The thickening of the vesicular wall can occur in both primary and secondary diseases.
The first group includes cholecystitis (acute,
chronic,
acalculous and xanthogranulomatous),
carcinoma of the gallbladder and adenomyomatosis,
while in the second pathologies such as liver cirrhosis,
hepatitis,
right heart failure,
renal failure and pancreatitis among others.
Physiological thickening of the vesicular wall should not be confused with a pathological finding in patients who gallbladder is not distended.
For this reason,
in order to correctly assess the parietal thickening of the gallbladder it is important that the patient is fasted to distend de gallbladder.
There are numerous pathologies that can cause parietal thickening (Table 1),
so it is necessary to make a differential diagnosis between them.
Primary diseases
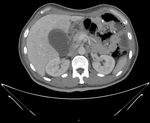
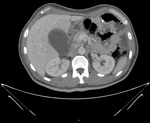
Acute cholecystitis (Figures 1 and 2)
It is the first diagnosis to take into account if parietal thickening of the gallbladder wall is seen because of its high incidence.
Although parietal thickening is suggestive of cholecystitis,
it is important to detect other signs to support the diagnosis since it is not pathognomonic of cholecystitis.
Among the signs suggestive of acute cholecystitis are:
- Obstructive biliary lithiasis.
- Gallbladder hydrops (marked distension).
- Sign of positive "Murphy ultrasound" (pain at pressure on the location of the gallbladder).
- Inflammation of the fat or presence of perivesicular fluid.
- Hyperemia of the vesicular wall seen in Doppler mode.
Acalculous cholecystitis
Acute acalculous cholecystitis occurs mainly in very sick patients due to an increase in the viscosity of the bile as a consequence of fasting and medication,
which leads to a state of cholestasis.
Ultrasonography findings are similar to those of acute gallstone cholecystitis but,
as the name suggests,
stones are not seen in acalculous cholecystitis,
although gallbladder sludge is frequently present.
Chronic cholecystitis (Figure 3)
It is called chronic cholecystitis to mild inflammation of the gallbladder with fibrosis due to transient obstruction by a stone.
The imaging findings,
which are slight parietal thickening and cholelithiasis,
must be accompanied by a compatible clinical history.
Xanthogranulomatous cholecystitis
Xanthogranulomatous cholecystitis is a rare variant of chronic cholecystitis characterized by an inflammatory process with lipid deposition that is comparable to xanthogranulomatous pyelonephritis.
Imaging findings are a marked thickening of the gallbladder wall,
which sometimes contains hypoechoic intramural nodules in ultrasound that are hypodense in CT.
These nodules represent abscesses or foci of xanthogranulomatous inflammation.
Occasionally,
the imaging findings of this pathology are indistinguishable from gallbladder carcinoma.
Porcelain gallbladder
A porcelain gallbladder is a rare entity caused by a mural calcification due to chronic cholecystitis.
In these patients,
prophylactic cholecystectomy is important because of its association with gallbladder carcinoma,
although this complication seems to be infrequent.
Gallbladder carcinoma
Vesicular carcinoma is the fifth most frequent cause of cancer of the gastrointestinal tract.
Sometimes it is detected in advanced stages of the disease as a consequence of the lack of early and specific symptoms.
In imaging tests,
it can be seen from intraluminal polypoid lesions to an infiltrating mass that completely replaces the gallbladder.
In addition,
it can also present as a diffuse parietal thickening.
Other findings,
such as the invasion of adjacent structures,
secondary dilatation of the biliary ducts and hepatic metastases or metastatic adenopathies,
can help in the differential diagnosis with other pathologies such as acute or xanthogranulomatous cholecystitis.
In the absence of these findings,
it is possible that carcinoma can not be distinguished.
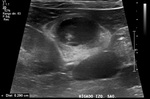
Adenomyomatosis (Figure 4)
Adenomyomatosis of the gallbladder is characterized by epithelial proliferation,
muscle hypertrophy and intramural diverticula,
which can affect the wall of the gallbladder in a segmental or diffuse manner.
It is a benign pathology that does not require specific treatment,
being a relatively frequent incidental finding.
In ultrasound,
cholesterol crystals present reverberating artifacts that make the diagnosis compatible when parietal thickening is present.
Air causes similar artifacts,
so differential diagnosis with emphysematous cholecystitis must be included (Figure 5); however,
patients with emphysematous cholecystitis are quite ill and patients with adenomyomatosis are asymptomatic.
Secondary diseases
Systemic diseases such as liver cirrhosis (Figure 6),
hepatitis (Figures 7 and 8),
heart failure,
pancreatitis or renal failure may cause parietal thickening of the gallbladder.
The pathophysiological mechanism by which this occurs is unknown,
but it is likely due to various factors such as portal hypertension,
increased central venous pressure or decreased intravascular osmotic pressure.
Other factors,
such as hypoproteinemia,
have also been proposed although with little scientific evidence.
In liver cirrhosis,
thickening of the vesicular wall is thought to be due to portal hypertension and to the decrease in intravascular osmotic pressure.
In pancreatitis,
parietal thickening of the gallbladder may be secondary to the direct extension of the inflammation or due to an immunological reaction.
Other entities such as hepatitis and pyelonephritis can also cause an increase in the thickness of the gallbladder wall by the same mechanism.
Other causes of parietal thickening,
such as infectious mononucleosis or HIV,
have also been described,
the latter due to the appearance of opportunistic infections or secondary neoplastic infiltration.