Imaging workup
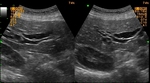
- Abdominal ultrasonography
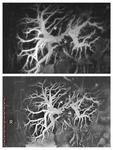
It can be used as initial modality.
Biliary dilatation is easily detected,
while intraductal lesions,
small tumor masses and wall thickeninig is more difficult to detect and usually are discovered in more advanced cases.
Propper assessment of tumor spread and respectability is also relatively unreliable.
The accuracy of US depends also on the equipment quality and operator’s experience (fig.2) /7,8/.
The technique is widely available,
noninvasive,
quick and relatively easy to perform.
It can depict the level and cause of biliary obstruction,
in most of the cases the tumor mass as well,
and it can help in staging the disease.
The acquisition of optimal images includes: oral water (or contrast) 700-1000 ml.
30 minutes before examination,
i.v.
contrast 120 ml.,
bolus-triggered,
injection rate 3-4 ml/sec.
Collimation 0.5-0.75,
pitch 1-1.5; slice thick – ness 2.5-5 mm.
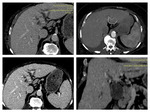
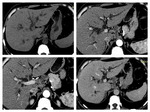
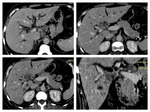
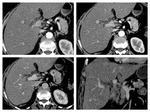
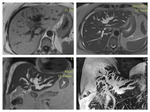
We acquire late arterial phase (instead of arterial phase) 35 seconds; portal-venous phases (60-65 seconds) and in some cases delayed phase (3-5 minutes).
We generate CTA images and study the vascular map to depict infiltration of important vessels and the presence of any vascular variants,
thereby helping in the surgical planning (fig.3,4,5) /9/.
We use standad liver protocol,
including routine gadolinium – enhanced dynamic series at 1.5 T,
standart MRCP sequences with maximum intensity projections.
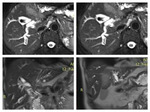
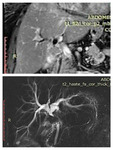
Perihilar cholangiocarcinomas present with dilated bile ducts and lack of communication between the right and the left hepatic ducts.
Very often in periductal infiltrating tumors it is possible only to find a stricture and thickening of the walls of the bile ducts with low or medium enhancement in the dynamic postcontrast scan /10/.
Diffusion – weighted imaging may improve the detection of tumor extent along the bile duct and liver invasion.
MR imaging with MR cholangiography has been found to be superior to CT for the assessment of intraductal lesions /5/.
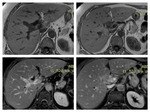
Perihilar cholangiocarcinoma is usually hypo- to isointense on T1 weighted images, and on T2 mainly slightly hyperintense.
At dynamic imaging with gadolinium based contrast material it usually shows slight heterogeneous enhancement that increases on delayed phase images (fig.6,7,8,9,10) /11/.
ERCP may be necessary in obtaining tussue samples for confirmation of diagnosis.
Endoscopic US with fine-needle aspiration.
Positron Emission Tomography and Positron Emission Tomography/CT.
They are extremely valuable in detecting very small infiltrating stricture forming tumors,
recurrent tumors,
metastatic lesions in the lymph nodes or peritoneum,
where CT and MRI have some limitations.
Primary sclerosing cholangitis; Recurrent pyogenic cholangitis; Mirizzi syndrome; Gall bladder cancer; Inflammatory pseudotumor; Lymphoma; Melanoma deposits; Sarcoidosis; Carcinoid tumor; Metastasis.
-
Key points in the radiological report:
1. Exact location and type of the tumor according to Bismuth-Corlette classification.
2. Type of tumor grouth
3. Size of tumor
4. Local spread and infiltration of surrounding structures – bile ducts,
liver,
vessels.
5. Lymph nodes involvement – regional or distant
6. Distant metastasis