Aims and objectives
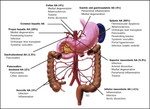
Aneurysms of peripancreatic arterial arcades (PAAAs) account for about 2-5% of all splanchnic aneurysms [1] (Fig.
1),
which in turn affect 0,1-2% of general population.
True aneurysms occur less often than false aneurysms.
There is usually no history of pancreatitis,
pancreatic trauma or surgery.
Great majority of these aneurysms coexist with celiac axis stenosis/occlusion.
They are asymptomatic or present with vague abdominal pain unless ruptured.
Their rupture is unpredictable [2] and,
according to the literature,
fatal in up to 20% [3].
The aims of our...
Methods and materials
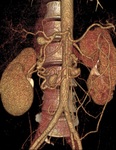
We present a series of 21 patients with PAAAs (Fig.
2).
The diagnosis was established by contrast-enhanced CT in all cases.
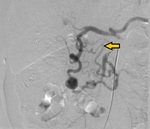
We evaluated different collateral pathways connecting celiac axis (CA) and superior mesenteric artery (SMA) circulations for presence of aneurysms (anterior pancreaticoduodenal arteries,
posterior pancreaticoduodenal arteries,
dorsal pancreatic artery and gastroepiploic arteries,
Fig.
3).
The aneurysms were characterized by their number,
location,
size and morphology.
We paid special attention to patency of CA and SMA and the most likely cause of their stenosis/occlusion.
Absence of...
Results
In our series:
1.
All but one CA lesions were secondary to MAL compression.
Furthermore,
we presume that atherosclerotic plaques in CA ostium do not exclude the preexisting compression.
SMA stenosis was identified in one patient with an appearance suggesting it’s compression.
2.
Aneurysms involved all main collateral pathways through anterior and posterior pancreaticoduodenal arteries as well as dorsal pancreatic artery in only one patient.
Multiple PAAAs were nearly as common as solitary.
Great majority of PAAAs involved inferior pancreaticoduodenal arteries.
Their size ranged from...
Conclusion
In case of CA stenosis/occlusion,
we should focus on peripancreatic circulation and actively search for aneurysms.
On the other hand,
if we find a PAAA,
we should assess patency of splanchnic arteries.
PAAAs are prone to rupture and there are no risk factors for their rupture.
Endovascular techniques play major role in their management.
We recommend surgical or combined treatment in three scenarios:
1.
All collateral pathways connecting CA and SMA affected by aneurysms
2.
Comorbidities requiring surgery,
eg.
pancreatic head cancer
3.
Technical failure...
Personal information
R Antoniak,
MD
2nd Department of Radiology,
Medical University of Warsaw - Warsaw/PL
Banacha 1a str.
02-097 Warsaw,
Poland
Phone: +48225992300
Fax: +48225992302
E-mail:
[email protected]
References
1.
Pasha S.F.,
Gloviczki P.,
Stanson A.,
et al.
Splanchnic artery aneurysms.
Mayo Clin Proc 2007;82(4):472–479.
2.
Kallamadi R.,
DeMoya M.
A.,
Kalva S.
P.
Inferior pancreaticoduodenal artery aneurysms in association with celiac stenosis/occlusion.
Seminars in Interventional Radiology.
2009;26(3):215–223.
3.
Moore E.,
Matthews M.
R.,
Minion D.
J.,
et al.
Surgical management of peripancreatic arterial aneurysms.
Journal of Vascular Surgery.
2004;40(2):247–253.
4.
Flood K.,
Nicholson A.
A.
Inferior pancreaticoduodenal artery aneurysms associated with occlusive lesions of the celiac axis: diagnosis,
treatment options,
outcomes,
and review...