Specific diagnosis of acute biliary disease is not always possible clinically because of the overlapping signs and symptoms,
such as right upper quadrant and epigastric pain,
jaundice,
and high fever.[2] Thus,
imaging plays a key role in establishing a prompt diagnosis and guiding the appropriate treatment.
Ultrasonography (US) should be the first imaging modality performed in patients with suspected biliary disease.
It has the advantages of being readily available and rapidly performed,
involving no ionizing radiation,
being able to confirm the presence of gallstones and detect complications of cholecystitis or biliary dilatation,
and being able to provide an alternative diagnosis.
Diagnostic US usually obviates the need for further imaging unless there are atypical signs or complications are suspected.[1]
Both computed tomography (CT) and magnetic resonance (MR) imaging allow detailed evaluation of the biliary system.
CT is often chosen because of its widespread availability,
faster imaging speed,
decreased artifacts,
and increased anatomic coverage during a single breath hold.[2] CT is also the best technique for direct imaging of emphysematous cholecystitis,
gallstone ileus,
and confirmation of suspected gallbladder perforation.[5] Multisequence MR imaging including MR cholangiopancreatography (MRCP) are employed in the acute or subacute setting as a non-invasive method (in alternative to endoscopic cholangiopancreatography) in the detection of the cause of common bile duct obstruction (previously unclarified by US and/or CT) and in the evaluation of complications that arise from acute cholecystitis and acute suppurative cholangitis.[3]
ACUTE CHOLECYSTITIS
The imaging findings include:
At US they may appear as mobile echogenic foci casting posterior acoustic shadows.
Sometimes a wall-echo-shadow sign is observed if the gallbladder is filled with gallstones.
A stone impacted in the gallbladder neck or cystic duct increases the specificity of the examination.[5]
Gallstones are depicted as a round signal defect in MRCP and heavily T2-weighted images.
A stone with high cholesterol content (or pigmented stone) may appear hyperintense on T1-weighted images.[3]
- Gallbladder distention (>40 mm)
- Intraluminal sludge
- Gallbladder wall thickening (>3 mm)
Gallbladder wall thickening is a common appearance but not characteristic of acute cholecystitis,
since it is possible to observe this finding in various conditions,
such as hypoalbuminemia,
heart failure,
hepatitis,
etc.[4]
- Gallbladder wall edema and mural stratification
- Pericholecystic inflammatory fat stranding/fluid and subserosal edema
Presence of pericholecystic inflammatory change is thought to be the most specific CT finding.[1]
- Pericholecystic fluid
- Perihepatic fluid
Some of these features are depicted on figure 2.
One of the most important advantages of US over other imaging techniques in the investigation of acute cholecystitis is the ability to assess for a sonographic Murphy sign,
which,
together with the presence of gallstones,
is the most specific US finding of acute cholecystitis.[1]
At CT or MR imaging,
transient increase in pericholecystic hepatic parenchymal enhancement (figure 2B) may be seen in the arterial phase,
caused by reactive hepatic arterial hyperaemia.
Also,
increased gallbladder wall enhancement and increased transient pericholecystic hepatic enhancement have been shown to have the highest sensitivity and specificity for the diagnosis of acute cholecystitis and differentiation from chronic cholecystitis.[1]
ACALCULOUS CHOLECYSTITIS
US remains the initial imaging modality of choice.
Eliciting a positive sonographic Murphy sign can help distinguish acute acalculous cholecystitis from a distended gallbladder caused by prolonged fasting,
although this sign may not be possible to evaluate,
for instance in the sedated intensive care unit patient.[5]
The CT and MR imaging findings are similar to those of calculous cholecystitis.
The advantage of these modalities is that they may show pericholecystic inflammatory change and fluid and abnormalities of the gallbladder wall or adjacent hepatic parenchyma,
which may not be conspicuous at US.
A normal gallbladder at CT is useful to exclude the diagnosis.[1]
Percutaneous cholecystostomy can be useful for both diagnosis and treatment in patients with sepsis of unknown cause and equivocal imaging findings of acute acalculous cholecystitis and treatment when the surgical approach is contra-indicated.[1]
EMPYEMA
Pus within the gallbladder may resemble sludge at US,
CT and MR imaging,
with material echogenic,
hyperattenuating and low signal,
respectively,
in the dependent portion of the gallbladder.
The accompanying imaging findings of acute cholecystitis are helpful in the diagnosis.[3]
GANGRENOUS CHOLECYSTITIS
US is not very sensible or specific for the detection of this complication.
A sonographic Murphy sign may not be present in these patients because of associated denervation of the gallbladder wall.
Also,
findings such as intraluminal membranes resulting from desquamation of the gallbladder mucosa may be difficult to assess on US.[1,4]
The imaging features of gangrenous cholecystitis include (figures 3 and 4):
- Gas within the gallbladder wall or lumen (in the context of emphysematous cholecystitis)
- Intraluminal membranes
- Greater degree of gallbladder distension
- Heterogeneous striated thickening and irregularity or disruption of the gallbladder wall (in the context of perforation)
- Irregular or absent gallbladder wall enhancement after intravenous contrast
- Intramural abscess
- Pericholecystic fluid collection or abscess
HEMORRHAGIC CHOLECYSTITIS
In addition to typical findings of cholecystitis,
there is intraluminal hemorrhage.
At US,
blood in the gallbladder lumen can be recognized as hyperechoic or heterogeneous material that is generally more hyperechoic than biliary sludge.
Clotted blood may appear as a clump or mass adherent to the gallbladder wall or heterogeneous echogenic material,
simulating a mass if organized (figure 5A).
CT shows spontaneous hyperattenuating material inside the gallbladde (figure 5B).[1] MRI may be more specific than both US and CT.
Hemorrhage in the wall and lumen of the gallbladder is seen as high signal intensity of methemoglobin on T1-weighted images.
Blood clots and hemorrhage may be shown as defects or low signal intensity lesions on T2-weighted images.
A fluid-fluid level can be observed in the lumen of the gallbladder and extrahepatic bile ducts.[3,5]
EMPHYSEMATOUS CHOLECYSTITIS
The hallmark of emphysematous cholecystitis is the presence of gas within the gallbladder wall or nondependent portion of the lumen (figures 6 and 7).[3]
At US,
a small amount of gas in the gallbladder wall may appear as an echogenic focus with associated ring-down or comet-tail artifact.
Larger amounts of intramural gas and intraluminal gas appear as a curvilinear arc of increased echogenicity with associated so-called dirty posterior acoustic shadowing that obscures the gallbladder fossa (figure 6A),
making it difficult to differentiate emphysematous cholecystitis from a contracted gallbladder with stones or a porcelain gallbladder with calcified wall.[1]
CT is the most sensitive and specific imaging modality for detection of gas and diagnosis of emphysematous cholecystitis.
At MR imaging,
gas in the gallbladder lumen and wall appears as signal void areas.[5] Other nonspecific CT and MRI findings resemble those of gangrenous cholecystitis and include irregularity or discontinuity of the gallbladder wall,
pericholecystic fluid and abscess formation.
Free intraperitoneal gas indicates associated gallbladder perforation and constitutes a surgical emergency.[1]
GALLBLADDER PERFORATION
The imaging findings of gallbladder perforation (figures 3 and 8) are:
- Interruption of the gallbladder wall or focal mural defect
- Extraluminal gallstone
- Gallbladder collapse
- Large amount of pericholecystic fluid
- Abscess formation in the liver,
gallbladder fossa,
or peritoneum
- Free intraperitoneal fluid and gas
Fluid often represents bile and,
in association with a collapsed gallbladder,
is indicative of free gallbladder perforation.[2]
CT is more sensitive than US for the detection of perforation.[5] Because of its superior soft tissue resolution and multiplanar imaging capability,
MR may also be a useful adjunct if US and CT findings remain equivocal.[1]
GALLSTONE ILEUS and CHOLECYSTOENTERIC FISTULA
CT is arguably the best method for imaging gallstone ileus (figure 9).
It is helpful in determining the multiplicity and location of ectopic gallstones and in detecting them before an obstruction develops.[5]
The imaging features include:
- Pneumobilia,
ectopic gallstone and bowel obstruction – the Rigler triad[5]
- Gallbladder collapse or contracted gallbladder containing air
- Fistulous connection between the gallbladder and the duodenum,
small bowel,
or colon (figure 10)
BILIARY COLIC
US is the technique of choice for detection of bile duct obstruction in emergency patients.
Its main application is the detection of bile duct dilatation.[1] Stones within the biliary tract may be readily detected with MRCP,
and less accurately with US and CT.
US limited sensitivity results in part from inability to completely visualize the common bile duct,
particularly the distal duct,
because of interposed bowel gas.
Common bile duct stones appear as echogenic foci,
which may or may not cause posterior acoustic shadowing depending on size and composition.[1]
As with gallstones,
the CT appearance of common bile duct stones is variable,
depending on their size and composition.
When visible on CT images,
a biliary stone often appears angulated and geometric and is located dependently in the duct,
with a rim of bile seen along the stone’s anterior margin (figure 11A).[2]
MRCP has high accuracy in the detection of common bile duct stones.
Stones generally appear as well circumscribed low-signal-intensity filling defects in the biliary tract (figure 11B and 11C).[1]
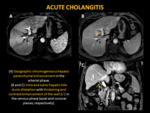
ACUTE CHOLANGITIS
The imaging findings of acute cholangitis (figure 12) include:
- Bile duct dilatation
- Biliary obstruction
- Diffuse and concentric thickening of the bile duct wall
After contrast administration,
CT findings include:
- Increased enhancement of the bile duct wall
- Nodular,
patchy,
wedge-shaped,
or geographic inhomogeneous hepatic parenchymal enhancement in arterial phase (figure 12A)[1]
At MR imaging,
in addition to the findings similiar to CT,
other feature of acute cholangitis is periportal edema depicted as areas of high signal intensity along the intrahepatic and extrahepatic portal vein and biliary tree on T2-weighted images.[1]
Imaging findings indicative of ACUTE SUPPURATIVE CHOLANGITIS are intraductal purulent material with low signal intensity on T2-weighted images and/or intermediate signal intensity on fat-suppressed T1-weighted images.
Purulent bile may have increased CT attenuation.[3]
Complications of acute cholangitis include pyogenic liver abscess,
portal vein thrombosis from pylephlebitis,
and biliary peritonitis.[1]