Procedure
Contraindications are the severe coagulopathy,
communication between cyst and biliary tract or peritoneal cavity,
and incapacity to recover the contrast medium from the cyst.
Conscious sedation is generally achieved with intravenous midazolam and fentanyl,
under constant hemodynamic monitoring.
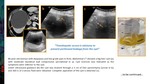
Typically the cyst is punctured under sonographic guidance,
and an 8 to 10F pigtail catheter is inserted into the cyst,
through 1-3 cm of liver tissue to prevent leakage from the cyst,
via the Seldinger or trocar technique,
as far as possible into the cyst.
All of the fluid is aspirated and a sample may be sent for Gram stain,
culture,
and cytology (Fig1).
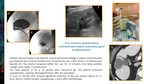
Once complete aspiration is obtained dilute contrast (equivalent amount as the alcohol used) is injected through the catheter under fluoroscopic or CT guidance,
to exclude leakage of fluid into the peritoneum or communication with blood vessels or the biliary system.
If any of these findings are present,
sclerotherapy is contraindicated,
especially the biliary system to avoid irreversible sclerosing cholangitis (Fig 2).
Injected contrast medium must be aspirated before sclerosing agent is administered,
otherwise sclerotherapy is contraindicated.
Multiple agents for sclerotherapy have been used including ethanol,
tetracycline,
minocycline,
and doxycyline.
However,
the most commonly used sclerosant is ethanol because it is readily available,
inexpensive,
and generally well tolerated.
10% of the aspirated cyst volume is replaced with 95-99% ethanol.
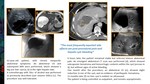
Ethanol causes protein denaturation,
cell death,
and inflammatory fibrosis after contacting the cyst wall (Fig 3).
Therefore,
contact with the entire cyst wall during treatment is desirable.
In order to ensure that,
the patient is rotated from prone to supine,
and right to left lateral decubitus positioning.
We maintain the patient for 3 minutes in each position,
leaving the alcohol in the cyst cavity for 12 minutes in cases of less than 1 liter of cystic volume; in larger cysts subsequent injection in the session is advised.
The maximum volume of ethanol should be limited to 100 mL in adults in order to avoid alcohol toxicity from systemically absorbed alcohol.
If the volume of the cyst is over 1L,
we use two step approach (Fig 3).
The alcohol should be completely aspirated; the cyst may be irrigated with saline to reduce leakage of ethanol during catheter withdrawal,
even though not routinely.
Complete evacuation documentation before removal of the catheter is advised.
Post-procedural rest is indicated and if asymptomatic the patient is discharged the same day.
Follow-up imaging should be performed in 3,
6 and months after the procedure.
Subsequent cyst sclerosis may be necessary,
especially if the cyst remains symptomatic.
Complications with alcohol sclerosis include pain,
which is usually secondary to leakage of alcohol into the peritoneum,
as well as the standard risks of bleeding (Fig 5),
infection,
and injury to adjacent organs.
If pain is encountered during injection,
10 to 15 mL of lidocaine can be instilled into the cyst cavity.
Particularly in cases where sclerotherapy is being performed via transperitoneal access routes,
care should be taken to be certain that 100% of the alcohol has been aspirated from the cavity prior to catheter removal.
This maneuver helps to decrease the likelihood of the intraperitoneal spread of alcohol,
which can cause very severe and difficult-to-control pain.
Finally,
many commercially available drainage catheters are not compatible with ethanol,
which can cause severe degeneration of the catheter.
Confirmation of alcohol compatibility must be made prior to placing the drainage catheter.