Keywords:
Arteries / Aorta, Vascular, CT-Angiography, MR, Image manipulation / Reconstruction, Segmentation, Surgery, Arteriosclerosis, Ischaemia / Infarction
Authors:
A. Panajotu, Z. Mihály, B. Szilveszter, F. I. Suhai, L. Entz, P. Sótonyi, P. Maurovich-Horvat; Budapest/HU
DOI:
10.26044/ecr2019/C-2495
Methods and materials
In our prospective study at Semmelweis University,
Heart and Vascular Center between January 2016 and May 2017 out of the total of 476 surgical carotid artery reconstruction patients 60 (23 female,
37 male) were included.
Inclusion criteria were the informed consent,
age under 75 years,
adequate quality preoperative carotid CTA with Philips Briliance iCT 256 scanner and preoperative cranial MRI with Philips Achiva 1.5T.
CTA analysis:
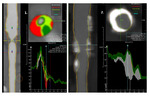
The CTA images of the plaques were analysed with the Medis AngioQ software by two independent observers.
For plaque quantification each dataset was loaded separately and after automated segmentation of the carotid bifurcation the proximal and distal end points of each plaque were set manually.
After semiautomated delineation of the outer and inner vessel-wall boundaries and cut off of the external carotid artery we used different density thresholds to identify separate plaque features.
We differentiated four types of plaque components: calcified (density>130 HU),
fibrotic (90 - 129 HU),
fatty fibrotic (30 - 89 HU) and lipid (29 - -100 HU).
The volume of each plaque components was calculated (Károlyi et al.
2017).
For plaque localization and morphology assessment we used a commercially available DICOM viewer (Osirix,
version 5.5.1).
The lesions were divided into two groups by localization (only affecting the internal carotid artery or the bifurcation and the internal carotid artery as well).
The severity of the lesion calcification was classified in Linker scale 0-2 (0: no calcification,
1: minor calcification,
2: severe calcification).
Finally the presence of positive remodeling was assessed.
MRI image evaluation:
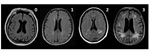
The cerebral ischemic lesions on MRI were classified by the Fazekas-scale (0-3) on the T2 weighted FLAIR (fluid-attenuated inversion recovery) images (Fazekas et al.
1987) by two independent readers.
This classification is the most widely used for the quantificatioin of deep white matter chronic ischemic lesions.
A score of 0 is given in the absence of hyperintense white matter lesions,
1 for small punctate lesions,
2 if the lesions are sporadically confluent and 3 if there are large areas of confluent high intensity areas.
We assigned grades to each patient according to the severity of white matter lesions of the cerebral hemisphere ipsilateral to the stenotic ICA.
Lesion localization was defined and recorded according to the study done by Weber et al.
on silent ischemic lesions on MRI (Weber et al.
2012).
A P value of 0.05 was considered significant.
Statistical analysis was performed using SPSS (IBM Corp,
version 22.0,
Armonk,
NY,
USA).