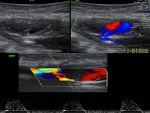
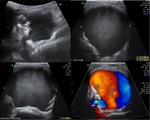
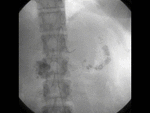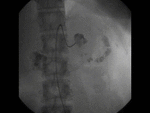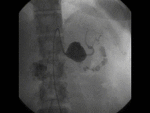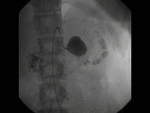
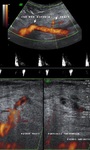
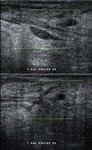
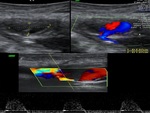
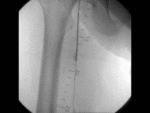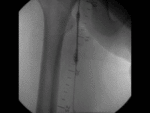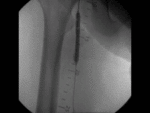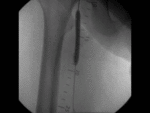
US & Colour Doppler (Figures 1 and 2)
Imaging features:
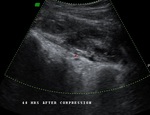
Pseudoaneurysm appears as an irregular hypoechoic cystic structure on Gray-scale US located in relation to a supplying parent artery.
Ultrasound characterizes the pseudoaneurysm in terms of number,
size of the sac,
number of compartments within the sac and the size of the neck,
simple or complex nature and the presence of septae.
Differential diagnosis of pseudoaneurysms on gray scale US would include simple and complex cysts and hematomas.3
On Colour Doppler,
the 'yin-yang' sign is appreciated owing to bidirectional or 'to and fro' flow leading to swirling of blood.
The 'to' component is blood entering the pseudoaneurysmal sac in systole and the 'fro' component is blood leaving the pseudoaneurysmal sac during diastole.3,5
Advantages 3,6:
Disadvantages:
-
Evaluation of visceral arteries is limited
-
Operator dependence
-
Limited evaluation of vessels in trauma with fractures or hematomas
-
Yin yang sign may also be seen in saccular true aneurysms
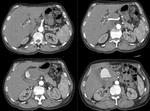
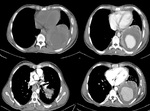
Computed Tomography (Figures 3 and 4)
Imaging features3,7:
Unenhanced CT scans :
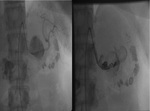
Low-attenuation rounded structure arising from the donor artery
Adjacent high attenuation indicates hemorrhage due to pseudoaneurysmal rupture.
The wall is usually smooth and well delineated.
A thickened,
irregular,
or ill defined wall points toward a mycotic pseudoaneurysm.
Contrast-enhanced CT :
Contrast –filled sac
A low-attenuation area within the pseudoaneurysm indicates partial thrombosis
The donor artery is adjacent to the pseudoaneurysm and can usually be seen communicating with it
Advantages 7,8:
-
Not operator dependent
-
Short acquisition time
-
Three-dimensional (3D) images allow for better spatial information
-
Detects associated injuries or other associated disease entities,
for example trauma or pancreatitis
-
Good accuracy (sensitivity - 95.1% and specificity - 98.7%)
Disadvantages:
-
Limited by imaging artifacts
-
Difficulty distinguishing between pseudoaneurysms and true aneurysms in small visceral arteries
-
Use of contrast material and ionizing radiation
-
No scope for intervention at the time of diagnosis
Conventional angiography (Figure 5)
Imaging features:
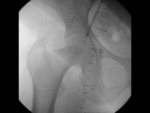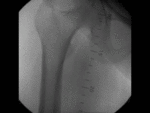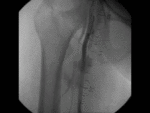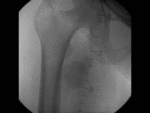
Usually performed after a baseline CT to identify the feeding vessel.
This is done in order to identify the main parent artery.
Selective catheterization of the parent artery and contrast injection causes contrast filling of the pseudoaneurysmal sac.
Advantages 9:
-
Capacity for real-time hemodynamic assessment of the vascular bed
-
Identification of collateral vessels and other pseudoaneurysms in the same vascular bed
-
Accurate identification of the donor artery with selective angiography
-
Concomitant therapeutic potential
Disadvantages 3:
-
Invasive nature and the increased risk of procedure-related complications (including the risk of developing a pseudoaneurysm at the puncture site,
hematomas,
arteriovenous fistulas,
distal embolization,
arterial spasm,
ischemia,
intimal dissection and vessel thrombosis)
-
Ionizing radiation and contrast material usage
-
Does not help accurately assess the size of a partially thrombosed pseudoaneurysm
-
Vascular lesions,
including other pseudoaneurysms,
can be overlooked if particular vascular beds are not evaluated during catheter-directed angiography.
Therapy
When to treat?3,4,10
Depends on factors like the size,
its location,
availability of material,
expertise and cost
Large symptomatic pseudoaneurysms often require intervention
Smaller lesions need conservative monitoring with a careful watch on its progression
Minimally invasive therapeutic options
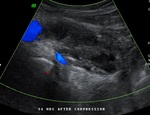
US guided compression (Figures 6 to 11)
How is it done?
Compression is performed with the US transducer.
This permits direct and continuous visualization of the vessels.
An initial 10–20-minute compression of the pseudoaneurysmal neck or the pseudoaneurysm itself is done.
Compression eliminates flow within the pseudoaneurysm and induces thrombosis,
but permits arterial perfusion to the extremity.
This can be repeated in cycles for up to 1 hour.
3,11
Advantages:
Disadvantages:
-
Limited by patient and operator discomfort due to the long compression time required
-
Only fairly superficial pseudoaneurysms can be treated
-
Limited application in obese patients
-
High failure rate with recurrence
-
Venous thrombosis,
skin necrosis,
and pseudoaneurysmal rupture
-
Local arterial thrombosis and distal embolization11,
12
US guided thrombin injection
How is it done?
Thrombin leads to thrombus formation by conversion of inactive fibrinogen into fibrin.
After complete US evaluation,
thrombin is injected into the sac under aseptic precautions and US guidance.
Thrombin is injected in the center of the sac,
while flow within the sac is monitored.
This is done until flow within the sac ceases.
The volume injected ranges from 0.5 to 1.0 mL,
the concentration of the formulation being 1000 IU/mL. 3,13
Advantages:
-
Greater than 90% success rate
-
Deep visceral arteries may also be treated
-
Can be performed when the donor artery is endoluminally inaccessible and its occlusion is not a viable option
-
Arteries above the inguinal ligament can also be treated with this method,
which is contraindicated in US-guided compression
Disadvantages:
Endoluminal management
How is it done?
The arterial anatomy and the caliber of the arteries leading to and at the pseudoaneurysm site should be favorable.
Broadly,
the methods employed in the endoluminal exclusion of a pseudoaneurysm fall into coil embolization (Figure 12) and stent placement (Figures 13 and 14).
Embolization of the afferent artery can be performed for a pseudoaneurysm that arises from an artery which does not have a collateral supply,
also known as an expendable donor artery.
A pseudoaneurysm arising from an inexpendable donor artery must be excluded from the circulation while preserving the donor artery.
Arteries that have a well-established collateral supply include the gastroduodenal,
hepatic,
and splenic arteries and other upper gastrointestinal arteries,
some pelvic and distal extremity arteries,
namely the internal iliac artery and the profunda femoris artery.
When embolizing arteries with numerous collateral vessels,
embolization must be performed both proximal and distal to the pseudoaneurysm.
This is so there is a complete exclusion and no backflow from the collateral circulation.
The width of the pseudoaneurysmal neck and the diameter of the donor artery determine the method used.
If the neck is narrow,
coil embolization with catheter-directed delivery of coils is the method chosen.
However,
there is potential for recanalization of the sac if the coils are not tightly packed.
The use of soft helical coils tightly packed into the sac has a low risk of recanalization.
Thrombin or N-butyl 2-cyanoacrylate (glue) may be used in addition to coils.
If the neck is wide,
remodeling is required to prevent outflow of these materials into and distal embolization.
Stent caging or trapping the coils by temporary balloon occlusion of the donor artery prevents coil outflow.
Another option,would be covered stent-graft placement across the neck.
3,9,
14
Advantages:
Disadvantages: