Clinical presentation
LBO may develop over a lengthy period but it’s clinical presentation is often acute and includes abdominal pain,
constipation and abdominal distention.
In the case of acute volvulus the bowel sounds are usually hypoactive,
while in vascular compromise/ischemia,
patients often exhibit substantial abdominal tenderness.
Pathophysiology
The visceral pain of intestinal obstruction is due to increased gut peristalsis against the obstruction.
Rather than being localized,
pain is usually referred towards the midline,
reflecting the gut’s embryological origin.
Bowel obstruction results in distention of the gut through the accumulation of both gas and fluid,
which causes increased intraluminal pressure that also affects the motility of the intestine: initially causing increased peristalsis and then leading to decreased peristalsis and relaxation.
Radiographic findings
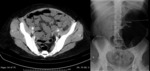
Abdominal radiograph is the first imaging exam performed in cases of suspected bowel obstruction and can diagnose LBO.
There is no consensual agreed cut-off value for dilation of the colon but the most commonly used are 6 cm to the colon and 9 cm to cecum.
The presence of air-fluid levels suggest that the cause of obstruction is acute since the colonic fluid has not been present long enough to be absorbed.
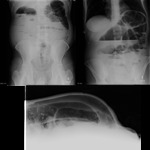
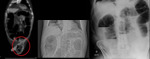
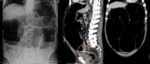
Plain abdominal radiography features of LBO: (Fig.
1)
- the distribution of gas - colonic distension proximal to the obstruction,
and paucity or absence of gas distal to the obstruction
- small bowel dilatation depends on duration of obstruction and incompetence of the ileocaecal valve
- free intra-abdominal gas (if perforation)
- air-fluid levels are often seen in the dilated colon on the upright or decubitus radiographs
Computed Tomography (CT) is essential to establish the diagnosis and site of obstruction but,
in most instances,
it is also able to identify the cause by showing luminal,
mural,
and extramural pathologies.
The detection of LBO with CT has been reported to have a sensitivity and specificity of 96% and 93%,
respectively.
The presence of a transition point is considered a reliable finding for the diagnosis of LBO.
The large bowel will be distended with a thinned stretched wall,
but should enhance (unless ischemic).
Etiology
The underlying etiology of LBOs is age-dependent.
For instance,
in adulthood,
the most common cause is colonic cancer (50-60%),
typically in the sigmoid.
(Fig.
2)
However,
it varies substantially worldwide as does the patient population affected.
- For example in India and Africa the most common cause is volvulus and the patients are usually young and healthy.
The second most common cause in adults is acute diverticulitis (usually involving the sigmoid colon).
Together,
obstructing tumours and acute diverticulitis account for 90% of all causes of LBO.
It is important to note that although adhesions are the leading cause for small bowel obstructions (SBO),
they tend not to cause LBO.
Overall causes include:
- malignancy
- diverticulitis
- volvulus
- adult intussusception
- fecal impactation
- inflammatory bowel disease
- pseudo-obstruction (Ogylvie syndrome; adynamic ileus; toxic megacolon)
- others (adhesions; hernias)
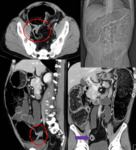
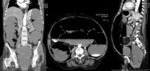
In colonic cancer the two most frequent locations of obstruction are the sigmoid colon and the splenic flexure.
The most common site of perforation in LBO is not at the site of the tumour but at the cecum,
with a reported incidence of perforation of 3–8%.
(Fig.
2,
Fig.
3)
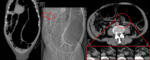
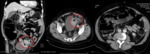
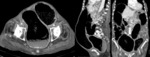
- CT findings include asymmetric and short-segment colonic wall thickening or an enhancing soft-tissue mass centered in the colon that narrows the colonic lumen with or without findings of ischemia and perforation.
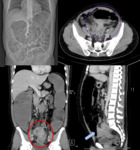
Volvulus represents one of the most common causes of LBO.
Sigmoid volvulus is three to four times more common than cecal volvulus and occurs mostly in the elderly,
who have an elongated and chronically dilated sigmoid colon.
Classic signs describing the findings of colonic volvulus include the coffee bean and bird beak signs on plain radiographs.
A specific CT sign for volvulus is the whirl sign,
an appearance of spiraled loops of collapsed bowel with enhancing engorged vessels radiating from the twisted bowel,
which is often evident at the point of obstruction. Sigmoid volvulus can be differentiated from a cecal volvulus by its ahaustral wall.
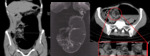
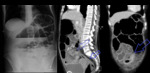
- Sigmoid volvulus (Fig.
5,
Fig.
6)
- The inverted U sign,
an inverted ahaustral dilated sigmoid in the shape of an inverted “U” extending into the right upper quadrant,
is specific to sigmoid volvulus.
- Northern exposure sign describes repositioning of the dilated sigmoid colon above the transverse colon – it is the most specific sign.
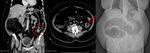
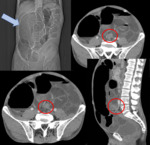
2. Cecal volvulus (Fig.
4,
Fig.
7)
- Torsion or hyperflexion of an enlarged,
poorly fixed,
and hypermobile cecum
- The cecum rotates out of the right lower quadrant into the left upper quadrant and occasionally into the left lower abdomen or mid line.
- Coronal reformations confirm the abnormal location of the cecum.
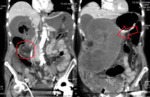
In acute diverticulitis patients,
LBO usually occurs in the setting of multiple episodes that causes narrowing and stricture formation. (Fig.
8)
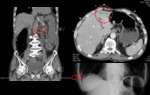
- CT scans,
are characterized by segmental,
symmetric bowel wall thickening with hyperemia,
which is typically in a longer segment (>10 cm) than malignant lesions.
- Pericolonic inflammation and fat stranding are hallmarks of diverticulitis.
Fluid in the root of the mesentery and vascular engorgement also favours the diagnosis of diverticulitis.
We should accept that in some patients it is not possible to distinguish between diverticulitis and a colonic malignancy without a colonoscopy guided biopsy. (Fig.
9)
Intraluminal content,
in most cases fecal impactation,
is not an unusual cause of LBO in the elderly,
chronically debilitated patients,
and in those taking certain medications.
(Fig.
10)
Uncommon causes (Fig.
11)
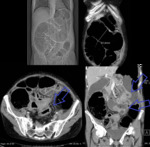
- Intussusception - The most common cause of a colocolonic intussusception is a primary colon carcinoma.
- Hernia - The most common internal hernia to produce an LBO is the foramen of Winslow hernia.
(Fig.
12)
- Inflammatory bowel disease - Crohn disease will have colonic involvement in 20% to 50% of patients and stricture formations in 5% to 17%.
(Fig.
13,
Fig.
14)
Pseudo-obstruction
- Ogilvie syndrome is described as an acute dilatation of the colon due to altered autonomic innervation of the colon with preserved haustration,
being perforation a possible complication.
(Fig.
15)
- Toxic megacolon is characterized by its hallmark feature of marked bowel wall thickening,
loss of haustration,
and segmental parietal wall thinning.
Complications
As dilatation of the colon increases,
the risk of perforation also augmented.
Perforation may occur at the site of obstruction,
or more proximally,
secondary to ischemic change. Intestinal ischemia and infarction are the major causes of morbidity and mortality in patients with bowel obstruction.
The exact size of the cecum at risk for perforation ranges in the literature from 9 to 12 cm,
but it is important to attend that the exact size of the cecum is less important than the duration and speed of is distension. Obstruction to venous outflow is the most common cause of ischemia in bowel obstruction.
CT features of complications includes abnormal decreased bowel wall enhancement, pneumatosis,
portal venous gas,
and pneumoperitoneum.
(Fig.
16,
Fig.
17)