Coronary CT images should be acquired as isotropic submillimeter 3-dimensional electrocardiography (ECG)-gated data sets (1),
in either retrospectively gated helical mode or prospectively triggered sequential mode.
Images must be reviewed interactively on cardiac-specific interpretation software platforms capable of 2- and 3-dimensional displays in all conventional reconstruction formats.
Because of the complexity of coronary anatomy,
the need of lesion morphology details and management of motion and calcium-related image artifacts,
acknowledgment of the application of the variety of image formats may improve diagnostic quality.
Interpretation formats
a)Transaxial images
Consist of a series of 2-dimensional images in the cranial-caudal direction,
in which they were acquired.
These help to obtain general information of the presence of atherosclerotic lesions (location,
composition) and to depict coronary and mediastinal anatomy.
(2)
The advantage of this format is that it displays the minimum likelihood of distortion consequent to postprocessing and the maximum resolution and gray-scale rendering .
A disadvantage of this format is that it requires the reader to mentally reconstruct the 3-dimensional anatomic relationships of the structures.
The thickness of each slice is determined by the reconstruction width and is not variable,
so tortuous arteries will move in and out of plane.(3)
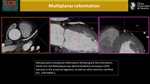
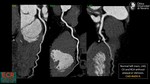
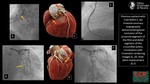
b)Multiplanar reformation (MPR)
MPR is a reconstruction format from isotropic high-resolution CT acquisitions,
where image data can be rearranged in arbitrary imaging planes (orthogonal and oblique) with excellent image quality.
(Fig.2)
It has the advantage of allowing views of coronary artery lesions from different angles and perspectives,
which enables better assessment of stenosis severity.
This is of particular importance in the presence of severe calcifications,
where a single view often fails to display residual lumen in the proximity of a heavily calcified plaque (2).
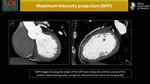
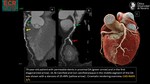
c)Maximum Intensity projection (MIP)
MIP incorporates a volume that includes the entire vessel lumen and wall diameter,
creating thicker sections (commonly 5 mm).
The intensity of each voxel is set at the maximum HU value along its line of intersection in the slab volume between the tube and detectors (3).
These features allow the reader to visualize a longer segment of a vessel’s course and tend to reduce perceived image noise.
MIP is similar to MPR in that orthogonal or oblique planes can be reviewed interactively (Fig.
3).
However,
there is loss of lesion information within the slab volume,
as the MIP does not provide in-depth information or attenuation detail within the slice.
Consequently,
MIP should never be the sole technique used to assess stenosis severity or plaque composition.
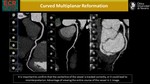
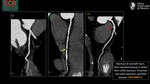
d)Curved Multiplanar Reformation (cMPR)
The cMPR image is created by tracing the centerline of the artery (manually or automatically) and producing an MPR along the curving path.(Fig.4)
It has the advantage of viewing the entire course of the vessel in one single image,
but this requires that the centerline of the vessel is tracked correctly.
It has the potential to produce artifactual lesions unless carefully (4),
should not be used in isolation.
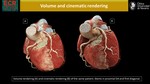
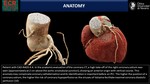
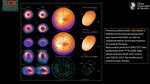
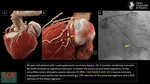
e) Volume-rendering technique
Creates volumetric 3-dimensional representations with the illusion of spatial integrity and color.
It is generally not useful for the assessment of coronary stenosis because the apparent thickness of the vessel lumen is dependent on window settings and the computer algorithm that is used to subtract nonvascular structures.(4)
VRTs are useful for visualizing spatial relationships,
such as thoracic-cardiovascular anatomy,
defining the course of coronary anomalies and the presence and course of coronary bypass grafts.
This technique finds much more for teaching purposes and illustrations for patients.
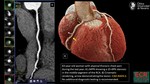
f)Cinematic rendering
Cinematic VRT is a research visualization technology that enables 3D photo-realistic images to be produced.
It creates a realistic appearance attributed to the image-based technique of shading.
(Fig.
5)
The algorithm uses a Monte Carlo path tracing method to generate photorealistic images by light transport simulation along the photons paths per pixel through the anatomy.
Such natural lighting in combination with the accurate simulation of photon scattering and absorption,
leads to photorealistic images that resemble many shading effects that can be observed in nature (5)
A complete evaluation of a coronary CT report should include (Fig.6):
1) Examining image quality
Familiarity with potential pitfalls and artefacts is important,
as they may lead to misinterpretation.
They can be classified in three categories:
1.1.
Motion-related artifacts
They can be due to breathing,
variations in heart rate during breathholding,
or irregularity of heart rate.
As a consequence,
blurring of the vessel or stepladder effects may occur.
The longitudinal direction of the vessel may abruptly shift and simulate a vessel stenosis.
Reconstructions at a different cardiac phase may be helpfull.
The easiest way of reducing cardiac motion artefacts is to lower the heart rate before the acquisition of the study using beta blockers (9). Artifacts due to breathing or body motion are distinctive because they affect the bones of the anterior or lateral chest wall in addition to the coronary arteries; these are less likely to be correctable by additional reconstructions.
1.2.
Beam hardening and structural artifacts
Produced by surgically implanted high-attenuating materials,
natural structures (such as coronary calcifications) or by contrast enhancement.
Calcified plaque and stents appear to narrow the lumen more than they actually do.
The adjustment of the Reconstruction Algorithm (‘‘Kernel’’) may help to reducE this artefact.
For the evaluation of coronary artery stents or inte presence of heavy calcifications,
it is recommendable to use a higher kernel with even stronger edge enhancing characteristics and greater spatial resolution.
(2)
1.3.
Reduced signal-to-noise and low vessel contrast intensity
Image quality may be impaired by poor signal to noise,
which can be because of obesity,
improper scan parameters (low tube output for a given body size),
or reconstruction during a part of the cardiac cycle with reduced tube current from electrocardiography-guided tube modulation.
Low contrast intensity may be secondary to improper image acquisition timing or slow contrast injection (3).
2) Coronary calcium scoring
The determination of the calcium score by CT is based on non-contrast axial slices,
with a thickness of 3 mm,
without overlapping or gaps,
limited to the cardiac region,
acquired prospectively in synchrony with the electrocardiogram at a predetermined moment in the R-R interval,
usually in the mid/late diastole.
(6)
Calcification is identified as areas of hyperattenuation of at least 1 mm2-with > 130 Hounsfied units (HU) or ≥ 3 adjacent pixels.
The main system for the quantification of the calcium score is the Agatston method,
which is used as a reference for most population databases and publications involving risk stratification and is therefore the method most often used in clinical practice.(7)
The values obtained can be interpreted and classified in two ways by using population databases,
being the Multi-Ethnic Study of Atherosclerosis (MESA) the most widely used.
(8) The total calcium score should be reported as well as the percentile as compared with age and gender nomograms.
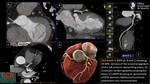
3) Analyzing coronary artery anatomy
The coronary tree should be initially examined for the course and branching of the main coronary vessels and subbranches.
Coronary anomalies should be examined with regard to their origin,
course,
and relationship to important structures such as the cardiac chambers,
aorta,
pulmonary artery,
and interventricular septum.(Fig.7) (10)
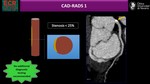
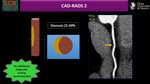
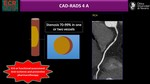
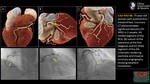
4)Assessment of coronary stenosis severity: CAD-RADS
Standardized CAD-RADS categories are based on the highest grade of coronary stenosis detected in any vessel. For the grading of stenosis severity,
a classification system suggested by the Society of Cardiovascular Computed Tomography is used (see Fig.8).
(12) It should reflect the clinically most relevant finding per patient along with a follow-up management recommendation.
Figures 9 through 26 provide examples of CAD-RADS categories and sub-categories.
Among patients with CAD-RADS 0 to 2,
no additional diagnostic testing is recommended.
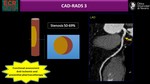
In patients with CAD-RADS 3,
implementation and maximization of medical therapy are recommended along with additional functional assessment.
In contrast,
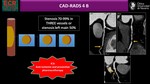
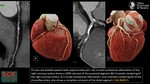
further invasive testing is recommended for CAD-RADS 4A to 5 along with preventive therapies and risk factor modification.
(11)
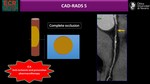
The clinical relevance of CAD-RADS 5 (total coronary occlusion) varies widely depending on the clinical context.
It may be acute or chronic,
and,
in the context of chronic occlusion,
factors such as lesion length,
calcification particularly at the proximal cap,
and degree of collateralization may be of relevance for management decisions.
CAD-RADS categories can be complemented by modifiers.
The symbol “/” (slash) should follow each modifier in the following order (11):
Modifier N – Non-diagnostic study
If not all segments > 1.5 mm diameter can be interpreted with confidence. The highest stenosis of the valuable segments should be graded in addition to the modifier N.
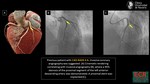
Modifier S
Indicates the presence of at least one coronary stent anywhere in the coronary system.
It does not matter whether the stenosis is in-stent or a non-stented vessel.(fig.
25)
Modifier G -Presence of coronary bypass grafts
Indicates the presence of at least one coronary-artery bypass graft.
Stenosis bypassed by a fully patent graft is not considered for the CAD-RADS classification.(Fig 26)
Modifier V- Presence of “vulnerable” or high-risk plaque features
They include positive remodeling,
low-attenuation plaque,
spotty calcification,
and the napkin-ring sign.
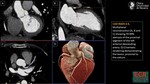
5)Non-coronary cardiac and extracardiac incidental findings.
By nature of the imaging technique and coverage,
thoracic,
noncardiovascular structures (pericardium,
cardiac chambers,
pulmonary arteries and veins,
thoracic aorta) and upper abdominal anatomy,
should be reported.
Review of all visible structures is important recognition of primary and secondary comorbid pathology,
and for the identification of findings that lead to alternative noncardiovascular diagnoses (3).
6) Clinical and therapeutic relevance of the imaging findings
Structured reporting is increasingly recommended to assure quality and consistency.
Uniform reporting and terminology minimizes an important source of interreport variability.
In addition,
data review may be facilitated ensuring that all required findings needed for patient care are contained within the report.
CAD-RADS not only has the capability of providing accurate prognostic information that can be easily conveyed to physicians using standardized and clinically intuitive coronary CTA definitions,
but it could also,
serve as a clinical decision support tool by including actionable,
guideline-directed recommendations for each score within the coronary CTA report.
Some recent studies have examined long-term prognosis associated with the novel CAD-RADS scores.
High rates of early invasive testing were identified in stable patients with intermediate coronary stenosis (CAD-RADS 3),
many of whom were either asymptomatic or not receiving guideline-directed medical therapy at baseline.(11)
Integration of CAD-RADS guided recommendations into clinical practice may provide a novel opportunity to reduce over-referral for downstream invasive coronary angiography and promote more appropriate follow-up care among patients undergoing a diagnostic evaluation for CAD.