Type:
Educational Exhibit
Keywords:
Embolism / Thrombosis, Blood, Recanalisation, Diagnostic procedure, Ultrasound-Spectral Doppler, Ultrasound-Colour Doppler, Ultrasound, Veins / Vena cava, Vascular
Authors:
M. Chiscaru, C.-E. Hincu, A.-M. Alecsa-Lupu, M. Ursaru, L. Gheorghe; Iasi/RO
DOI:
10.26044/ecr2019/C-2244
Background
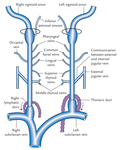
The internal jugular vein is a paired,
symmetrical venous structure which plays the role of the main blood collector from the brain,
superficial parts of the face and neck.
It continues the sigmoid sinus from its skull exit through the jugular foramen and joins the subclavian vein at the junction of the neck and thorax to form the brachiocephalic vein.
It has a caudal path in the carotid sheath where is accompanied anteromedially initially by the internal and then the common carotid artery and posteriorly by the vagus nerve.
Due to its superficial course in the neck,
it is very accessible to ultrasound examination,
which is the first diagnostic procedure used to exclude jugular vein thrombosis (Fig.
2).
Thrombosis of the internal jugular vein is a rare,
probably underdiagnosed condition whose serious complications such as pulmonary embolism can be fatal.
Therefore the importance of prompt and correct diagnosis and treatment is primary.
Apart from the pulmonary embolism,
other possible sequelae are the extension of the thrombus into the nearby veins,
recurrent thrombosis,
and chronic residual vascular obstruction.
It is mostly related to prolonged central vein catheterization as the internal jugular vein is a preferred access site for a central venous catheter.
Recently it is was observed an increased incidence of jugular vein thrombosis at intravenous drug users who are injecting the substances directly in their internal jugular veins.
Other possible causes include head and neck infections,
extension or compression from nearby inflammatory or neoplastic processes,
the hyper-coagulability status induced by neoplasia and also surgical procedures performed in the nearby area.
A particularly condition is Lemierre's syndrome which is characterized by thrombophlebitis of the internal jugular vein with distant metastatic sepsis following an initial oropharyngeal infection such as pharyngitis or tonsillitis.
As clinical manifestation,
patients may present with a painful swelling of the affected side of the neck that can also extend to the ipsilateral upper extremity,
or may be asymptomatic.
Occasionally collateral veins in the lower neck or over the anterior chest wall can be observed,
phenomena known as the Urschel sign.
This appears mostly in chronic thrombosis due to the prolonged dysfunctional drainage from the internal jugular vein.