Type:
Educational Exhibit
Keywords:
Oedema, Neoplasia, Ischaemia / Infarction, Surgery, Education, MR, CT, Trauma, Neuroradiology brain, Emergency
Authors:
S. Caruso1, P. V. Foti1, M. Travali2, M. Coronella1, R. FARINA3, S. Palmucci1, P. Milone1, A. Basile1; 1catania/IT, 2Catania, Catania/IT, 3Catania, IT/IT
DOI:
10.26044/ecr2019/C-2732
Background
Brain herniation represents a shift of brain parenchyma across anatomical boundaries formed by intracranial bony ridges and dural folds (falx cerebri,
tentorium cerebelli,
falx cerebelli and the diaphragm sellae).
Brain herniation occurs when an expanding mass lesion including tumors,
hematomas,
infarctions,
infection,
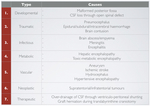
or haemorrhage exhausts the limited capacity of intracranial cavity (Table 1).
Development of herniation due to mass effect depends upon many factors including patient age; size,
location and progression rate of mass lesion; pressure gradient between mean blood pressure,
cerebrospinal fluid and brain tissue.
Chronic lesions usually present as severe anatomic herniation with few initial neurological manifestations.
In contrast,
a rapidly enhancing mass lesion may result in profound and dreaded neurological deficits.