2019/C-2003
Aims and objectives
Background
Assessment of treatment response in brain tumours is one of the most important issues in oncology.
After chemo-radiotherapy (CRT),
glioblastoma,
the most common aggressive primary brain tumour,
increases in size in one third of patients.
It appears that treatment is not working and in about half of these cases,
the growth is transient and due to treatment itself,
known as ‘pseudoprogression’,
rather than true progression.1 In clinical practice,
it is impossible to differentiate between true progression and pseudoprogression.
Conventional MRI scans also cannot distinguish between the two (Fig. 1).
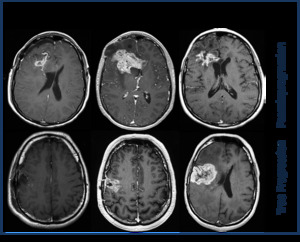
Fig. 1: Examples of pseudoprogression and true progression in two patients. At the first follow-up MRI scan at six weeks after chemo-radiotherapy treatment, there is an increase in enhancing disease. At this time it is impossible to differentiate between the two pathologies. Scans at 6-9 months make the distinction.
Computer vision can be used to read images of tumours and detect hundreds of features invisible to the human eye,
known as ‘radiomics’.2 Machine learning can also be used to create a prediction model from the features and clinical data to predict clinical outcome.3
Aim
The aim of this pilot study was to see if we could use computer vision to identify radiomic features,
not visible to the human eyes,
to distinguish between early true progression and pseudoprogression in glioblastoma.