Abdominal X-ray and ultrasound can be useful to suspect AMI within the correct clinical context,
but the absence of abnormal findings does not exclude the diagnosis.
Typical X-ray findings include bowel dilatation,
portomesenteric gas,
pneumatosis intestinalis and pneumoperitoneum,
whereas ultrasound findings include parietal thickening of a long segment of intestine with diminished or absent Doppler flow.
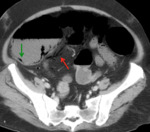
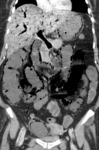
Multiphase CT of the abdomen and pelvis is the imaging modality of choice in the assessment of patients with suspected AMI.
An arterial phase is done triggered automatically by a real-time bolus tracking technique with the ROI in the origin of the abdominal aorta when the aorta reaches >100 HU.
The portal venous phase is done 30 seconds after the arterial phase finishes.
A phase without contrast and the use of oral contrast are optional.
Typical findings in the CT for the diagnosis of AMI are bowel dilatation,
abnormal bowel wall enhancement,
thickening or thinning of the bowel wall,
intramural bowel gas (pneumatosis intestinalis),
gas in the mesenteric vein or in the portal vein (pneumatosis portalis),
ascites and mesenteric edema.
The perforation of the wall may cause pneumoperitoneum.
In some cases,
the cause can be identified and the occlusion of the mesenteric vessels or the portal vein can be seen.
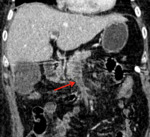
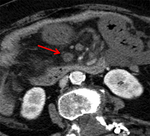
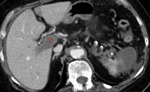
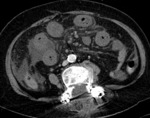
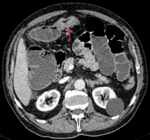
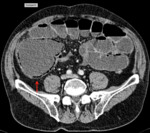
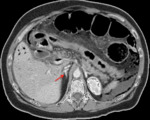
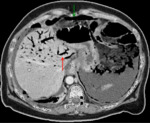
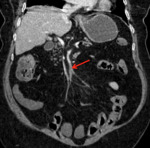
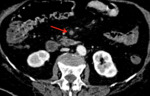
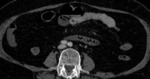
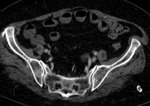
Examples of patients with acute mesentic ischemia due to different causes:
CASE 1: Venous thrombosis. 69-year-old woman with abdominal pain during 3 weeks,
which got worse in the last 5 days accompanied with diarrhea and leukocytosis.
(Fig.
1,
2,
3 and 4)
CASE 2: Bowel obstruction and dilatation secondary to colon cancer. 73-year-old with abdominal pain and distension for the last 2 days accompanied with nausea and vomiting.
Slight leukocytosis with neutrophilia and increased CRP and lactate levels.
(Fig.
5 and 6)
CASE 3: Hypovolemic shock. 80-year-old patient with systemic shock and abdominal pain.
(Fig.
7 and 8)
CASE 4: Arterial thrombosis. 81-year-old man with a history of a cardioembolic stroke who presents abdominal pain,
leukocytosis,
increased levels of CRP and alkaline phosphatase after an episode of atrial fibrillation.
(Fig.
9,
10,
11 and 12)
CASE 5: Arterial vasoconstriction due to drugs (noradrenaline). 48-year-old woman admitted to the hospital with respiratory insufficiency and fever of 40º.
After a neuroleptic syndrome she is relocated to the Intensive Care Unit in a state of coma.
A blood test shows leukocytosis and increased levels of LDH and alkaline phosphatase.
(Fig.
13 and 14)