Type:
Educational Exhibit
Keywords:
Kidney, Urinary Tract / Bladder, Interventional vascular, CT, CT-Angiography, Catheter arteriography, Embolisation, Diagnostic procedure, Surgery, Pathology
Authors:
A. Serdio1, M. Gredilla2, M. LETURIA ETXEBERRIA3, A. Aguado4, K. Biurrun Mancisidor2, G. Vega-Hazas Porrúa5; 1Donostia - San Sebastián/ES, 2DONOSTIA/ES, 3San Sebastian, Gipuzkoa/ES, 4San sebastian/ES, 5San SebastiáN/ES
DOI:
10.26044/ecr2019/C-2728
Findings and procedure details
1.
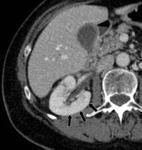
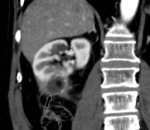
Normal postoperative imaging:
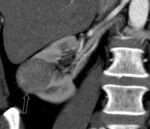
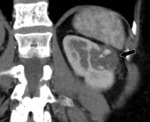
- The postoperative kidney commonly has a more posterior retroperitoneal location (closer to the posterior abdominal wall). Fig. 1
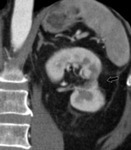
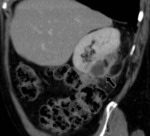
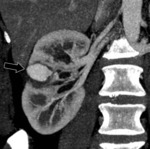
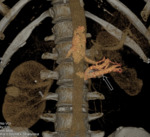
- The appearance of the postoperative kidney depends on the size and the location of the resected tumor. After resection of small peripheral tumor,
a wedgeshaped defect in the renal parenchyma is seen at CT and MR imaging.
Fig. 2
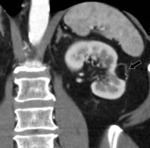
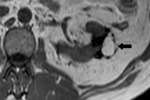
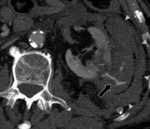
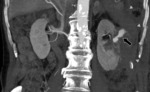
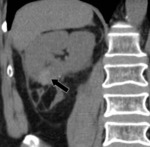
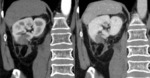
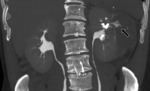
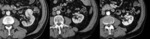
- In some cases,
the surgeon may pack perinephric fat into the surgical bed to help achieve hemostasis.
With time,
the volume of fat used for surgical packing may decrease or remain unchanged.
Fig. 3 Fig. 4 This fatty material may be mistaken for a fatty mass such as an angiomyolipoma.
- The hemostatic material may be biologically absorbable material and contain air pockets or bubbles and resemble a focal abscess.
Usually,
the air is rapidly resorbed during the 1st postsurgical week. However,
in some cases,
air bubbles can be identified on postoperative images even 1 month after surgery.
2.
Infection:
2.1.
Abscess: Fig. 5 Fig. 6
- It may be difficult to differentiate an infected fluid collection from an uninfected one based only on imaging techniques. However,
patients with a postoperative abscess are likely to manifest clinical symptoms and signs (eg,
fever and an elevated white blood cell count) suggestive of infection.
- The presence of an abscess should be suspected if a localized fluid collection that has an enhanced rim and contains gas bubbles or a gas-fluid level is seen.
2.2.
Pielonefritis:
- Patients who have undergone a partial nephrectomy may present with pyelonephritis,
which may appear as a striated or heterogeneous nephrogram.
It may be difficult to differentiate from renal infarction on images alone as both present tipically a triangular shape.
3.
Vascular complications:
Possible serious vascular complications owing to the difficulty recognizing the vascular border and abundant renal vascularity.
3.1.
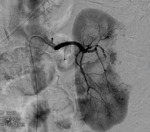
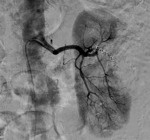
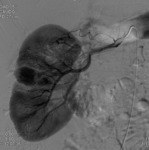
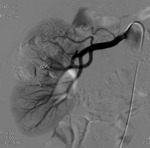
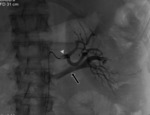
Active bleeding: Fig. 7 Fig. 8 Fig. 9 Fig. 10
- It is the most relevant complication after PN.
- Large tumors or those with central location have been correlated with an increased risk of hemorrhage.
3.2.
Hematoma: Fig. 11 Fig. 12
- Hematoma may result if the suturing of transected blood vessels is inadequate.
3.3.
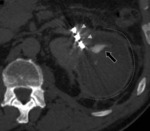
Pseudoaneurysm: Fig. 13 Fig. 14 Fig. 15 Fig. 16
- A pseudoaneurysm may result from injury to an intrarenal artery at the surgical site or to the main renal artery or one of its major branches.
- It is a sack with turbulen blood flow inside secondary to incomplet or contained rupture of the wall of an artery.
It is a vascular emergency.
3.4.
Arteriovenousus fistula: Fig. 17 Fig. 18 Fig. 19
- Arteriovenousus fistula is a communications between an artery and a vein,
characterized by arterialization of venous flow.
- CT shows early filling of the renal veins in the arterial phase.
Digital subtraction angiography (DSA) with selective embolization is an efficacious technique for appropriate management of vascular complications providing minimally invasive treatment without the need for re-operation.
4.
Collecting system complications:
4.1.
Urinary leakage:
To ensure an adequate margin of resection for deep tumors,
calyceal entry is often necessary and calyceal repair then would be required,
to avoid urinary leakage.
- Diagnosis on contrast-enhanced CT and MR images acquired during the excretory phase,
with the observation of contrast material leakage from the collecting system into the surgical bed. Fig. 20 Fig. 21
- In most cases,
the fluid collection resolves either spontaneously or after placement of a ureteral stent or nephrostomy catheter.
- Less commonly,
urinary leakage persists and a urinoma forms.
4.2.
Chyluria:
Lymphatic injury is another less known risk of PN. The finding of fat in the bladder (chyluria) is believed to be due to lymphatic injury and persistent connection of lymphatic channels with the renal collecting system (lymphatic-urinary fistula).
- Patients are usually asymptomatic.
- Less commonly,
patients with chronic chyluria can experience hypoproteinemia,
hypolipidemia,
and loss of immune competence.
- CT of the fat–fluid level reveals the supernatant fluid to be hypodense compared with the dependent nonfatty fluid. Fig. 22 Additional evaluation of this finding is generally not needed.
- It is important to differentiate fat,
which is of higher density,
from air in the bladder, often seen as the result of instrumentation.
- Imaging of patients with suspected lymphatic injury previously required lymphangiography. CT is now more widely used for postsurgical evaluation but does not directly show the communication between the collection and lymphatic systems or the injury to the lymphatic vessels.
- Patients who had detectable chyluria on CT do not need surgical intervention and continued to have no significant symptoms after conservative treatment.
It may require surgical intervention if patient presents hypoproteinemia.
5.
Recurrent tumoral:
- At PN,
a small portion of the normal renal parenchyma is excised with the tumor to ensure an adequate resection and a tumorfree margin.
If an adequate margin is not obtained and surgical excision is incomplete,
the growth of any remaining neoplastic cells at the resection site over time may result in tumor recurrence in the surgical bed. Fig. 23
- The surgical field of view during laparoscopic partial nephrectomy is limited,
and the surgeon can see only a small portion of the kidney.
In a patient with multiple foci of disease,
an apparent tumor recurrence may actually be an additional preexistent renal cell carcinoma that either was not depicted at preoperative imaging or was not identified intraoperatively.
6.
Other complications:
6.1.
Rabdomylysis in patient undergoing PN in lateral decubitus position. Fig. 24
During the laparoscopic partial nephrectomy,
the patient remains in lateral decubitus for a long time.
The laparoscopic/robotic approach supposes a longer duration of the intervention.
This position can produce rhabdomyolysis by compression.