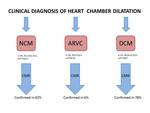
Left ventricular non-compaction cardiomyopathy (NCM) is a rare structural abnormality of the left ventricular (LV) myocardium of uncertain etiology and with unknown molecular patho-mechanism.
LVNC is characterized by numerous prominent trabeculations and deep intertrabecular recesses in hypertrophied and hypokinetic segments of the left ventricle. The clinical presentation of the disease is highly variable,
ranging from asymptomatic one to severe heart failure and even sudden cardiac death [1].
In our study the patients with supposed diagnosis of NCM had a clinical signs of arterial hypertension in 10% of cases,
arrhythmias and conduction disorders - in 23%, chronic heart failure - in 20%.
Left ventricle ejection fraction was slightly reduced to 45.3±17.8%.
After CMR the presence of non-compact myocardium was confirmed in 42%,
DCM with hypertrabeculation was confirmed in 9% of cases.
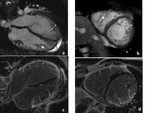
Intramyocardial fibrosis was observed in 7% of individuals. Fig. 2 illustrates CMR results of the patien,
25-year-old man,
with in-frame deletion in the gene DES.
Arrythmogenic right ventricular cardiomyopathy (ARVC) is an inherited cardiomyopathy that leads to ventricular arrhythmias and often causes SCD in the young.
CMR is an important adjunct in making the diagnosis of ARVC,
primarily due to its accuracy in assessing right ventricular dilatation and dysfunction.
Diagnostic findings in this disease include RV dilatation and global or regional dysfunction including focal RV systolic bulging or aneurysm [4].
LV involvement in ARVC is increasingly recognized [9].
Quantitative functional RV imaging with strain measures by CMR feature tracking may objectify regional functional measures and improve upon diagnostic accuracy for ARVC compared to qualitative analysis of cine images [8].
The hallmark of the diagnosis,
however,
remains RV dilatation and dysfunction.
In ARVC group the clinical diagnosis was represented by arrhythmias and conduction disorders in 42% (without specifying the etiology).
Myocarditis and congenital heart defects were suspected in 6% of patients.
In this group of patients LVEF was not impaired (59.2±9%).
The average number of ventricular extrasystoles day by Holter monitoring data was 11942±13003,
number of supraventricular extrasystoles was 1340±351.
The diagnosis of ARVC was confirmed in 6% of patients,
the diagnosis of other CMP was specified in 9% (hypertrophic,
dilated or non-compaction),
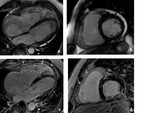
signs of myocarditis was found in 3%. ARVC and myocarditis were excluded in 56%. Fig. 3 illustrates LGE CMR results of 48-year old patient with bi-ventricular ARVC,
with familial history of cardiomyopathy.
After the confirmation of ARVC diagnosis the cardioverter defibrillator has been implanted to the patient with paroxismal venricular tachiarrhythmia and the history of syncopes.
Dilated cardiomyopathy likely represents an end-stage manifestation of multiple non-ischemic disorders that can damage the myocardium.
The management plan is often determined by patient symptoms,
abnormalities on the electrocardiogram,
and LVEF; however,
this is an imperfect approach that does not adequately identify those patients who are unlikely to respond to medical therapy or at risk for sudden cardiac death.
Recently,
there has been growing interest in exploiting the role of myocardial fibrosis,
an integral pathophysiologic component of dilated cardiomyopathy,
as a biomarker for guiding the patient management and determining the prognosis.
It is increasingly being understood that fibrosis can occur in two forms that can be detected by CMR [2]: irreversible replacement fibrosis which corresponds to the presence of LGE and diffuse interstitial fibrosis which better corresponds to findings on T1-mapping.
In the investigated cohort DCM was clinically suspected in 53% of the patients; in 27% of the patients it should be differentiated from myocarditis or other CMP.
In 62% of patients,
arrhythmias and conduction disorders were observed.
In the group of patients with syndrome of DCM,
LVEF was significantly reduced (29.9±12.7%).
In DCM group the diagnosis was confirmed in 78%,
an aetiology was specified in 36% (21% of the patients had signs of myocarditis,
myocardial scar was visualised in 15%).
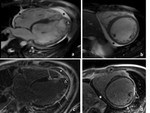
Fig. 4 illustrates LGE CMR results in 19 year-old patient with heart failure (LVEF - 17%) that proved postinflammatory aetiology of DCM.
In 20% of patients with doubtful diagnosis of NCM and ARVC the results of genetic testing confirmed CMR.