Keywords:
Vascular, Interventional vascular, CT-Angiography, Catheter arteriography, Diagnostic procedure, Embolisation, Aneurysms
Authors:
R. Antoniak1, L. Grabowska-Derlatka2, R. B. Maciag1, O. Rowinski1; 1Warsaw/PL, 2Warsaw, NO/PL
DOI:
10.26044/ecr2019/C-2355
Results
In our series:
1.
All but one CA lesions were secondary to MAL compression.
Furthermore,
we presume that atherosclerotic plaques in CA ostium do not exclude the preexisting compression.
SMA stenosis was identified in one patient with an appearance suggesting it’s compression.
2.
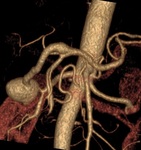
Aneurysms involved all main collateral pathways through anterior and posterior pancreaticoduodenal arteries as well as dorsal pancreatic artery in only one patient.
Multiple PAAAs were nearly as common as solitary.
Great majority of PAAAs involved inferior pancreaticoduodenal arteries.
Their size ranged from 3/3/3 mm to 50/51/53 mm.
Nearly all PAAAs were saccular.
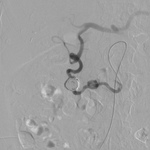
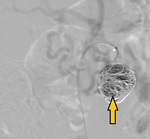
Fourteen patients underwent successful endovascular embolization with no complications (Fig.
9).
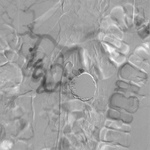
Follow-up studies (angiography and/or MRI) revealed residual leakage of contrast media into the aneurysm in two cases.
They required additional embolization (Fig.
10 and 11).
All other aneurysms remained stable with no filling of contrast media.
We performed angiography and/or MRI to avoid artifacts produced by embolic agents in CT,
which obscure both borders of the aneurysms and possible residual endoleak.
There is no clear consensus regarding treatment of CA lesion in these patients [6].
There are no known cases of aneurysm recurrence after treatment [7].
Celiac revascularization should be considered in symptomatic patients.
We do not recommend stenting in case of CA compression as we have seen stent occlusions and fractures.
Surgery was performed in seven patients,
in more complex cases.
There were three serious complications of treatment.
Two of them,
including infection of aorto-hepatic by-pass in one patient and injury of right hepatic artery and common bile duct in another,
were managed conservatively.
Arterial bleeding,
fluid collections,
and biliary fistula complicated pancreaticoduodenectomy performed due to coexisting pancreatic cancer in the third patient.
They were successfully managed in subsequent surgical procedures.
In the follow-up,
we preferred angio-CT for patients treated only surgically and angiography/MR for those,
who underwent subsequent embolization.
These studies showed stenosis and aneurismal dilatation of reno-hepatic by-pass in one patient (Fig.
12) and minimal dilatation in another one.
Other grafts and treated aneurysms remained stable.