MATERIAL AND METHODS
Imaging exams of 17 patients with "aggressive" DAVF confirmed by DSA (cavernous cranial DAVF were excluded),
which occurred in the last 4 years in our hospital were reviewed,
to find out imaging clues that could suggest the diagnosis in the conventional CT and MR.
One of our patients had two fistulas at the same time Fig. 11 so 18 cases of DAVF were available to study.
RESULTS
There was not significant differences between men and women (9 males and 8 females).
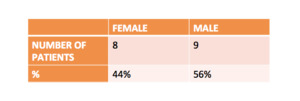

Fig. 3: Distribution of the DAVF according the sex of the patients.
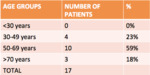
The most representative age group was between 50 to 69 years (59%),
and the average age was 62 years.
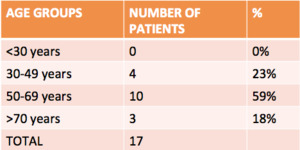
Fig. 2: Distribution of the DAVF according to age groups.
DAVF with CVD occasionally have acute clinical symptoms at the diagnosis,
including acute intracranial haemorrhage,
seizure,
focal neurological deficit,
cognitive change,
dementia and altered level of consciousness.
Eleven of our patients had an acute clinical presentation,
and nine of them were diagnosed as a brain stroke before the radiological images.
At the time of the diagnosis,
29% of our patients were asymptomatic and the fistula was an incidental finding.
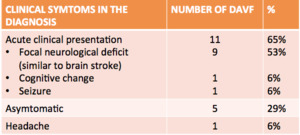
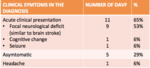
Fig. 4: Distribution of the clinical symptoms of DAVF at the diagnosis.
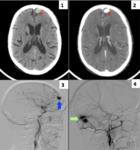
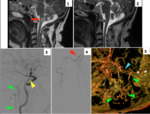
In our serie the most frequent locations involve in the fistulae were firstly the transverse-sigmoid sinus (38%) Fig. 7,
Fig. 9, and secondly the tentorium (33%) Fig. 8, Fig. 11.
Superior sagital sinus (17%) Fig. 12 ,
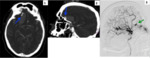
anterior cranial fossa (6%) Fig. 10,
Fig. 11 and straight sinus (6%) are uncommon locations for DAVF.
Just one of the patients presented Cognard grade V fistulae Fig. 13.
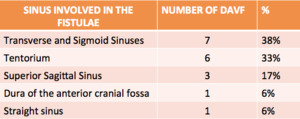
Fig. 5: Distribution of the locations of the DAVF in our serie.
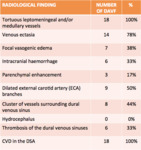
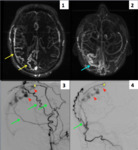
Abnormal tortuous and dilated leptomeningeal or medullary vessels were found in the 100% of our patiets.
Other findings presented in a high percentage or the exams were venous ectasia (78%),
dilated ECA branches (50%),
vasogenic edema (38%),
sinus thrombosis (33%) and intracranial haemorrhage (33%).
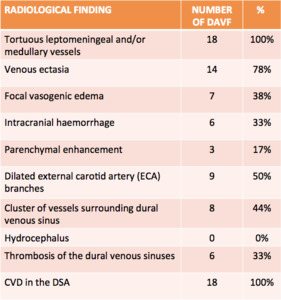
Fig. 6: Distribution of the radiological finding of our patients at the diagnosis of the DAVF.
DISCUSSION
The first steps in the work-out of patients with clinical suspicion of intracranial disease,
are usually contrast-enhanced computed tomography (CECT),
non-enhanced CT (NECT),
and magnetic resonance (MR).
Non-enhanced CT and MR imaging can often appear normal in benign DAVF,
therefore we have focussed our study in the aggressive forms.
Radiologic features that suggest DAVF are:
- Abnormally tortuous leptomeningeal and/or medullary vessels
- Venous ectasia
- Focal vasogenic edema
- Intracranial haemorrhage
- Parenchymal enhancement
- Dilated external carotid artery (ECA) branches
- Cluster of vessels surrounding dural venous sinus
- Hydrocephalus
- Thrombosis of the dural venous sinuses
It has been reported in some scientific articles,
that the imaging findings,
which were significantly associated with the presence of “aggressive” DAVF,
were: dilated leptomeningeal and medullary vessels,
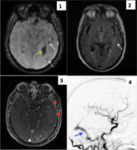
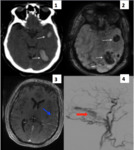
focal venous ectasias and vasogenic edema Fig. 7 . Dilated leptomeningeal was largely the most common finding associated with CVD (82-96%).
Another findings were linked with CVD such as parenchymal enhancement,
dilated extracranial ECA branches,
and clusters of vessels surrounding dural venous sinus,
although they did not achieve the statistical grade of association.
Intracranial haemorrhages in ruptured DAVF are frequently intraparenchymal,
usually lobar and could be multiple.
They may be remote from the location of the arteriovenous shunt.
Subarachnoid haemorrhages are less common,
often associated with DAVF Cognard type V (venous drainage directly into spinal perimedullary veins).
Intraventricular haemorrhage may be present as a result of the extension of intraparenchymal or subarachnoid haemorrhage.
Subdural and epidural hematomas are extraordinary rare.
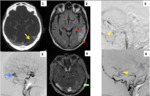
Six of our patients had intracranial haemorrhage,
five of them intraparenchymal Fig. 8 Fig. 9 Fig. 10 ,
and one intraventricular,
just one of the intraparenchymal haemorrhages was multiple Fig. 7 .
Thrombosis of the major dural venous sinuses has a reported incidence ranging from 39 to 68% in different articles,
in our serie it was presented in the 35%,
and in all those cases the thrombosis were next to the fistula.
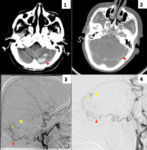
It is not extraordinary to find an acute venous thrombosis at the time of DAVF diagnosis Fig. 14 ,
probably because it produces an acute worsening of the venous drainage,
which leads to venous infarct or hematoma with the corresponding clinical symptoms.
Nevertheless,
the thrombosis sometimes appears before the fistulae formation,
as it is thought to be one of the potential factors contributing to DAVF development.
Hydrocephalus is an infrequent finding in non-cavernous cranial DAVF,
it is produce by a decrease in the pressure gradient for CSF reabsorption,
due to venous hypertension within periventricular and medullary veins.
In the most severe cases,
the blockage of CSF drainage can lead to congestive encephalopathy,
which is clinically manifest as dementia.
We did not found in our serie any case of hydrocephalus related to DAVF.
Althoug DSA is the gold standard for the diagnosis of intracraneal DAVF,
due to its high spatial and temporal resolution,
radiologists should be aware of this wide spectrum of findings to suspect DAVF and perform more specific studies,
such as dynamic angiographic MR and CT,
which are generally not routinely performed unless suspicion of a vascular pathology.
TREATMENTS AND TECHNIQUES
Patients with benign fistulas (Borden I and Cognard I,
IIa) could benefit from conservative management,
with low rate of severe complications.
Treatment may be considered to relieve their symptoms.
However,
they should undergo clinical and imaging follow-up due to the small risk of transformation in an aggressive lesion.
On the other hand,
malignant type of DAVF and patients with alarm clinical presentation that should be promptly treated.
The aim of the treatment is to close the fistula either by endovascular therapy or by surgical methods.
» Endovascular embolization is the treatment of choice for DAVF.
The target is the elimination of fistulisation between arteries and draining veins.
Partial embolization could reduce the symptoms but usually does not cure the lesion,
moreover it may change the venous drainage pattern and at the end induce cortical venous reflux.
Sometimes the complete obliteration of the fistulae is not possible in a first attempt and it needs several endovascular sessions Fig. 14 Fig. 15 Fig. 16 .
Embolization of DAVF can be accomplished using particulates,
microcoils,
or liquid embolic agents (such as n-butyl cyano- acrylate (n-BCA) more used in the past,
or ethylene vinyl alcohol copolymer (Onyx)).
Depending on the access to the fistulae we can separate the techniques in:
- Transvenous embolization is a good option when the draining veins do not participate in the normal cerebral venous system and also when the DAVF is feeded by multiple arterial pedicles.
The principal complications are venous infarction and dural sinus perforation.
- Transarterial embolization is usually performed with liquid embolic agents because of the high rate of fistula recurrence using particulates,
and also due to the high effectiveness of the liquid embolic treatment in permanent fistula closure (if the agent cross the lesion).
Specific risks are: microcatheter entrapment,
retrograde penetration of non-caheterized article pedicles,
and venous penetration (could be avoided by disposal coils before the liquid injection).
» Surgical repair is a secure and efficient therapy for cranial DAVF,
and it can be performed alone or jointly with endovascular methods.
It is preferable for anterior cranial fossa fistulaes,
which are supplied by ophthalmic artery meningeal branches.
In comparison with endovascular embolization,
intracranial surgery presents a higher frequency of complications such as arterial and venous infarct,
and haemorrhage.
Therefore this technique is reserved only for lesions that do not respond to endovascular treatment,
or in which this treatment cannot be carried out.
» Stereotactic radiosurgery also play a role in the DAVF treatment,
mainly in “benign” fistulaes,
because it reduces de symptoms (for example tinnitus),
even if the fistula obliteration is not completed.
Complications are uncommon or even zero in some series.
The principal inconvenience is that it could delay the closure of the fistula,
so it is not recommended to use this technique alone in “aggressive” fistulaes.
LIMITATIONS
It is important to highlight the limitations of our review.
Firstly the number of cases is small for a statistical analysis,
and secondly being a retrospective review has the risks of selection and information biases.