All the images have been collected in a prospective way from the 15th of May 2018 till the 30th of September 2018 from the selected patients of Greek origin between 19 and 73 years old presenting to the emergency department with the clinical suspicion of appendicitis.
All the relevant images were obtained by a 64-slices computed tomography scanner and an ultrasound device.
HELICAL COMPUTED TOMOGRAPHY
In case of clinical suspicion of appendicitis,
helical CT scan of the abdomen including pelvis is the most conservative and popular imaging technique.
Administration of intravenous and oral contrast agents is typically used and beneficial.
The severity of radiological findings is strongly dependent on the time passed from the onset of symptoms and the clinical status of the patient.
Vermiformis appendix with no signs of inflammation appears as a tube filled with fluid,
contrast,
air or bowel content.
The fat tissue around the organ is normally homogenous and the wall thickness does not exceed 2 mm.
In order to diagnose an active appendicitis in CT,
it is mandatory to visualize the abnormal appendix and evaluate its size,
quantity and quality of the periappendicular fat and caecal changes (ileocaecal bowel opacification).
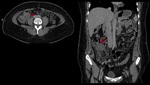
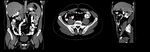
The CT findings that support the diagnosis of an active appendicitis are listed below [6] :
- external diameter of the appendix > 6 mm - symmetric thickening of the wall on the scans with IV contrast - mural stratification (frequently manifested in a form of a target sign)
- local thickening of fascia
- focal apical caecal thickening
- the arrowhead sign (contrast medium due to the blockage of appendix can collect at the upper part of the caecum in a shape of an arrowhead) [7]
Recognition of some secondary sign scan be assisting in establishing the final diagnosis as their presence positively correlates with the likelihood of inflammation.
Among them the following can be distinguished: identified fecaliths,
periappendiceal free fluid,
complex collections,
enlarged prominent lymph nodes,
phlegmon,
etc [7].
For unexperienced radiologists,
it is important to be aware that the presence of phlegmon or abscess in the abdominal right lower quarter are strongly suggestive but not pathognomic of appendicitis.
ULTRASONOGRAPHY
It is believed that US scan of the right lower abdominal quadrant requires more skills and experience.
Nevertheless,
the criteria for the US-based diagnosis of acute appendicitis are well established and reliable [8].
Assuming that appendix is identified,
sonographic examination has been found to have strong positive predictive value reaching up to 100% in detecting appendicitis [9].
For the radiologists in training,
who have not developed their own way of performing the sonographic examination yet,
it is advised to start the US scan in the transverse plane by starting from the tip of the liver and continuing until they encounter the pelvic brim.
It might be required to change the scanning plane medially or laterally.
The US exploration begins ideally with curvilinear and is followed by the linear transducer as the latter can provide more detailed images [6].
Graded compression US techniques are highly advised in the exploration of the right lower quadrant.
They are based on the hypothesis that normal and gas-filled loops of gut will be either displaced from the field of view or compressed whilst the inflamed appendix will not react to compression.
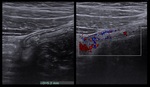
Severity of inflammation seems to be associated with the increase of blood flow through the bowel wall,
which can be detected by Color Doppler US.
Because of constant peristaltic movements of the intestine,
blood flow detection in the uninflamed bowel wall is more challenging.
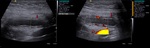
Identification of the appendix can be confirmed when a blind-ended,
tubular structure that arises from the base of the caecum is seen during the sonographic examination.
Inflammation of the appendix can be suspected if the organ is identified to have laminated wall and its external diameter exceeds 6mm.
Among other sonographic findings strongly suggestive of appendicitis we can distinguish: presence and increase of intramural blood flow,
non-compressibility and lack of peristalsis [6].
All the assisting signs like periappendiceal fluid identification,
increase of number and/or size of lymph nodes and the change in the quality of the fat tissue,
must be thoroughly described in the radiological report.