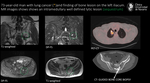
Imaging findings
Before discussing the patterns of bone marrow edema,
it is important to review components of bone marrow (i.e.,
red vs.
yellow marrow).
Bone marrow
Marrow is composed of fat,
water,
and protein (hematopoietic cells).
The proportion of each component varies between red and yellow marrow.
Yellow marrow is composed of a higher proportion of fat (80%),
and red marrow is composed of a higher proportion of protein (20%).
The distribution of red and yellow marrow is a dynamic process that changes with age and physiologic and pathologic triggers. Fig. 4
Distinguishing metastatic disease from red marrow Fig. 5 can sometimes be challenging; however,
there are several clues that can be used in the differentiation.
The cellular proliferation in metastatic lesions locally replaces normal bone marrow,
leading to the disappearance of fatty MR imaging signal inside the lesion; this has been established as a key diagnostic criterion to differentiate neoplastic tissue from normal marrow .
Chemical shift MR imaging is a problem-solving examination for distinguishing red marrow from metastasis or other pathologic infiltrative processes.
In this exhibit,
the causes of bening marrow edema in cancer patients will be reviewed,
include acute or repetitive trauma (fracture,
ligamentous,
or tendon injury); infection; avascular necrosis; metabolic derangement; systemic disease processes (Paget’s,
sarcoidosis); or arthritides
1.TRAUMATIC INJURY
Acute traumatic injuries includes contusions and fracture Fig. 6 .
A direct blow to the bone results in MR findings of bone marrow edema related to trabecular microfracture.
The ill-defined low T1 and corresponding high T2 signal on MRI is similar to stress reactions,
but can be differentiated by patient history,
physical examination findings (overlying ecchymosis),
surrounding soft tissue edema on MRI,
and location of the marrow abnormality.
- NON-ACUTE TRAUMATIC INJURY
BME pattern not related to acute trauma including: stress,
osteochondral lesions,
osteonecrosis,
tendon injury or ligamentous injury
· Stress injuries
Bone or cartilage,
or both,
are frequently injured related to repetitive overuse.
Stress injuries commonly occur with predictable locations and edema patterns.
Common locations include the sacral ala within 1 to 2 cm of the sacroiliac joint,
femoral neck (compressive side),
femoral head epiphysis (subchondral in location paralleling the chondral surface),
tibial plateau,
talar dome,
distal fibula,
posterior calcaneus,
and metatarsal bones.
Endosteal and periosteal bone marrow edema are associated with stress fractures.
The pubic rami stress injury shows the edema most often in small,
confluent and subcortical areas.
Fig. 7
· Osteonecrosis
The end stage of chronic stress may result in osteonecrosis of bone .The classic appearance is a serpentine rim that is low signal intensity on Tl-weighted MR images and has a mixed high and low signal on non-fat- saturated T2-weighted MR images (the double line sign).
The central portion often contains signal that is the same as fat.
A fracture or "crescent sign" in the subcbondral marrow may result from osteonecrosis at the end of a bone.
· Osteochondral lesions
Usually they involve the sub-articular bone and overlying cartilage. The lesion is characterized by a crescentic low signal intensity subchondral fracture line on MRI.
There is often a surrounding reactive BME-like pattern.
It is important to assess the stability of these lesions with imaging.
Fig. 8
.
Tendinopathy
Tendinopathy is a degenerative due to a chronic overuse of a given tendon
In general,
tendinopathy on MRI exibits focal or diffuse tendon thickening with increased or intermediate T2 signal.Small,
recurrent intrasubstance collagen fibril tears may contribute to chronic tendinopathy,
occasionally seen on imaging as focal linear high T2 intrasubstance signal without superimposed acute injury.
Fig. 10
2.INFECTION
Osteomyelitis (OM) is inflammation of the bone marrow secondary to infection,
which can progress to osteonecrosis,
bone destruction and septic arthritis.
Areas of active inflammation show loss of the high marrow signal on the T1-weighted images with increased corresponding signal intensity on the T2-weighted and short T1-weighted inversion recovery (STIR) images.Enhancement is noted on the postgadolinium T1- weighted images.
Cortical bone initially appears normal.
The muscular and fascial planes adjacent to the infected bone may demonstrate localized or diffuse increased signal intensity on the T2-weighted and STIR images Fig. 11 Fig. 12
Areas of inhomogeneous signal intensity are seen in the medullary cavity with areas of acute inflammation characterized by low T1 signal and high T2 signal.
Intervening areas of chronic fibrosis are seen as low signal on T1 and T2 images.
Other findings include cortical bone thickening,
sequestra,
and sinus tracts to the adjacent soft tissues Fig. 16
3.
SYSTEMIC DISEASE PROCESSES
Paget disease is characterized by excessive and abnormal remodeling of bone,
with both active and quiescent phases .
Three pathologic phases have been described: the lytic phase (incipient-active),
in which osteoclasts predominate; the mixed phase (active),
in which osteoblasts cause repair superimposed on the resorption; and the blastic phase (late-inactive) in which osteoblasts predominate.
Bone enlargement as well as trabecular and cortical thickening (which has low signal intensity with all MR pulse sequences) may be seen on MR images; however,
this pathognomonic appearance is easier to appreciate on radiographs.
The MR imaging appearance of the remainder of the marrow in Paget disease is variable and depends on the disease phase and,
more important,
on the histologic composition of the marrow space.
Fig. 13 Fig. 14
4.
ARTHROPATHY
Many of the arthropathies are associated with a reactive BME-like pattern at the margins of the joint.
Active infammatory arthropathies such as rheumatoid arthritis and the seronegative arthropathies produce infiammation within the bone marrow that result in this pattern.
Also present with bone marrow edema,
other features could be present such as erosions,
osteopenia,
periostitis,
synovitis,
ankylosis,
or subluxation.
Fig. 15