RAS refers to a narrowing of one or both renal arteries leading to impaired blood flow to the kidneys and represents the most common cause of reno-vascular hypertension,
accounting for 1-10% of the 50 million cases of hypertension in the US in 2018 with prevalence of unilateral stenosis (compared to bilateral stenosis) approximately from 50 % to 80% [1-3].
RAS etiopathogenesis is heterogeneous and the two most common causes are represented by atherosclerosis (60-90%) and fibro-muscular dysplasia (10-30%).
Atherosclerosis primarily affects males over the age of 45 years old,
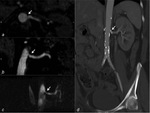
mainly involving the ostium or the proximal 2 cm of the main renal artery (fig.1).
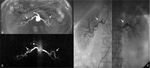
Fibro-muscular dysplasia primarily affects women younger than 50 years old and usually involves the middle and distal main renal arteries or intra-renal branches (fig.2).
Other less common etiologies (<10%) include thromboembolic disease,
arterial dissection,
vasculitis,
neurofibromatosis type 1 and retroperitoneal fibrosis.
Duplex US represents the first line diagnostic exam,
with significant limits: it is operator dependent and has various grade of sensibility: a complete examination of both renal arteries may be achieved in 50-90% of cases.
Second line exams include CT angiography (CTA) and contrast-enhanced MR (CEMRA); both having high sensibility in evaluating the morphology of the renal arteries,
although,
they lack information about the haemo-dynamic function with risk of overestimation/underestimation of a stenosis,
in particular,
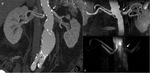
in patients with atherosclerosis (fig.3).
In addition to CT radiation exposure,
both techniques use contrast medium,
a contraindication in patients with pre-existing chronic kidney disease and high blood creatinine level,
frequently occurring in these patients.
ACE inhibitor scintigraphy evaluates the kidney function,
without morphological arterial information.
Once the gold standard in RAS diagnosis,
conventional arteriography maintains nowadays a pivotal role in the disease treatment,
with the possibility of balloon angioplasty and stent placement.
Since the development of higher field (3T) MR scanner,
optimized angiographic sequences may help the diagnostic process,
avoiding radiation and contrast agents administration.