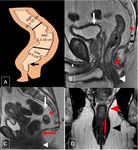
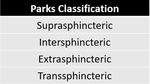
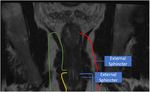
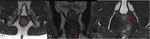
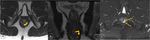
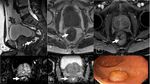
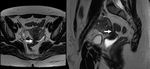
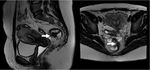
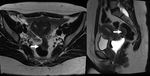
Anorectal anatomy
The rectum is a continuation of the sigmoid colon after the rectosigmoid junction and continues as the anal canal at the anorectal angle created by puborectalis muscle.
At the level of the S3 vertebral body,
the sigmoid colon loses its mesentery and becomes the rectum which is approximately 15 cm long.
The rectum extends from the rectosigmoid junction to proximal anorectal sphincter.
It does not have the distinctive haustra nor epiploic appendages that the rest of the large intestine has.
The lower part of the rectum is dilated and is called the rectal ampulla and there are three semilunar transverse rectal folds,
which project into the rectum.
The rectum can be divided into three parts: the upper,
middle,
and lower rectum.
From the anal verge,
these three parts are defined as following: the lower rectum,
0 to 6 cm; the middle rectum,
7 to 11 cm; and the upper rectum,
12 to 15 cm (figure 1).
The upper third is covered by peritoneum anteriorly and laterally,
the mid third only anterior and its lower third is not covered by peritoneum.
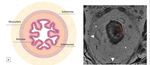
The rectum wall consists of several layers,
which are mucosa with muscularis mucosae,
submucosa,
muscularis propria and surrounding mesorectal fat.
[3,4](figure 2)
The rectum continues on as the anal canal at the level of the coccyx tip,
it takes on an acute angle,
the anorectal angle or perineal flexure,
as it passes anterior to the sling of the puborectalis muscle where it becomes the anal canal. The anal canal measures approximately 4 cm long and it is a muscular tube although the muscular layer is circular forming the external and internal anal sphincters. The dentate (pectinate) line separates the anal canal into an upper and lower parts,
not only in structure but also in neurovascular supply,
it is formed by the anal columns,
which consists of a series of anal sinuses (which drain anal glands),
in the following table there are the differences between the upper and lower anal canal [4] (table 1).
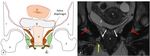
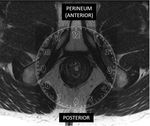
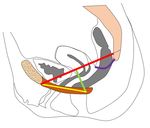
The supporting female pelvic floor structures consist of a complex of fascia,
ligaments and muscles,
these structures form three contiguous layers: the endopelvic fascia,
the pelvic diaphragm,
and the urogenital diaphragm [5,6] (figure 3 and 4).
MRI protocols
The MRI protocol includes multiplanar imaging and a high degree of soft-tissue differentiation,
which allows the evaluation of the anorectal anatomy and the surrounding structures.
The resonance equipment should have a magnetic field of 1.5 to 3.0T.
The patient should be positioned comfortably in the dorsal position.
The appropriate coil must be positioned covering from aortic bifurcation to anal verge.
To achieve the correct orientation,
a sagittal fast spin-echo (FSE) T2-weighted images (WI)sequence should be performed initially,
providing an overview of the pelvis and showing the extent and axis of the anal canal (figure 5).
The correct orientation of the anal canal for MR imaging can be derived from this sequence,
providing truly axial and coronal images along the long axis of the anal canal.
The levator plate and the entire perineum should be included.
The following sequences are oblique axial T1WI FSE,
oblique axial T2WI FSE,
if the contrast is used the others sequences peformed are oblique axial and oblique coronal fat-suppressed T1WI FSE with gadolinium-based contrast material,
oriented perpendicular or parallel to the long axis of the anal canal.
The rectum and anal canal MRI is routinely performed with IV contrast,
except for the evaluation of endometriosis and rectal tumor.
To evaluate the pelvic floor the images are obtained while the patients is at rest and during the Valsalva maneuver [3].
There is no need of bowel preparation and endorectal coil.
In some cases,
the use of spasmolytic agents,
such as scopolamine,
is recommended.
Microenema may also be done to remove the rectal air,
in order to reduce diffusion weighted images (DWI) artifacts.
Anorectal benign diseases
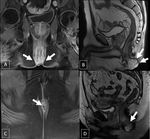
Anal fistula (figure 6 – 12)
Perianal fistula is an inflammatory condition that affects the region around the anal canal,
in which a connection (fistula) occurs between the anal canal and the skin of the perineum.
Generally,
the treatment of the anal fistulas requires surgery,
because of its high tendency to recur,
requiring a precise radiological evaluation to assess the location and extent to the pelvic structures [7,8].
(table 2-3)
Main sequences to evaluate:
T2WI FSE: anatomy.
Oblique axial and oblique coronal fat-suppressed T1WI FSE with gadolinium: fistula.
[9,10]
What the radiologist needs to report:
1.
Classification: intersphincteric,
transsphincteric,
extrasphincteric and suprasphincteric.
2. Position of the fistulous orifice in the anal mucosa (hours): evaluated in the axial plane.
3. Distance from the fistula to the skin: coronal plane.
4. Define the anatomic relationships.
5. Secondary fistulas,
abscesses or other complications.
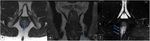
Proctitis in inflammatory bowel disease (ulcerative colitis)
The ulcerative colitis (UC) is an inflammatory bowel disease thats tipically manifests in young adults and is more prevalent in males.
It usually springs from the rectum and extends proximally by contiguity and is limited to the mucosa and submucosa.
The MRI findings can be divided into acute and subacute / chronic phases.
The acute phase is marked by hyperenhancement of the mucosa,
progressive mucosal edema (wall thickening) and high T2WI signal.
The subacute / chronic phase is seen as a widening of presacral space,
with incresead perirectal fat volume often accompanied by a narrow rectum due to a circumferential thickening caused by muscularis hypertrophy and submucosal fat deposition; varying degrees of mucosal inflammation can be present (figure 13).
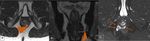
Polyps
The rectal polyps are more common in older patients and the prevalence ranges from 7-50%.
They can be divided histologically as malignant or benign,
hyperplastic,
harmatomatous or inflammatory.
The benign polyps or adenoma can be tubular,
tubulovillous or villous,
they are typically sessile,
less commonly pedunculated and the villous adenoma rectal polyps appear carpet-like or nodular.
The hyperplastic polyps have no malignant potential and are usually <5 mm.
The polyp presents as an intraluminal mass filling the lumen [11].
(figure 14)
Prolapse
An enterocele or rectocele is a herniation that indicates loss of posterior muscular support.
Descent and anterior bulging if the rectum indicates a rectocele.
Generally,
the patients complain of incomplete evacuation.
This type of pelvic floor weakness is usually due to disruption of the supporting ligaments and the iliococcygeus muscle with subsequent widening of the rectovaginal space [5,6].
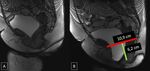
To evaluate the pelvic floor images,
the radiologist should identify the pubococcygeal line,
that represents the level of the pelvic floor,
the H and M lines,
which are helpful to confirm pelvic floor laxity,
and the angle of the elevator plate with the pubococcygeal line that helps the identification of small bowel prolapse [5,6].
The pubococcygeal line extends from the last joint of the coccyx to the inferior aspects of the pubic symphysis,
this measure should be obtained at rest and at maximal pelvic strain,
the organ descente greater than 1 cm below the pubococcygeal line indicates pelvic floor laxity.
The H line is the anteroposterior width of the levator hiatos and extends from the inferior aspect of the pubic symphysis to the posterior wall of the rectum,
at the level of the anorectal junction (normal < 6mm).
The M line is the vertical descent of the levator hiatus and is drawn as a perpendicular line dropped from the pubococcigeal line to the most posterior aspect of the H line (normal < 2mm).
The angle of the levator plate with the pubococcygeal line is measured,
normally,
the levator plate will parallel the pubococcygeal line at rest and during the pelvic strain.
Increasead caudal inclination is an indicator of loss of posterior muscular support.
Descent of the small bowel more than 2 cm between the vagina and rectum is an indicative of enterocele.
Anterior bulging of the rectum is evidence of an anterior retocele.
(figure 15-17 and table 4)
The MRI finding report should detail the location and number of the pelvic compartments that demonstrate laxity.
The location of muscle tears and inferred fascial tears should also be specified.
The supporting measures as H line,
M line and angle of the elevator plate can be reported [5,6].
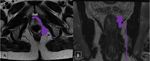
Hemorrhoids
Hemorrhoids are an ingurgitation of blood vessels in the lower rectum.
There are three types of hemorrhoids as follows: (a) external hemorrhoids that are located distal to the dentate line; (b) internal hemorrhoids located proximal to the dentate line; and (c) mixed hemorrhoids located both proximal and distal to the dentate line.
Clinically,
the hemorrhoids may show perianal itching,
pain,
bleeding or inflammation.
At the MRI,
it shows as enlarged blood vessels around the anus and the lower rectum.
The hemorrhoids may complicate with thrombosis that present with acute pain around the perianal surface and in the contrast-enhanced T1WI will demonstrate lack of flow or heterogeneous enhancement [12].
(figure 17)
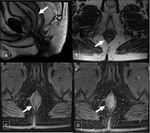
Endometriosis (figures 18 – 21)
Endometriosis is defined as the presence of functional endometrial tissue outside the uterine cavity.
It is mainly found in the abdominal cavity,
most commonly on the surface of the ovaries.
The deep pelvic endometriosis frequently presents with pelvic pain and is defined as subperitoneal invasion that exceeds 5mm in depth.
Pelvic MRI is a noninvasive method with high spatial resolution that allows multiplanar evaluation of deep pelvic endometriosis.
The intravaginal gel is not essential but is frequently administered to distend the vaginal cavity facilitating the evaluation of the retrocervical area and vaginal fornices.
The endometriotic lesions usually demonstrate low signal intensity on T2WI and intermediate to high signal on T1WI.
Sometimes,
a punctate foci of high signal intensity are seen on T2WI which indicates a dilated endometrial gland.
A lesion with high signal intensity on T1WI,
if it remains with a high signal intensity on T1WI with fat saturation,
characterize a hemorrhage.
The T1WI with fat saturation sequence is important to differentiate lesions with high signal on T1WI,
as blood or immature cystic teratoma,
the last one will lose sign at the fat saturation sequence [3].
Main sequences to evaluate:
- Fat-suppressed T1WI: sensitive for bloody foci.
- T2WI: evaluation of fibrotic lesions.
The rectum wall involvement should be suspected when it has a thickened or nodular appearance on T2WI with low signal intensity and with retractile appearance.
The rectosigmoid is the bowel part that is most commonly involved by endometriosis.
Generally,
the implants are restricted to serosal,
but may infiltrate subserosal layers.
The presence of hypointense parietal thickening on T2WI is the most helpful finding in making the diagnosis.
But,
be careful,
black plaques can be mistaken for the black gas contents of the rectum.
Some complications as adhesions and gastrointestinal obstruction may result from the inflammatory response to cyclic hemorrhage [3].
- What the radiologist needs to report:
1. Depth of endometrial involvement.
2. Percentage of involvement of the bowel wall.
3. Distance of the lesion from the anal border