In our clinic,
4 cases of jugular vein thrombosis were encountered from a total of 134 cases with cervical ultrasonography performed in the emergency room of “Sf.
Spiridon" Hospital,
from 1 May 2017 to 31 May 2018.
All patients were examined by an experienced radiologist,
initially by ultrasound using a Logiq P9 ultrasound scanner with linear array transducers 11L-D (4.2-12MHz) and 9L-D (3.1-10 MHz),
and then by computed tomography.
Ultrasound
Examination technique: The patient is examined in a supine position with the upper body slightly elevated and the head rotated to the contralateral side.
The examination starts at the supraclavicular level using a medium to high-frequency linear transducer with a satisfying width.
From its confluence with the subclavian vein,
the internal jugular vein is traced upward in transverse section,
while intermittent compression is applied.
The first examination performed is the real-time observation with gray-scale imaging,
followed by color Doppler sonography and Doppler waveform analysis.
The B-mode examination is particularly useful when examining the internal jugular veins because these are very accessible to direct visualization and compression.
It allows to observe the movement of the valves and combined with the two other methods,
the change of diameter as a response to Valsalva maneuver and sniffing,
or during quiet respiration.
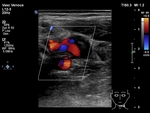
Color Doppler imaging helps to identify the vessels and the thrombosis within when a hypoechoic clot is involved.
The diagnosis is further confirmed with the aid of spectral analysis that measures the degree of venous stenosis,
serial follow-up studies being necessary after anticoagulant or thrombolytic therapy.
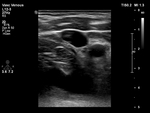
B-mode images: Normally,
the vein should be clear and completely compressible.
Lack of compression or a partially compressed vein is a sign of thrombosis (Fig.
3).
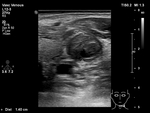
Within the lumen,
a variably echogenic clot may be seen. Recent thromboses are usually more echogenic due to the red blood cells aggregation in early stages (Fig.
1) and tend to become hypo- or anechoic later. The echogenicity of a thrombus is not,
however,
a precise indicator of its age.
A more reliable method is to determine the transverse diameter in comparison with the accompanying artery,
which is more than twice in recent (<10 days) thrombosis.
As the clot retracts (>10 days), the lumen becomes more narrow.
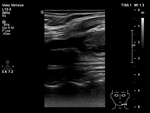
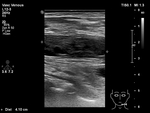
The extent of the thrombosis is determined by identifying the upper limit of the thrombus,
which is usually non-adherent to the wall and with slightly increased echogenicity.
This is particularly important for the follow-up examinations when the treatment response is evaluated.
(Fig.
4)
Another sign of thrombosis is the ”cut-off sign” (in which the normally high-contrast interface between the lumen and the posterior venous wall disappears),
the absence of beating valves and the loss of respiratory variability and vessel pulsation.
Color flow images and Spectral Doppler: The absence of flows is a sign of total venous occlusion.
A color flow between the vein wall and the clot is detectable in case a free-floating thrombus or in case of recanalized thrombosis (Fig.
6). Partial occlusion of a long segment is usually characterized by a Doppler waveform that does not vary with respiration and without atrial pulsation.
An increased flow velocity accompanied by turbulence at the stenosis indicates a partial focal obstruction.
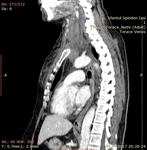
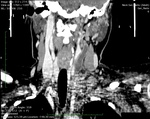
Computed Tomography
Examination technique: The CT scans were captured with a multi-detector-row CT scanner (Somatom Emotion Eco; Siemens Healthineers Headquarters,
Germany),
with the patient in supine position and the images were reconstructed at 2.0-mm intervals.
The adequate bolus of contrast iodine media used to achieve optimal visualization of head and neck venous thrombosis is usually the value of patient's weight + 10 ml, with a 1.0-1.5 ml/s injection rate and the empiric imaging delay is up to 70-80 seconds.
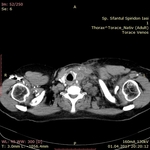
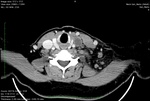
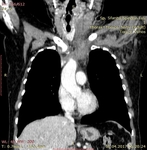
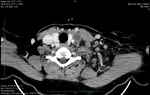
Procedure findings: The direct signs of acute thrombosis are a low-attenuation filling defect that forms an acute angle with the vessel wall or a total cut-off of vascular enhancement within the lumen (Fig.8 ). Indirect signs are represented by the following: the rim of high-attenuation surrounding the filling defect due to the presence of contrast material in the vasa vasorum,
infiltration of the perivenous soft-tissue,
collateral veins and upstream venous dilatation in comparison with the contralateral side.
The most common pitfall is the pseudo-clot,
which is a false positive interpretation resulting from the mixture of opacified and unopacified blood,
especially at the junction of two vessels (for example,
the site of facial vein drainage into the internal jugular vein) (Fig 7,
9,
10,
11).
In contrast to ultrasonography,
computer tomography brings a more reliable contribution distinguishing bland from neoplastic thrombosis,
which is of fundamental importance because of the different management and prognosis.
Direct tumoral invasion into the examined vein,
similar attenuation of both tumor mass and thrombus,
irregular venous lumen expansion and post-contrast thrombus enhancement demonstrating abnormal arterial vascularity are the identifying characteristics.
Ultrasonography can also identify gross direct invasion,
same tumor and clot echogenicity and low-resistance arterial signals within the thrombus in case of neoplasia,
but a subsequent CT is still necessary for a complete description (Fig.
5).
Furthermore,
CT examination helps to establish the etiology with higher accuracy as it gives a richer overview of the entire examined area.
For example,
in Fig 12,
besides internal jugular vein thrombosis, multiple left cervical lymphadenopathies are also shown,
which were proven to be the source of non-Hodgkin lymphoma.
Another case of the four ones was associated with malignancy,
the root pathology being breast cancer,
another with a mediastinal infection and only one patient had prolonged central vein catheterization.