Keywords:
Abdomen, Genital / Reproductive system male, Pelvis, MR, MR-Diffusion/Perfusion, Observer performance, Biopsy, Decision analysis, Cancer, Multidisciplinary cancer care, Pathology
Authors:
A. Labra Weitzler, F. Tapia, C. Silva, J. P. Olivares, A. Zuñiga; Santiago/CL
DOI:
10.26044/ecr2019/C-2160
Results
The group of institutional patients (267 patients,
134 biopsied and 133 non-biopsied) was characterized according to age,
prostate-specific antigen,
and prostatic volume.
Mean age of the biopsied group was 60 years and that of the non-biopsied group was 62 years.
(p = 0.03).
There were no significant differences between the patients biopsied and non-biopsied in regards to prostate-specific antigen,
prostate volume and PSA-density. Fig. 5

Fig. 5: Results
PSA-density distribution of the biopsied patients showed skewed shape with a greater number of patients with prostate-specific antigen density close to 0.10 ng/ml/cc. Fig. 6
The results of the transrectal biopsies performed on the group of institutional PI-RADS 3 patients (134 patients) showed 26.8% of clinically significant prostate cancer and 15.6% low-risk cancers.
57.5% of the biopsies showed no evidence of prostatic cancer. Fig. 7

Fig. 7: Number of patients with prostate cancer according to risk group of prostate cancer.
Clinically significant 26,8%
In patients with clinically significant prostate cancer,
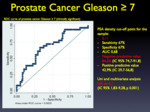
a prostate-specific antigen density cut-off point was obtained to biopsy of 0.11 ng/ml/cc with a sensitivity and specificity of 67% and an AUC of 0.68.
OR for a statistically significant value obtained was 4.1 (IC 95% 1,83-9,28,
p 0,001).
Fig. 8

Fig. 8: ROC Curve of Prostate Cancer Gleason > 7