Ultrasound (US) is operator dependent,
breast ultrasound even more so.
Careful attention to scanning technique as well as knowledge of different technical options available are imperative for an optimized and accurate breast US examination.
US must be interactive,
dynamic modality and individualized technique.
Positioning.
First of all,
correct patient position is essential,
with the patient´s arm relaxed and flexed behind the head.
Supine position is selected to study medial or inferior lesions.
To study superior lesions the patient is in supine or sitting and opposite posterior oblique position is used in lateral breast lesions and axilla (Fig1).
It is important to correlate the ultrasound with any palpable lumps indicated by the patient.
If the patient can only identify the lump when she is erect,
then we should rescan the patient in the erect position.
Transducer.
Breast ultrasound requires a linear high-frequency transducer 8-15 MHz.
But we must personalize the frequency according to breast characteristics,
using a lower frequency transducer (5-12 MHz) in larger attenuative breasts,
inflammatory masses and the axilla (Fig.2).
In small breast or superficial lesions,
higher frequency transducers (8-17 MHz) must be selected (Fig.3).
High-frequency transducers provide super spatial and soft tissue resolution,
improving differentiation of subtle shades of gray and margin resolution.
Nevertheless,
the cost of such a high insonating frequency is reduced penetration due to attenuation of the ultrasound beam,
making visualization of deep posterior structures difficult.
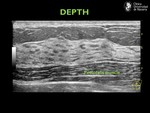
Depth.
The depth must be set so that the pectoralis muscles are visualized along the posterior margin of the field of view (Fig.4).
When a lesion is identified,
or while looking for a subtle finding,
the depth may be adjusted,
centering the lesion/area of interest.
It should be decreased to study superficial lesions and increased to better visualization of deeper structures.
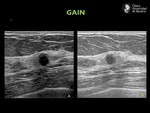
Gain.
The gain should be adjusted so that fat at all levels is shown as a midlevel gray.
(Fig.5)
Premammary layer is the reference tissue.
It contains fat,
thus,
it must have the same level of gray as retromammary layer.
Time gain compensation (adjusts image brightness at different depths to compensate for attenuation of the ultrasound beam as it penetrates into the breast tissue),
can be adjusted automatically if the equipment does not have this option,
should be set manually.
Focal zone
The focal zone is the region over which the effective width of the sound beam is within some measure of its width at the local distance.
It is indicated by moving small arrowhead or hourglass at the side of the screen (Fig.
6).
Single focal zone must be kept either at the lesion or just deep to it.
Be careful because if it is too deep causes volume-averaging artifacts and gives erroneous results about tissue consistency.
Multiple focal zones improve resolution at multiple depths simultaneously; should be used if available.
Speed of sound imaging.
Conventional US systems set the speed of sound in tissue at a uniform 1540 m/sec.
Nevertheless,
the speed of sound in tissues of different composition is variable,
depending on whether predominately fatty,
dense or mixed tissue.
In fat,
speed of sound is about 1430-1470 m/sec.
It is higher in dense tissue.
It can be used to better characterize lesion margins,
microcalcifications and to identify subtle hypoechoic lesions surrounded by fatty tissue (Fig.7).
Speckle reduction and spatial compounding.
Spatial compounding acquires multiple images obtained from different angles within the plane of imaging,
therefore artifactual echoes are substantially reduced.
Ultrasound images show a characteristic granular structure,
known as speckle.
Speckle reduction is a real-time post-processing technique that also increases contrast resolution and improves border definition.
It is complementary to spatial compounding and can be used simultaneously (Fig.8).
Tissue harmonic imaging.
It uses the effect of nonlinear propagation of the acoustic signal and generation of the higher-frequency signals in the insonated tissue.
When a lesion is localized,
we can use harmonic imaging to get better signal-noise ratio,
reduce side lobe artifacts,
and improve lateral resolution compared with fundamental frequency sonography.
Harmonic imaging also improves contrast between fatty tissue and subtle lesions and it´s very useful to better characterize a cyst or a subtle solid lesion.
(Fig.9,
Fig.10)
Imaging panoramic view.
By using a freehand technique,
the operator slides the transducer along the desired region of interest (Fig.11).
This can be helpful in large lesions and for assessing the relationship of multifocal-multicentric disease.
Virtual convex,
also allows larger areas to be collated into a single image (Fig.12),
we can use this method thoroughly entire the study.
Doppler.
Several studies have demonstrated the similarity of Doppler characteristics in benign and malignant lesions and seem that Doppler does not improve specificity.
But it is very useful to evaluate cysts and complex cystic masses that contain a solid component.
Power Doppler is generally more sensitive than color Doppler detecting malignant breast lesions.
(Fig.13).
We can use doppler to evaluate “twinkle artifact” to identify biopsy marker clip or subtle echogenic microcalcifications.
B-flow imaging mode
The B-Flow imaging technique shows the blood flow signals in gray scale imaging throughout the entire field of view.
The displayed flow intensity is not affected by the interrogation angle of the ultrasound beam as it is with Color Doppler (Fig.14).
Furthermore,
B-Flow is capable of displaying true flow hemodynamics with spatial resolution similar to that of gray scale imaging and doesn’t suffer from blooming or wall overwriting.
We are currently studying its application to complex cystic masses and suspicious breast masses.
Shear wave elastography (SWE).
SWE serves as an accurate diagnostic technology for discriminating between malignant and benign breast lesions.
SWE uses the acoustic radiation force induced by the ultrasound push pulse generated by the transducer.
It provides quantitative elasticity parameters (kPa or m/s),
as well as displaying a visual color overlay of elastic information in real time.
SWE is a highly reproducible technology and may be useful in improving the specificity of US evaluation of BI-RADS 3 and 4A lesions.
Malignant masses evaluated with elastography tend to be more irregular,
heterogeneous,
and typically appear larger at elastography than at grayscale imaging.
Although malignant lesions generally also exhibit maximum stiffness greater than 80-100 kPa (orange-red color),
caution is necessary when it is greater than 30kPa.
(Figs.
15,
16,
17).