Type:
Educational Exhibit
Keywords:
Transplantation, Stents, Angioplasty, Ultrasound-Colour Doppler, Fluoroscopy, CT, Vascular, Biliary Tract / Gallbladder, Liver
Authors:
F. P. Tarantino, P. Rossi, R. Cioni, D. Caramella, L. Crocetti; Pisa/IT
DOI:
10.26044/ecr2019/C-2778
Background
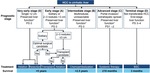
EASL 2018 guidelines confirm LT as a first line treatment in patients with early HCC unsuitable for surgery and life-saving treatment in patients with end-stage liver disease [Fig.1].
Even though patient selection,
surgical technique,
organ preservation and immunosuppressive agents advancement significantly improved with 5-year graft and patient survival rates of 67% and 74%,
respectively,
radiologists’ role remains of the utmost importance to early detect and treat transplant complications avoiding graft loss.
After discharge,
one month after transplant,
ultrasound (US) is performed as a first line diagnostic exam to study graft parenchyma and confirm the transplant success evaluating biliary and vascular (arterial and venous) anastomoses.
Duplex US must be performed carefully using the correct parameters (PRF and wave angle) to produce reliable and reproducible spectra and velocity measurements.
CT exam is the second line diagnostic exam,
confirming vascular or parenchymal US abnormal findings,
both in the early and late post-LT period.
MR cholangiography has a fundamental role evaluating biliary complications.
Angiography and percutaneous cholangiography procedures,
providing a panoramic and detailed representation of vascular and hepatic biliary tree,
have a crucial role in the treatment of complications.