The skull is a rigid bone structure occupied by the brain,
the cerebrospinal fluid,
the blood vessels and the meninges,
with a single wide opening (foramen magno).Meninges consist of three membranous connective tissue layers: dura mater,
arachnoid mater and pia mater.
The dura mater is a thick fibrous membrane consisting of two laminae: the outer dural layer adheres intimately to the periosteum of the skull; the inner dural layer forms voluminous folds that deepen in the brain by dividing the cranial cavity into various compartments and protecting the brain from excessive movements.
These dural reflections are falx cerebri,
tentorium cerebelli,
falx cerebelli and the diaphragm sellae.
The falx cerebri separates the right and left hemispheres from each other,
whereas the tentorium cerebelli separates the supratentorial from the infratentorial compartment.
Brain,
cerebrospinal fluid and blood all coexist in a rigid bone box.
Under normal conditions,
pressures within the brain parenchyma and intracranial cerebrospinal fluid spaces are equal.
The Monro-Kellie hypothesis state,
“The sum of volumes of brain,
cerebrospinal fluid,
and intracranial blood is constant in an intact skull.
An increase in one should cause a decrease in one or both of the remaining two”.
Accordingly,
any increase in intracranial volume requires a compensatory and equal decrease in the other contents.
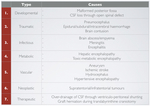
The pathological increase in intracranial pressure occurs when there is an increase in the volume of one or more of its components:
- increase in brain volume: expansive lesions (hematomas,
tumors,
abscesses),
increase in the intracerebral water content (cytotoxic and vasogenic edema)
- increase in blood volume: hyperemia from congestive obstruction of venous return (venous thrombosis)
- increase in the volume of liquor: hydrocephalus hypertensive (obstructive or non-obstructive)
Initially the small volume increases of a cerebral expansive mass can be compensated by the reduction of the volume of the liquor and of the blood volume; when the volumetric increase is noticeable or occurs in a short time,
however,
it creates a decompensation with acute or subacute onset of intracranial hypertension.
The brain,
liquor spaces and blood vessels are moved from an intracranial compartment to the adjacent one,
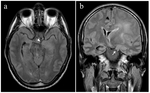
resulting in one or more brain hernias (Fig. 1).
Owing to its widespread availability and short examination time,
computed tomography (CT) is usually performed as a first step in the emergency setting to identify underlying primary pathology that requires immediate medical and/or surgical approach; magnetic resonance (MR) imaging may be performed subsequently for more accurate categorization of lesion or associated complications.
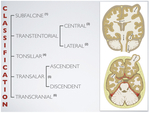
According to which anatomic boundary the herniating structure crosses,
five varieties of cerebral herniation are described: subfalcine,
transtentorial,
tonsillar,
transphenoidal and transcalvarial herniation (Table 2).
- Subfalcine herniation is the most common brain herniation.
It occurs when a supratentorial mass causes midline shift of brain tissue under the falx cerebri. It extends anteriorly from crista galli,
where it is narrow,
to the internal occipital protuberance posteriorly,
where it broadens,
which makes it more resistant to any pressure effect in the posterior portion.
For this reason,
subfalcine herniations are more common anteriorly.
Falx cerebri is in close relationship with anterior cerebral artery,
cingulate gyrus inferio-medially,
internal cerebral veins,
vein of Galen and deep subependymal veins posteriorly.
Any mass effect in this region can lead to brain ischemia as a result of arterial compression or brain parenchymal congestion and/or raised intracranial pressure due to compression of venous system.
The severity of herniation may vary from mild with minimal midline shift to complete herniation of the cingulate gyrus and the adjoining parenchyma.
Continued mass effect compresses the ventricular system including ipsilateral lateral ventricle and foramina of Monro with enlargement of contralateral lateral ventricle and consequent obstructive hydrocephalus.
Subfalcine herniation can occur in isolation or in conjunction with transtentorial herniation.
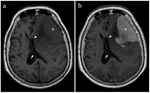
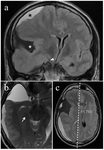
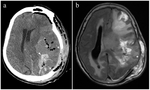
Imaging signs of subfalcine herniation include unilateral mass effect causing subfalcine shift of brain to the contralateral side,
asymmetry of the anterior falx with a widened cerebrospinal fluid space on the contralateral anterior falx (Fig. 2).
The easiest method for evaluating subfalcine shift on axial CT images is a straight line drawn in the expected location of the septum pellucidum from the anterior to posterior aspect of the falx.
Shift of the septum pellucidum from this midline can be measured in millimeters and compared over time to determine any change (Fig. 3).
Shift of the median line greater than 15 mm correlates with a poor prognosis,
while shifts of less than 5 mm do not affect the patient's clinical outcome.
- Transtentorial herniation is upward or downward shift of neural parenchyma across the tentorium at level of incisura.
The tentorium cerebelli is a crescent shaped lamina,
attached anteriorly to the clinoid processes of sphenoid bone,
anterolaterally to the petrous part of the temporal bone,
and posterolaterally to the internal surface of occipital and parietal bone.
Superiomedially,
tentorium cerebelli continues as falx cerebri; while,
the concave anteriomedial margin of the tentorium between clinoid processes is free,
leaving a semiovular opening known as tentorial notch or incisura.
The principal structures coursing through the incisura include midbrain,
occulomotor nerve,
posterior communicating artery,
posterior cerebral artery and superior cerebellar artery.
Transtentorial herniation can be further subcategorized into ascending,
descending and uncal.
Uncal herniation is an early or unilateral descending transtentorial herniation that occurs when innermost portion of temporal lobe,
the uncus is pushed over the free edge of the tentorial incisura.
Furthermore,
uncus obliterates the supracellar cistern and the aqueduct of sylvius and compresses the cerebral peduncles and occulomotor nerve with loss of parasympathetic innervation resulting in pupillary dilation and loss of light reflex.
Uncal herniation can also compress the posterior cerebral artery resulting in ischemia of ipsilateral primary visual cortex,
with consequent contralateral visual field defects in both eyes (Homonymous hemianopia).
Pressure effect upon ipsilateral cerebral peduncle (comprises corticospinal and corticobulbar fibres) results in contralateral hemiparesis.
In contrast,
uncus may also compress contralateral cerebral peduncle against the tentorium cerebelli,
resulting in ipsilateral hemiparesis (false localizing sign,
known as Kernohan’s notch).
“Top-down” mass effect displaces the midbrain inferiorly and closes the midbrain-pontine angle.
Perforating arteries that arise from the top of the basilar artery are compressed and buckled inferiorly,
eventually occluding and causing a secondary hemorrhagic midbrain infarct know as a Duret’s hemorrhages which can be fatal.
Axial CT scans,
in uncal herniation,
show that the uncus is displaced medially and the ipsilateral aspect of the suprasellar cistern is effaced (Fig. 4).
As herniation increases,
the hippocampus also herniates medially over the edge of the tentorium,
compressing the quadrigeminal cistern and pushing the midbrain toward the opposite side of the incisura.
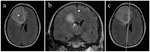
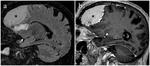
Descending transtentorial herniation can also be bilateral (or central) and occurs when a midline/bilateral supratentorial mass pushes the diencephalon and or the parahippocampal gyrus inferiomedially from the supratentorial space into the incisura,
obliterates basilar cisterns and compresses occulomotor nerve,
midbrain,
posterior cerebral artery and anterior choroidal artery (Fig. 5).
With further increase in herniation,
pons and medulla are also compressed.
In severe cases,
occlusion of small perforating branches supplying the upper brain stem results in brain stem haemorrhage (Duret’s hemorrhages).
In complete bilateral descending transtentorial herniations,
perforating arteries that arise from the circle of Willis can be compressed against the central skull base and also occluded,
causing hypothalamic and basal ganglia infarcts.
Ascending transtentorial herniation results from upward migration of brain parenchyma through the incisura due to an expanding mass lesion within in the posterior fossa.
Herniated brain tissue includes central lobule,
culmen,
and cerebellar vermis,
which compresses the dorsal mid brain,
fourth ventricle,
pretectum and the cerebral aqueduct (Fig. 6).
Pretectal compression leads to loss of vertical eye movements.
Increasing pressure effect compresses the pons,
leading to loss of sympathetic innervation descending through the pontomedullary region.
Thus,
the unopposed parasympathetic papillary supply to the eye leads to small minimally reactive pupil,
termed as ‘pontine pupil’.
However,
coexistent compression of midbrain and third nerve may also cut the parasympathetic supply,
leading to midpositioned or even dilated fixed pupil.
With increasing upward herniation obstructive hydrocephalus develops,
and the quadrigeminal cistern and superior cerebellar cistern become obliterated.
The distal part of superior cerebellar artery and posterior cerebral artery may get compressed,
resulting in infarction of cerebellar hemisphere and occipital lobe.
Increasing mass effect also compresses the vein of Galen and the basal vein of Rosenthal,
which further exacerbates the neuronal congestion,
resulting in rise in intracranial pressure and secondary haemorrhagic infarction of diencephalon.
- Tonsillar herniation can be congenital (e.g.
Chiari 1 malformation) or acquired.
In acquired tonsillar herniation,
increased pressure gradient within the posterior fossa pushes the cerebellar tonsils through the foramen magnum.
Acute tonsillar herniation can cause significant compression upon the medulla,
posterior inferior cerebellar arteries and fourth ventricle which can be fatal.
Ischemia and infarction of cerebellar tonsil,
lower cerebellum and entire lower brain stem and upper spinal cord may occur due to occlusion of vertebral arteries,
their branches and the origin of anterior spinal artery.
Clinical symptomatology may be subtle or patient may exhibit Lhermitte’s phenomenon,
defined as dyesthesia in arms and legs upon forward bending of head due to pressure upon anterior spinal cord tracts.
Compression of ventricular system may result in obstructive hydrocephalus.
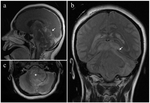
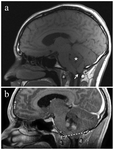
In tonsillar herniation,
radiological findings include downward displacement of cerebellar tonsil up to the level of odontoid process and lesser amount of cerebrospinal fluid in the foramen magnum,
on axial CT images.
A sagittal MR image is however,
a more accurate method for determining the herniation (Fig. 7).
Tonsillar herniation should be differentiated from low lying normal cerebellar tonsils: radiologically,
cerebellar tonsil should lie at least five millimeters below the level of foramen magnum in adults or seven millimeters in children,
to categorize it as herniation.
- Transphenoidal or transalar herniation occurs when a mass lesion shifts brain tissue across the lesser sphenoid wing or “ala”.
There are two types of transphenoidal herniation,
anterior or ascending and posterior or descending.
Ascending herniation is the most common and is produced by middle cranial fossa mass effect with displacement of the temporal lobe,
sylvian fissure,
and middle cerebral artery anterosuperiorly over the sphenoid wing (Fig. 8).
Superior displacement of the temporal lobe can compress the supraclinoid internal carotid artery against the anterior clinoid process and result in infarction of the anterior and middle cerebral artery territories.
Descending herniation is caused by anterior fossa mass effect and occurs when the frontal lobe extends posteriorly and inferiorly over the lesser sphenoid ridge,
causing posterior displacement of the sylvian fissure and the middle cerebral artery resulting in a middle cerebral artery infarction.
- Transcalvarial or transcranial or transdural herniation is a rare form of herniation of oedematous brain tissue through a bony defect,
sometimes called a “brain fungus”.
For transcalvarian herniation three conditions are required: a skull bony defect must be present,
the dura must be lacerated and intracranial pressure must be increased.
Traumatic transcranial herniations typically occur in infants or young children with a comminuted skull fracture that deforms inward with impact,
lacerating the dura-arachnoid.
Iatrogenic transcranial herniations occur when a burr hole,
craniotomy or craniectomy is performed in a patient with severely elevated intracranial pressure.
In transcranial herniations,
MR and CT easily demonstrate the defect and the amount of herniating brain tissue (Fig. 9).
MR imaging is more accurate in detecting small herniations,
especially in post-operative or post-traumatic sites involving the orbit,
sella and middle ear canal.
MR better depicts the disrupted dura as a discontinuous black line on T2-weighted images.