Keywords:
CNS, Neuroradiology brain, Oncology, MR, Diagnostic procedure, Neoplasia
Authors:
J. F. Landa Pake1, A. Pons Escoda2, P. Naval Baudin3, A. Guell Bara4, I. RODRIGUEZ CAAMAÑO2, I. Oronoz Mitxelena2, C. Aguilera Grijalvo2, C. Majós2; 1L'Hospitalet de Llobregat/ES, 2Barcelona/ES, 3L'Hospitalet de Llobregat, Barcelona/ES, 4Tarragona/ES
DOI:
10.26044/ecr2019/C-2458
Methods and materials
Catalan Institute of Oncology performs its activity in Duran & Reynals Hospital working together with the Bellvitge University Hospital,
as a reference center specialized in cancer treatment.
It has a network of collaboration with 7 county hospitals within the south area of Catalonia,
covering a population of over 1.200.000 patients.
Image acquisition:
The MRs were performed in our center at Philipps 1.5T & 3T MR devices.
All the MRs included at least sagittal T1,
axial T2,
axial FLAIR,
axial DWI,
and coronal and axial T1 post- gadolinium injection.
Data Collection:
We reviewed our neurooncology unit files between 2015 and 2018 for cases of confirmed isolated brain mets and GB.
56 patients with single brain mets and 120 with GB were included.
Multiple and extraaxial lesions as well as suboptimal MR exams were excluded.
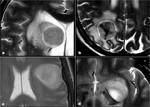
Two staff neuroradiologists and one radiologist in training jointly blindly reviewed the T2-weighted MR sequence of all the cases for the presence or absence of the “T2-parenchymal cleft sign”.
When the sign was doubtful,
it was considered as absent.
Fig. 4
Statistical analyses:
Descriptive statistics were obtained and a chi-square test was performed.