EPIDEMIOLOGY
In our center,
during January 2014-December 2018,
237 patients (50 women; 187 men; average age of 79 years) were diagnosticated for HCC and registered in tumors registry of the Region of Madrid.
An average of 40 HCC is diagnosed per year.
In these five years 30% have died and 59% remain alive.

Fig. 1: An average of 40 HCC is diagnosed per year.
References: Department of Radiology, University Hospital Puerta de Hierro Majadahonda/ES
DIAGNOSIS
In cirrhotic patients,
the diagnosis was based on imaging criteria.
Multiphasic CT or MR with extracellular contrast (late arterial phase,
portal venous phase,
and delayed phase) was used.
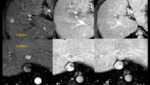
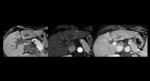
HCC in a cirrhotic liver has a typical pattern: hypervascularity in late arterial phase and washout on portal venous and/or delayed phases.
We can also find regenerative or dysplastic nodules.
In our center,
and with the aim of standardizing reports and improving communication between radiologists and clinicians,
we follow the LI-RADS algorithm.
We use it progressively since 2014-2015 and established in an way since 2016.
LI-RADS is used for diagnosis and staging of HCC in patients with cirrhosis,
viral infection due to hepatitis B,
chronic hepatitis current, previous HCC and candidates for liver transplantation and post-transplant recipients with HCH.
The LI-RADS system assesses contrast dynamics, presence of the capsule and the growth of the tumor over time.

Fig. 2: CT/MRI Diagnostic Table. CT/MRI LI-RADS®v2018
References: CT/MRI LI-RADS®v2018
LI-RADS categorizes the lesions according to the probability of HCC (LR2,
LR3 and LR4 corresponding to low,
intermediate or high probability of HCC).(Fig. 4)(Fig. 5)

Fig. 3: CT/MRI LI-RADS®v2018 Categories
References: Department of Radiology, University Hospital Puerta de Hierro Majadahonda/ES
The findings,
treatments,
protocols of actions and follow-up are individualized and discussed weekly by a multidisciplinary committee.

Fig. 6: CT/MRI LI-RADS®Based Management: Suggested Imaging Workup Options &
Time Intervals
References: CT/MRI LI-RADS®
The multidisciplinary committee decided to perform biopsy to 85 HCC.

Fig. 7: CT/MRI allows definitive diagnosis of 64% HCC without biopsy
References: Department of Radiology, University Hospital Puerta de Hierro Majadahonda/ES
With the systematic use of LI-RADS since 2016 in our center,
we observed a tendency to decrease the number of biopsies performed for the diagnosis of HCC.
In relation to the number of HCC diagnosed,
the number of biopsies has decreased in the last two years.

Fig. 8: Relating the number of HCC, the number of biopsies has been reduced in the last three years.
References: Department of Radiology, University Hospital Puerta de Hierro Majadahonda/ES
Restrospectively,
all HCH diagnosed with biopsies since 2014 and without categorization LI-RADS were reviewed:
-91% They were cataloged as LI-RADS4 and LI-RADS5.
-9% LI-M (lesions probably or definitely malignant,
but not an appearance compatible with HCC).
The LI-M,
suggested other differential diagnoses: adenomas,
hyperplasias,
cholangiocarcinoma,
metastasis of neuroendocrine tumors.
In non-cirrhotic livers,
HCCs are diagnosed by biopsy and LI-RADS is not used.
These lesions are characterized by larger lesions,
have less typical behavior and other diagnoses are proposed.
Since the use of the LI-RADS system,
the biopsy recommendations are submitted to a multidisciplinary committee. LR-4,
LR-M,
and LR-TIV (thrombus in the vein) lesions are susceptible to biopsy.
In our center,
the isolated biopsies performed in Li-RADS 5 have been made to analyze molecular markers in case of change of treatment or inclusion in clinical trials.
In the last year,
we have analized the response to treatment according to LI-RADS.
STAGING AND TREATMENT
For the staging and treatment the patients are discussed and individualized in a multidisciplinary committee based on the Barcelona-Clinic Liver Cancer Staging System [BCLC] attending to:
-Tumor (number and size of nodules,
presence of vascular invasion,
extrahepatic dissemination)
-Liver function (bilirubin,
portal hypertension,
liver function preservation)
-Health status (classification of the Eastern Cooperative Oncology Group [ECOG] and presence of symptoms)
Very early CHC (BCLC 0):
| Prognostic stage |
Treatment |
Survival |
| 1 solitary tumor <2 cm |
-Resection
-Ablation
|
Five years in 80 to 90%
|
| No vascular invasion / or satellite injuries |
| ECOG-0 |
| Well-preserved hepatic function (Child-Pugh class A). |
Ablation:
-Radiofrequency ablation (RFA): the heat produces coagulative necrosis in the tumor and the periphery,
that creates a "safety ring" in the peritumoral tissue,
which could eliminate the undetected small satellites.
-Microwave ablation (MWA): uses electromagnetic energy that heats the tissue but the periphery is less involved by heat. Advantage: in near lesions to vascular structures.
-Ethanol injection: where thermal ablation is not technically feasible,
in tumors <2 cm.
Complete necrosis in 90% but high rate of local recurrence.
They can be used by laparoscopic approach.
Resection and the radiofrequency ablation (ARF) are similar in terms of results,
with more life expectancy and life expectancy adjusted for quality at a lower cost in favor of ARF.
ARF could become the first line option even in surgical patients.
To evaluate the resection, multiparameter are valued,
but the most important are: liver function assessment,
degree of portal hypertension,
extend of hepatectomy and surgical invasiveness.
Macrovascular invasion is a contraindication of liver resection (LR).
Stereotactic body radiotherapy (SBRT): emerging modality under investigation.
It has been studied as a combination with TACE or as a bridge for liver transplantation in the early stage of inoperable hepatocellular carcinoma.
Early HCC (BCLC A):
| Prognostic stage |
Treatment |
Survival |
| Single tumors > 2 cm* or three nodules <3 cm |
-Liver transplant (LT)
-Local ablation
|
50% to 70% five years after resection
|
| ECOG-0 |
| Preserved liver function |
*Unique tumors> 5 cm and RM pre-operative without macrovascular involvement,
portal pressure and bilirubin normal: surgical resection is the first option.
Criteria of Milan Transplant (Fig. 9)
Single tumors ≤5 cm or three nodules ≤3 cm.
Tumor vascular invasion and extrahepatic metastases are contraindication for liver transplant.
The use of pre-trasplant (neoadjuvant) loco-regional therapies is recommended in LT candidates.
Neoadjuvant treatment can be applied as "bridging" treatment (candidates for transplant on the waiting list),
or as "downstating" treatment (to try to include patients whose tumor burden is outside the accepted criteria for transplantation).
HCC intermedio (BCLC B):
| Prognostic stage |
Treatment |
Survival |
| Multinodular asymptomatic tumors without vascular invasion or extrahepatic involvement |
TACE |
49% at two years |
| Preserved liver function |
| ECOG 0 |
The definition of intermediate HCC includes a wide range of patients according to liver function and tumor burden.
-Large multifocal CHC affecting both lobes,
without vascular invasion or extrahepatic disseminations associated with cancer-related symptoms: stadium BCLC C and D.
-Child-Pugh A-B may include patients with refractory ascites,
spontaneous bacterial peritonitis,
hyponatremia or recurrent encephalopathy.
In these cases: liver transplantation.
-If it exceeds the accepted criteria for transplantation: BCLC D.
TACE (Transcatheter arterial chemoembolisation)
Intraarterial infusion of a cytotoxic agent and embolization of the blood vessels that nourish the tumor.
Usually,
it use of drug-releasing beads (adriamycin,
doxoricicin or epirubicin)
TACE should not be used in patients with decompensated liver disease,
advanced hepatic and / or renal dysfunction,
hepatofugal flow,
macroscopic vascular invasion or extrahepatic dissemination.
Although it can be performed safely in patients with thrombosis with selective treatment.
After the initial success of TACE,
tumors can recur (re-vascularization).
The procedure can be repeated. Do not repeat when there is no necrosis in two consecutives TACE,
when there is no necrosis in the sites where they have progressed,
or in progression that prevents new treatment.
(Fig. 10)
Transarterial Radioembolization with Yttrium-90 (TARE):
The infusion of radioactive substances such as microspheres containing yttrium-90 (Y90) (isotope that emits ß) in the hepatic artery.
The subgroup of patients who benefit from TARE should be defined: downsize and/or bridge patients to liver transplant, alternative to TACE, or HCC with portal vein thrombosis.
A preliminary angiogram was performed,
where 99Tc macroaggregated albumin was injected into the hepatic artery.
Computed tomography with single-photon emission of macroaggregated albumin was used to calculate the dose needed for treatment,
the dose for the adjacent liver,
the fraction of hepatopulmonary derivation and the distribution of yttrium.
(Fig. 11
Severe pulmonary shunting and extrahepatic uptake contraindicate the procedure.
The treatment can be used in patients with portal vein thrombosis.
Advanced CHC (BCLC C):
| Prognostic stage |
Treatment |
Survival |
| Symptomatic tumors |
Sorafenib |
25% per year |
| Macrovascular invasion (segmental or portal invasion) |
| Extrahepatic dissemination (involvement of the lymph nodes or metastasis) |
| Preserved liver function |
| ECOG 1-2 |
Systemic treatment: sorafenib, multi-tyrosine kinase inhibitor.
Regorafenib: second line
Under study (Lenvatinib,
Cabozantinib)
End-stage HCC (BCLC D):
| Prognostic stage |
Treatment |
Survival |
| End-stage liver function |
Best supportive care
|
11% at year
|
| ECOG 3-4 |
Patients with end-stage disease has very poor performance status (ECOG 3-4) that reflects a severe tumour related disability.
Palliative treatment.
Their median survival is 11% at one year.
In our centre the number of Radiofrecuency Ablation (RF),
Microwave Ablation (MW),
Transarterial Chemoembolization (TARE),
transarterial radioembolization (TARE) and Steroatactic body has increased.
The number of liver transplants and surgical treatment has decreased.
In 2014,
4 liver transplants were performed for HCC; In 2017,
only one and none in 2018.
The number of Radiofrequency Ablation (RF),
Microwave Ablation (MW),
Transarterial Chemoembolization (TARE),
Transarterial Radioembolization (TARE) and Stereotactic Body Radiation Therapy (SBRT) has increased.
Six patients have been treated with SBRT,
2 of them in combination with other treatment (TACE,
TARE,
MW) and 4 as initial treatment.

Fig. 12: Number of RF,TARE,TACE, SBRT have increased. The number of liver transplants and surgical treatment has decreased.
References: Department of Radiology, University Hospital Puerta de Hierro Majadahonda/ES
In non cirrhotic liver,
surgery has been the treatment of choice (Fig. 13)