The first step in diagnosis is stratifying risk by differentiating simple and complex cysts.
- Simple cysts have: Thin,
smooth walls and may contain up to two septae.
- Complex cysts have: Septated,
mural irregularity or nodularity,
debris,
calcification,
and fluid levels.
(Table 1 -2)

Table 1: Distinguishing charateristics of simple and complexe cysts.
References: Marianna G. Mavilia et al. (2018) Differentiating Cystic Liver Lesions: A Review of Imaging Modalities, Diagnosis and Management: Journal of Clinical and Translational Hepatology vol. 6 | 208–216.

Table 2: Apprearance of simple versus complex hepatic cysts with various imaging modalities
References: Marianna G. Mavilia et al. (2018) Differentiating Cystic Liver Lesions: A Review of Imaging Modalities, Diagnosis and Management: Journal of Clinical and Translational Hepatology vol. 6 | 208–216.
-
The simple cyst includes developmental lesions:
o Simple cyst:
A benign,
congenital,
and developmental lesion derived from biliary endothelium that does not communicate with the biliary tree.
Multiple,
round or ovoid structures without a perceptible wall.
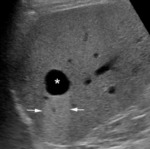
§ US: oval or rounded lesion,
anechoic,
with regular well-limited margins and posterior strengthening.
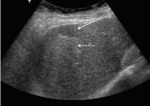
(Fig 1)

Fig. 1: US: Right hepatic simple cyst (Star)
posterior strengthening (Arrow)
References: M.Wagner et al. (2017) Hepatic fluid abnormality. Elsevier Masson
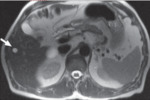
§ CT and MRI: Simple cysts have attenuation (0–15 HU) and signal intensity (T1 hypo-intensity,
T2 hyper-intensity) similar to water.
Simple cysts do not show enhancement after injection of contrast materiel.
[5] (Fig 2,3 )

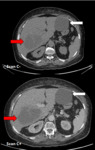
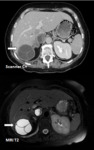
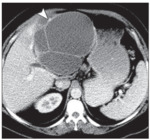
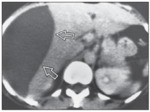
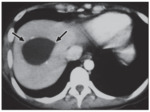
Fig. 2: CT scan without and with injection:
White arrow: Left hepatic rounded lesion, hypodense, with regular well-limited margins enhancing after injection. (Simple cyst)
Red arrow: Right hepatic rounded lesion, iso to hypo attenuating compared with background liver on the unenhanced phase and has a peripheral rim of enhancement on administration of IV contrast material. (Abces)

Fig. 3: T2-weighted MR image in 45-year-old woman shows homogeneously hyperintense simple hepatic cyst (arrow).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
Asymptomatic: no treatment is needed
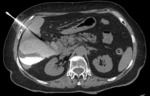
Symptomatic: percutaneous drainage with sclerotherapy (Fig 4),
surgical resection.

Fig. 4: CT Scan: percutaneous drainage with sclerotherapy
o Biliary hamartoma:
Rare and asymptomatic lesion.
Benign malformation of the biliary tract.
Found incidentally on autopsy or at laparotomy.
§ US: Multiple small well-circumscribed lesions with echogenicity depending on components.
(Fig 5)
§ CT: Multiple hypo-attenuating lesions (< 1.5 cm) with regular margins.
The density of the lesion depends on the relative amounts of cystic and solid components.
Predominantly cystic lesions show no contrast enhancement.
MRI: Hypo-intense on T1-weighted imaging and hyper-intense on T2-weighted imaging.
Predominantly cystic lesions show no enhancement after gadolinium,
whereas predominantly solid lesions enhance.

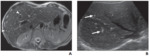
Fig. 5: Biliary hamartoma in 35 years old woman.
A: Axial T2-fat-suppressed MR image shows innumerable tiny hyperintense round lesions (arrowheads) throughout liver.
B:Transverse ultrasound image of liver shows multiple echogenic foci with comet-tail artifact (arrows).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
o Caroli disease:
This entity is rare,
benign and asymptomatic.
It is manifest with saccular dilatation of large intra-hepatic bile ducts as multiple intrahepatic cysts of varying sizes that communicate with the biliary system usually the left lobe.
(Fig 6)
§ CT and MRI: The lesions are cystic and usually have a central enhancing component,
the “central dot” sign,
which is the portal radical.
(Fig 7)
§ Thin-section CT: Show communication between the Caroli cysts and the biliary tree.
MRI confirms the communication with biliary system with contrast agent.

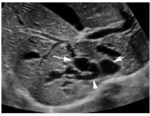
Fig. 6: US: (Caroli disease) Multiple cystic dilations (arrow) that communicate with dilated bile ducts (arrowhead).
References: M.Wagner et al. (2017) Hepatic fluid abnormality. Elsevier Masson

Fig. 7: Caroli disease in 35-year-old man.
Contrast-enhanced portal venous phase CT scan shows saccular dilations of biliary tree (arrowheads) with enhancement of central portal vein radicals (“central dot sign”) (arrows).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
o Polycystic liver disease:
Polycystic liver disease is a rare and its cause is mal-development of the ductal plate that affects the small intrahepatic bile ducts.
[7]
An autosomal-dominant condition can be associated with autosomal-dominant polycystic kidney disease (50% of these patients).
The majority of patients are asymptomatic.
§ US: Multiple intrahepatic cysts peripherally located and vary in size.
The peribiliary cysts are typically small (< 10 mm) and have a periportal distribution.
(Fig 8)
§ CT: A fluid level,
wall thickening,
calcification,
or internal gas.
§ MRI: The best modality for identifying cysts complicated by hemorrhage or infection.

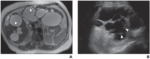
Fig. 8: Autosomal dominant polycystic disease in 40-year-old man with known polycystic liver disease.
A: Axial T2-weighted single-shot fast spin-echo image shows numerous cysts of varying sizes throughout liver.
Peripheral incomplete and thin septations (arrowheads) are seen within several cysts. Kidneys are normal.
B: Transverse ultrasound image of liver shows multiple anechoic cysts with thin echogenic septations (arrowheads).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
o Ciliated foregut duplication cyst:
A ciliated hepatic foregut duplication cyst is a rare congenital cystic lesion that is thought to arise from the embryonic foregut.
Asymptomatic and incidentally discovery.
Given the reported risk of malignant transformation,
ciliated hepatic foregut duplication cysts that are symptomatic,
are enlarging,
are larger than 4 cm,
or contain atypical features (e.g.,
solid components,
thick septations) should be resected (level of evidence of III and IV).
[8]
§ US: A small lesion less than 3mm in segment IV,
anechoic or hypoechoic lesion.
(Fig 9)
§ CT- MRI: The density depends on the serous or mucinous content.

Fig. 9: Example of ciliated cyst in a woman 76 years old. Ultrasound finds a hypoechoic lesion (arrow subcapsular with posterior reinforcement (dashed arrow).
References: M.Wagner et al. (2017) Hepatic fluid abnormality. Elsevier Masson
·
The complex cyst include: Inflammatory,
neoplastic,
trauma-related lesions.
o Inflammatory or Infectious Cysts:
§ Pyogenic and amebic abscess: Diagnosis is based on clinical and biology information.
The difference in imaging between the two types of diagnosis remains very minimal (Fig 2-10).
Clinically: Fever,
hepatomegaly,
right hypochondrium pain.
· US: Anechoic mass well-defined or indistinct borders and with increased through-transmission and may contain echogenic debris or gas.[2]
· CT: Iso to hypo attenuating compared with background liver on the unenhanced phase and has a peripheral rim of enhancement on administration of IV contrast material.
A “double-target” sign may also be evident but it is not specific for a pyogenic source.
[2]
·
MRI: Hypo intensity on T1,
hyper intensity on T2; with hyper intensity in T2 around the lesion indicating edema.
§ Fungual microabscess: Principally small (< 2 cm) and disseminated lesions in liver and spleen.
· US: hyperechoic round lesion with hypoechoic peripheral ring “bull’s eye”.
· CT: Tri-phasic liver imaging: Most lesions being detectable on the arterial phase.
The portal venous phase: hypo attenuating with a ring enhancing appearance,
or may be uniformly hyperenhancing.
[9]
· MRI: Micro abcess hyper intense on T2 weighted imaging.

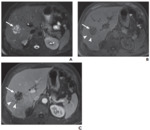
Fig. 10: Hepatic abscess with septic
thrombophlebitis.
A: Axial T2-weighted fat-sat MRI shows multiloculated hyperintense lesion in right hepatic lobe, consistent with abscess (arrow).
B and C: Axial unenhanced (B) and contrast-enhanced (C) T1-weighted spoiled gradient recalled echo images show abscess (arrow) to be hypointense to liver parenchyma, with enhancement of rim and internal septations. Adjacent hepatic venous branches (arrowheads) did not enhance, representing septic thrombophlebitis of hepatic vein adjacent to abscess.
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
§ Hydatid Cyst:
· Round,
uni or multilocular,
tonic lesion.
Usually finding calcifications ring.
(Fig 11-12)
Anechoic on US,
hypo attenuation on CT and hypo T1 hyper T2 on MRI.
The classification of Gharbi is established according to its characteristics.

Fig. 11: Hydatic cyst Type II of Gharby classification.
US: fluid formation anechoic, rounded, with detachment of the proliferous membrane (Arrow)
Scanner C+: rounded, well-defined hypodense lesion of the right liver with detachment of the proliferous membrane (Arrow)

Fig. 12: Multilocular hydatic hepatic cyst type III of Gharby classification.
o Neoplastic lesion:
§ Biliary Cystadenoma and Cystadenocarcinoma:
·
Rare tumor,
it develops from the bile ducts
· Large lesion multilocular with fine septations,
enhancing walls and calcification.
· The morphology can mimic that of pyogenic abscess,
amebic abscess,
or cystic metastasis,
and knowledge of clinical information is paramount for providing the correct diagnosis [2] (Fig 13)

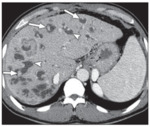
Fig. 13: Biliary cystadenoma in 47-year-old woman.
Contrast-enhanced CT scan shows multiseptated
cystic lesion in left lobe of liver. Note focal papillary
excrescence (arrowhead).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
§ Cystic Hepatocellular Carcinoma:
· Rare atypical form of hepatocellular carcinoma.
· Clinically: fever and leucocytosis.
· Radiologically: The lesion mimics the appearance of the abscess.
On CT: An irregular multilocular hypo attenuating lesion with a peripheral rim of enhancement [2].
(Fig 14)

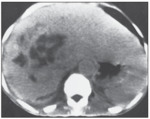
Fig. 14: Cystic hepatocellular carcinoma in 60-year-old man with known hepatocellular carcinoma. CT
scan shows multiple low-at tenuation masses in liver.
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
§ Cyst metastases:
· Many cystic tumors may metastasize to the liver (e.g.,
pan-creatic or ovary cystadenocarcinomas).
Other liver metastatic lesions which can appear cystic usually originate from rapidly growing hypervascular tumors (sarcoma, melanoma, and neuroendocrine tumors) and appear so due to necrosis and cystic degeneration [10]
· On ultrasound,
CT,
and MRI,
cystic metastases appear as solitary or,
more commonly,
multifocal lesions with complex features,
such as thick,
irregular,
enhancing walls; thick or nodular septations; mural nodularity; or internal debris[5] (Fig 15)

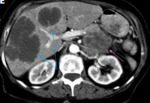
Fig. 15: computed tomography image: Showing two large cystic-appearing liver lesions (light blue arrows) in a case of a metastatic pancreatic cystadenocarcinoma that is also evident (pink arrow)
References: A. Bakoyiannis et Al (2013). Rare cystic liver lesions: A diagnostic and managing challenge.
o Trauma-related lesion:
§ Hepatic hematoma:
The collection of bile,
lymph,
or blood products after injury to the liver parenchyma will result in the formation of a biloma,
se-roma,
or hematoma,
respectively [12].
· On CT:
o Recent bleeding: Hyperdensity
o Chronic bleeding: Hypodensity
· On MRI: The chronology of the hematoma and its methemoglobin content conditions the MRI signal.
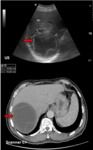
(Fig 16)

Fig. 16: Subcapsular hematoma
CT scan shows well-circumscribed elliptical area of hypodensity (arrows) in periphery of right lobe of liver.
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
§ Biloma:
· On US,
CT and MRI: Well-defined cystic lesion oval or rounded,
without a clean wall,
not raised and not vascularized.
(Fig17)

Fig. 17: Intrahepatic. CT scan shows well-circumscribed fluid-density collection within liver (arrows).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
o Miscellaneous Lesions:
§ Peribiliary cyst:
· Multiple single cysts isolated or grouped around portal and intrahepatic bile ducts.
§ Intrahepatic pseudocyst:
· A rare complication of acute alcoholic pancreatitis.
· On imaging,
Cystic lesion with a raised fine capsule.
(Fig 18)

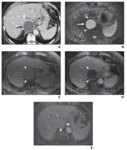
Fig. 18: Pseudocyst related to prior episode of pancreatitis in 45-year-old man.
A: Axial contrast enhanced CT image of liver shows round low attenuation lesion centered in subcapsular region of caudate lobe (arrow). Mass has thick peripheral rim (white arrowhead) and adjacent inflammatory fat stranding (black arrowheads).
B: Axial T2 fatsat shows homogeneous hyperintensity within cyst (arrow), with mildly hyperintense peripheral rim (arrowheads).
C and D: Axial unenhanced (C) and contrast-enhanced (D) T1-weighted images show cyst (arrow) to be hypointense to hepatic parenchyma with no internal enhancement, although there is peripheral rim enhancement (arrowheads).
E: axial contrast-enhanced T1-weighted obtained 3 months later shows near-complete resolution, with only minimal residual hyperenhancement in parenchyma of caudate lobe (arrowheads).
References: B.Vachha et al. (2011) Cystic Lesions of the Liver. AJR; 196:W355 –W366
The diagnosis of liver cyst is depending on the number of lesions and their dissemination.
The present of a wall,
the internal structure of the lesion,
particularly the MR signal and the proximity of the biliary tree are the main diagnostic criteria.
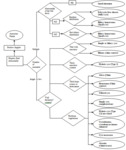
The ultrasound algorithm used to progress to diagnostic hypotheses is as follows: (Fig 19)

Fig. 19: Hepatic cystic abnormalities.
References: M.Wagner et al. (2017) Hepatic fluid abnormality. Elsevier Masson