Besides its age-old uses,
there have been innovative successful single case or short case series studies to demonstrate its role in lesser known pathological conditions.
HEAD AND NECK
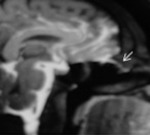
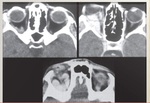
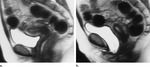
CSF leaks- In CT cisternography,
after obtaining initial pre-cisternogram images and confirming cranial flow of contrast material,
the patient is asked to perform Valsalva maneuver that can exacerbate the leak and repeat CT is performed.[2]All methods of cisternography—radionuclide,
CT,
and MR—provide improved or optimal CSF fistula detection when the fistula is active and when a Valsalva maneuver is added to the imaging protocol(fig-2).
Alternatives- Any provocative maneuver that can exacerbate leak- sneezing,
head hanging followed by direct coronal images in prone position.
Neuroradiology- Patients with significant carotid artery stenosis display altered flow dynamics in the distribution of the middle cerebral artery ipsilateral to the carotid disease during a forced Valsalva.The Valsalva maneuver significantly increases the sensitivity of Trans-cranial doppler and may obviate the need for more invasive neuroangiographic studies.
Also used during nuclear medicine studies to assess asymmetric cerebral blood flow due to AVMs or intracardiac shunts.[3]
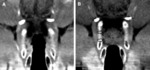
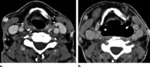
Local staging of malignancies in para-glottic space- Better evaluation of para-glottic fat planes and lesions in sub-glottis since vocal cords are in mid-line and sub-glottis is air filled(fig-3).As an adjunct in the assessment of vocal cord mobility
Alternatives- 'eee' phonation for evaluation of sub-glottic spread of lesions,
distension of pyriform fossa and laryngeal ventricle.
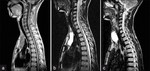
Anterior neck masses- Better visualisation of internal/external jugular or angular/facial venous ectasia or aneurysms and to differentiate them from laryngoceles.
Occasional herniation of thymus/ lung apex into neck due to weakened cervico-thoracic facia,
after performing valsalva in dynamic CT/MRI scans.(fig-4)
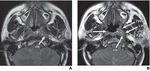
Eustachian tube dysfunction- In patients with nasopharyngeal carcinoma,
it has been used in conjunction with functional MRI,
to know the extent of involvement and functionality of eustachian tube and surrounding soft tissue by the tumor.[4](fig-5)
ORBITS
Orbital varices- Large varices having communication with venous system distend with maneuvers that cause increase in venous pressure.
On colour doppler imaging,
there is retrograde flow of blood towards the transducer when the intra-orbital pressure is increased,
cessation of colour flow when maximum distension is reached and antegrade flow when valsalva is stopped.
On CT, enlargement of enhancing vascular mass as compared to the resting state in supine position.(fig-6)
Alternatives- coughing,
forward flexion,
jugular vein compression, prone belly position.
GASTROINTESTINAL SYSTEM
Esophageal anatomy and disorders- On barium esophagogram,
for demonstration of normal vestibule,
Schatzki ring (by increasing the diameter of associated hiatal hernia),
Sliding hiatal hernias(due to increased intra-abdominal pressure),
esophageal varices,
pulsion diverticula,
gastroesophageal reflux.
However,
provocative maneuvers have controversial role in specificity of diagnosing significant reflux.
Alternatives- prone RAO,
deep inspiration for Schatzki rings; water siphon test,
coughing,
straight leg test for GERD; prone RAO,
single small sips of barium for varices,
buscopan for varices.
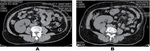
Sonographic evaluation of difficult to visualise organs- Best technique for visualisation of left kidney is having person perform a Valsalva maneuver while in supine position.
Also for evaluation of spleen and pancreas.
Alternatives- RPO position in cases of spleen and kidney; sitting upright,
standing,
rolling patient onto either side,
filling the stomach to create a window and placing the patient in LPO for pancreas.
Abdominal and groin hernias- Used for better delineation and characterisation of defect and contents in barium studies, USG,
CT scan or ultra-fast MRI.
Useful in occult hernias or obese/post-herniorrhaphy patients.
Movement of fat on Valsalva maneuver is more likely an Indirect hernia than Direct hernia.To differentiate canal of Nuck hydrocele from inguinal hernia.
Alternatives- Controlled Valsalva like maneuvers such as-'blowing out cheeks with mouth closed',
'tensing up stomach',
'raising head from pillow' rather than coughing,
which is less controlled.
Postural maneuvers- prone or lateral decubitus positioning.(fig-7)
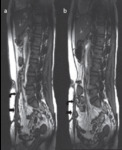
Intra-abdominal adhesions- By functional cine-MRI it is possible to study the bowel movement brought about after Valsalva maneuver.
In case of adhesions,
the movement of bowel loop will be altered (in and out movement in plane perpendicular to direction of movement) and limited by non-variable structure like peritoneum.(fig-8) A direct sign of adhesions is distortion of adjacent organs and small bowel loops on Valsalva.[5]
Extra-hepatic CBD obstruction-Normally,
the Valsalva maneuver may decrease the size of the CHD at the level of the portal vein greater than 1 mm.
This change in diameter of the duct during the Valsalva maneuver may be caused by compression by the liver at the level of the portal vein where the CHD is intrahepatic.
The increased pressure in the CHD associated with extrahepatic biliary obstruction probably prevents this change during Valsalva.
CHEST (Uses in Doppler echocardiography have been omitted)
Atrial appendages and ventricular aneurysms- Before the popularisation of echocardiography and CT,
left ventricular aneurysm on chest X-ray was detected as outward bulge along left cardiac border on Valsalva maneuver due to increase in intra-luminal pressure.It has also been an effective means of demonstrating diseased left atrial appendages,
not otherwise visible ,
in rheumatic heart disease patients.
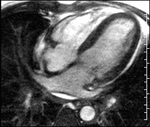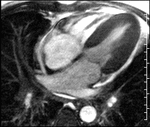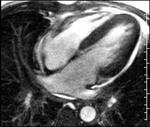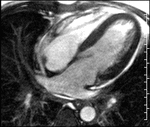
Patent foramen ovale-The MRI depiction of PFO is dependant upon the demonstration of flap-like membrane in the region of the fossa ovalis and or the real-time demonstration of flow during perfusion imaging traversing the inter-atrial septum.
Small field-of-view cinematic GRE sequence targeted to the interatrial septum during employment of valsalva maneuver can reveal a flap-like membrane in the region of the fossa ovalis consistent with a patent foramen ovale.
4-chamber cinematic GRE sequence also acquired with the employment of valsalva confirms this finding(fig-9).
[6]
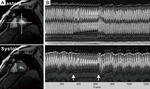
As a stress test in patients with diastolic dysfunction - Real-time cardiac MRI with T1 contrast (3 T,
33 ms) of a patient with diastolic dysfunction during Valsalva maneuver,
i.e.,
increased intrathoracic pressure demonstrates reduced systolic and diastolic myocardial movements as well as alterations of wall thickening(fig-10).[7]
Slipping rib syndrome- It is pain produced by impingement of an intercostal nerve between 2 costal cartilages secondary to luxation of an interchondral articulation.
Sonography combined with valsalva manever can demonstrate that an overlapping movement occurs first,
followed by a sudden slipping in depth of the lower rib,
with shearing stress,
due to contraction of abdominal wall muscles.
PHLEBOLOGY
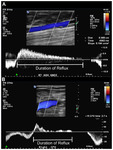
Assessment of venous reflux- Venous reflux,
is the reverse venous flow secondary to venous valvular incompetence during >0.5 s in the superficial venous system or >1 s in the deep system(fig-11) The Valsalva maneuver is considered ‘‘positive’’ when during the straining phase a reverse flow is elicited from the CFV to the GSV (or other superficial veins of the thigh),
due to incompetence of the terminal valve (TV) of the SFJ (or junction recanalization) and "negative' in the absence of reverse flow.[8-1]
Detailed analysis of SFJ- In assessing the SFJ hemodynamic status,
Valsalva maneuver is able to analyse several conditions and different hemodynamic behaviours when compared to distal maneuvers.[8-2]
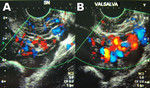
Pelvic vein incompetence- In the presence of pelvic vein incompetence,
it may be useful during abdominal or transvaginal DUS assessment.
It can differentiate between pelvic varices due to extrinsic compression (on the renal vein or iliac vein) – in which the flow is continuous and does not change during strain – from those due to ovarian or internal iliac vein incompetence,
in which the flow increases during straining(fig-12).[8-3]
Indirect evidence of deep venous thrombosis- In response to a Valsalva maneuver,
a normal vein dilates to more than 50% of its original diameter as a result of impaired venous drainage upstream from the area sampled,
whereas veins with acute thrombus do not.
Lack of appropriate response to Valsalva may indicate thrombosis in IVC or pelvic veins,
and is generally limited to assessment of CFV,
which is sufficiently large to demonstrate calibre changes.[8-4]
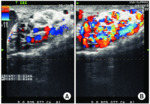
Extra and Intra-testicular Varicocele- Multiple veins >3.0 to 3.5 mm with concomitant reversal of flow after Valsalva maneuver is the most widely used criteria for diagnosing a varicocele on scrotal colour doppler ultrasound(fig-13).The detection of varicocele is more precise with the patient in the standing position,
and the Valsalva maneuver has a greater role in dilation of the pampiniform plexus in the standing position than in the supine position.
Secondary varicoceles due to venous obstruction will be unchanged on provocative maneuvers.
Descending Venography- A valsalva maneuver will assist the retrograde flow of contrast as far as competent valves allow.[8-5]
URO-GYNECOLOGY
Genito-urinary fistulas- Increased intra-abdominal pressure can cause contrast to opacify the fistulous tract and delineate communication between urinary bladder/rectum and vagina when a suspicious communication is not demonstrated on delayed phase of contrast CT abdomen/conventional fistulography.(fig-14)
Cysto-sonography for Vesico-ureteric Reflux- Valsalva produces an increased intra-abdominal and intravesical pressure that mimics the voiding effort and represents an effective approach to demonstrate the presence of VUR.
[9]
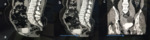
Pelvic Organ prolapse and Obstructed Defecation syndrome- During dynamic trans-perineal sonography or dynamic MRI,
can be used to demonstrate rectocele,
enterocele and inferior descent of the anorectal junction,
bladder base,
and vaginal vault, rectal intussusception and dyssenergic defecation.[10-1]
Urinary dysfunction- Dynamic MR pelvis with rectal contrast is superior to MR defecography in investigation of involuntary leakage of urine,
frequent urination,
urgency,
straining to void,
incomplete voiding,
splinting,
or digital maneuvers to void.(fig-15).[10-2]
MISCONCEPTIONS
- Many definitions and proposed techniques of performing Valsalva maneuver have been described in literature.Originally described as forceful expiration against closed nostrils and mouth in order to increase intra-thoracic pressure that is transmitted through the open glottis to the oro-nasopharyngeal cavity.
During expiration,
abdominal and pelvic floor muscles contract to increase intra-abdominal pressure and to push diaphragm upwards.
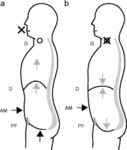
- However,
glottal closure is an essential part of 'abdominal straining' which reflects an inspiratory pattern causing diaphragm to contract and flatten downwards,
abdominal muscles to contract against a relaxed pelvic floor.
- Both Valsalva and abdominal straining maneuvers lead to increased intra-abdominal and intra-thoracic pressure,
but during Valsalva,
pelvic floor muscles contract, preventing descent of pelvic organs by elevation of the pelvic floor.
During straining,
pelvic floor muscles are eccentrically contracted and relaxed in order to initiate,
maintain or improve voiding and defecation.(fig-16)
- Valsalva maneuver should also be differentiated from held deep inspiration.
In males,
both supine and standing,
the mean intra-abdominal pressure is significantly higher during straining than during Valsalva maneuvre.
In females it is significantly higher on straining than on Valsalva in supine position but not on standing,
and thus abdominal straining is preferred for investigation of pelvic organ prolapse and genuine stress incontinence.
MODIFICATIONS
- Modified Valsalva- Expiration against the resistance of pursed lips or a pursed nose.
The patient should be able to hold his or her breath for at least 10 seconds.Uses-
- Distention of the oral cavity and oral vestibule
- Distention of the Rosenmüller fossa
- Distention of the hypopharynx (including the pyriform sinus and postcricoid area) (fig-17)
- Better delineation of the inner cheek wall
- Evaluation of pneumoparotitis
- DIVE maneuver- Deep inspiration preceeding Valsalva maneuver and rapid expiration immediately following it in colour doppler flow imaging.
[11]Advantages-
- Enhancement of venous blood flow and color Doppler venous filling
- The differentiation between partially and completely occluding thrombi.
- Artificial incomplete filling of the venous lumen with colour signal,
especially in areas such as Hunter’s canal where the vein is extrinsically compressed,unlikely to occur with DIVE.
- Use of compression is reduced.
Performed when compression cannot be applied.
PIT-FALLS AND COMPLICATIONS
- Transient contrast bolus interruption- Suspended deep inspiration with a Valsalva maneuver causes unopacified blood from inferior vena cava to pass preferentially into right heart and pulmonary arteries leading to non-diagnostic CT scan,
or if localised,
may simulate pulmonary embolism.
- Poor contrast in lumen of coronary arteries in CT coronary angiography causing low contrast to noise ratio.
- Estimation of cardio-pericardial silhoutte size on Chest X-ray- If an inadvertant Valsalva maneuver follows deep inspiration,
heart size appears reduced.
- Dampening of hepatic venous waveform- Physiologic factors like high intra-abdominal pressure due to Valsalva maneuver or suspending respiration in end expiration may cause dampening of waveform,
indicative of relative venous outflow obstruction.
- Syncope,
rupture of intra-cranial aneurysms,
rebleeding following hemostasis,
expansion of chronic subdural hematomas,
pneumocephalus,
pneumothorax,
rupture of thin walled meningoceles and spontaneous CSF rhinorrhoea,
Valsalva retinopathy.