The IFs were 31.6% of all the pathological findings obtained and grouped by anatomical units.
We did not find statistically significant differences between different groups.
However,
we observed grouping tendencies due to the characteristics of each entity or pathology group: the group of critical CHD was by far the group in which we found the highest frequency of IFs.
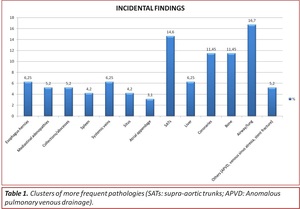
Table 1
In this work,
we tried to reflect the prevalence and the impact of IFs,
both cardiovascular and extracardiac in the patient’s management.
All these findings were not directly related to the initial diagnostic suspicion provided by the clinician,
resulting in a diagnostic surprise.
We registered a total of 396 (31.6%) findings that were not suspected initially before the CT exam.
We can affirm that there are associations of IFs that over the years we have learned to relate to each basal cardiopathological entity,
but that their finding must indicate urgency (thrombi,
effusion,
ascites,
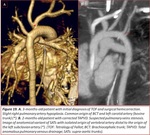
adenopathies… Fig. 1,
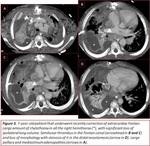
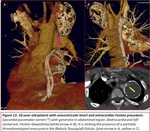
Fig. 2,
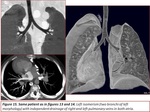
Fig. 3,
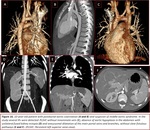
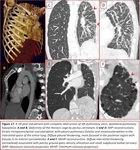
Fig. 4,
Fig. 5,
Fig. 6),
severity (stenosis,
extraanatomical collateral circulation,
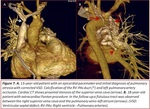
tumor… Fig. 7,
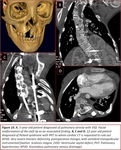
Fig. 8),
or simply part of a pathological complex encompassed in a syndrome (Alagylle,
Poland,
Marfan,
VACTER,
Ivermark...
Fig. 9,
Fig. 10,
Fig. 11).
Taking into account these complex entities,
the difficulty appears when thinking that the IFs that we found can be part of the complex and therefore could no longer be considered as such.
However,
with the premise of focusing on the indication to perform the study,
always cardiac pathology,
these findings could be considered IFs.
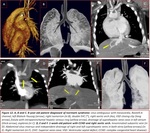
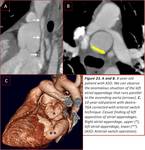
Fig. 4 Fig. 12,
Fig. 13,
Fig. 14,
Fig. 15,
Fig. 16,
Fig. 17.
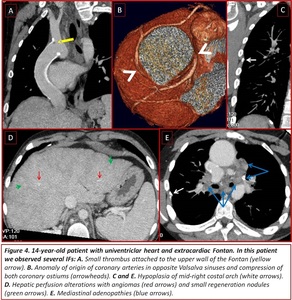
Fig. 4
The most frequent IF were the vascular findings (IVFs) (31.1%).
The most frequent IVF pathology groups were major aortopulmonary collateral arteries (MAPCAs) (21.6%),
persistent left superior vena cava (PLSVC) (15.3%) and anomalous pulmonary venous drainage (APVD) (11.3%).
Variants of development of the supra-aortic trunks (SATs)(14.6%) Fig. 18,
Fig. 19,
Fig. 20,
and coronary anomalies (11.45%) were present in a lot of patients.
The group of complex CHD was by far the group in which we found the highest frequency of IFs.
There is an evident predominance of association with aortic pathology in congenital airway abnormalities and APVD.
Fig. 7 Fig. 18,
Fig. 19,
Fig. 20,
Fig. 21,
Fig. 22.
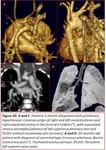
We must not forget the IFs that affect the atrial appendages,
which are relatively frequent in CHDs and difficult to identify by not specialized radiologists.
Fig. 23.
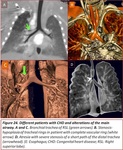
The most frequent non-vascular findings were airway and lung disease (16.7%) Fig. 6,
Fig. 17,
Fig. 6,
Fig. 24,
Fig. 25, bone disorders (11.45%) Fig. 8,
Fig. 22,
Fig. 26,
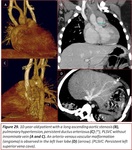
Fig. 27 and liver alterations (6.25%).
Fig. 28,
Fig. 29.
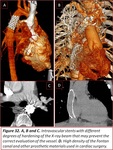
Cardiac CT is the gold standard technique for evaluating airway stenosis of a vascular or non-vascular cause that often precipitates respiratory distress or failure of ventilator withdrawal in children with CHD.
Volumetric images are especially useful not only to demonstrate vascular compression but also help to make appropriate surgical approaches or interventionist treatment.
In our work,
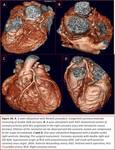
the study of coronary arteries accounts for 11.45% of all abnormalities and more than half are congenital anomalies. Fig. 4,
Fig. 30.
As in the literature,
most of the cases we have found are unexpected findings,
which are detected when carrying out studies with other indications or main diagnoses. Patients with complex CHD have a higher prevalence of CAAs (15.11%),
which should be considered before surgery.
Although hepatic lesions described in the literature include adenoma or focal nodular hyperplasia,
we did not find any cases of these pathologies during the study period. Several cases of focal nodular hyperplasia and abdominal and mediastinal neuroblastoma were observed in subsequent MRI controls of three of our patients.
Our most frequent hepatic findings consisted of vascular lesions with angiomas or venous fistulas,
as well as some cases of cirrhosis and/or liver transplantation associated with Alagille syndrome.
Fig. 28,
Fig. 29.
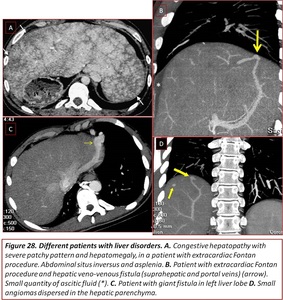
Fig. 28
Likewise,
splenic alterations recorded consisted mainly of splenomegaly associated with Fontan and asplenia and polysplenia associated with visceral-atrial situs anomalies.
Fig. 8,
Fig. 12,
Fig. 28.
Bone alterations were as frequent as coronary anomalies in our study (11.45%).
These findings are usually quite easy to detect,
being the isolated findings vertebral or rib alterations.
The most serious pathological lesions usually accompany syndromic pathological complexes.
Fig. 8,
Fig. 10,
Fig. 22,
Fig. 26,
Fig. 27.
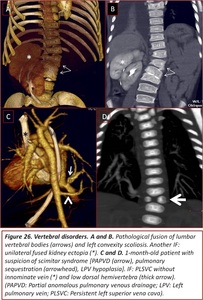
Fig. 26
Other findings such as severe calcification of ducts,
pacemaker leads,
or embolization coils are not always reflected in the patient's clinical history and for the radiologist,
they represent an incidental finding that may alter the patient's management and/or the quality of the study.
Fig. 5,
Fig. 31,
Fig. 32,
Fig. 33.