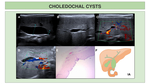
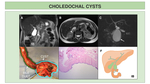
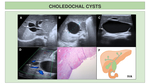
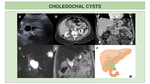
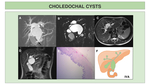
We present illustrations of the classification of choledochal cysts,
together with the most representative findings in US,
CT and MRCP.
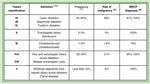
The classification proposed by Todani is the most used for its categorization,
dividing them into five groups (Fig. 1).
Type I is the most frequent,
representing 50 to 85%,
subdivided into 3 categories.
Type IA is a cystic dilatation of the entire extrahepatic biliary tree,
with preservation of the intrahepatic ducts (Fig. 2). Type IB is a focal or segmental dilatation of the extrahepatic bile duct,
being more frequent distally,
without alteration in pancreaticobiliary junction (Fig. 3). Type IC is defined as a fusiform,
diffuse or cylindrical dilatation of the entire extrahepatic bile duct generally associated with an anomaly in pancreaticobiliary junction (Fig. 4) [3-7].
Type II represents 2% of the cases and is defined as a true diverticula of the extrahepatic bile duct,
usually arising laterally but less frequently in the pancreatic portion.
Type III represent 1.4-4.5%,
is also called choledochocele,
consists of distal dilatation of common bile duct that borders duodenal wall,
often protruding over it.
The outer lining is always duodenal mucosa,
while the internal lining may be duodenal or biliary epithelium.
Type IV is second in frequency and represent 15-35%.
These are multiple and involve the extrahepatic and intrahepatic bile duct dividing into two subtypes.
Type IVA cysts are multiple dilatations of the extrahepatic and intrahepatic bile ducts,
being intrahepatic cystic or fusiform type (Fig. 5). Type IVB cysts refer to multiple dilatations of the extrahepatic bile duct.
Finally,
Type V, also known as Caroli disease,
represents 20% and is defined as multiple dilatations of the intrahepatic bile ducts (Fig. 6) [3-7].
Ultrasound is the first imaging study that is usually done.
With the exception of type III and V cysts,
the most common finding is a cystic mass located in the right upper quadrant,
adjacent to the porta hepatis,
which is separated from the gallbladder.
To obtain a diagnosis of certainty,
a continuity must be visualized between the cystic dilatation and the bile duct (Fig. 7). This finding differentiates this pathology from other diagnoses such as the pancreatic pseudocyst,
echinococcal cyst and biliary cystadenoma.
For this reason,
and the limitations of ultrasound,
another study must be done to confirm this finding [8].
Computed tomography has the advantage that it allows to visualize with greater certainty the continuity between cyst and bile duct,
the relationship with surrounding structures and the presence of malignancy (Fig. 8). Additionally it is superior to ultrasound in imaging the intrahepatic bile ducts,
distal bile duct and pancreatic head [8].
Magnetic resonance cholangiopancreatography (MRCP) has a diagnostic certainty for the detection of this pathology ranging from 96 to 100% which varies between the different types of the Todani classification (Table 1). In the detection of anomalous pancreaticobiliary junction,
the diagnostic sensitivity is 53-100% and the specificity is 90-100% (Fig. 9),
similar to endoscopic retrograde cholangiopancreatography (ERCP) [9].
MRCP uses T2 weighted sequences with fat suppression which allows visualization of spaces filled with liquid,
being of great use in the diagnosis of types I,
II and III,
however in type IV and V it can be difficult to demonstrate the relationship of liquid collections with biliary tree (Fig. 10).
In these cases,
the use of intravenous contrasts,
such as gadoxetic acid,
drastically improves diagnosis of these types,
by performing T1-weighted sequences in hepatobiliary phase,
which begins approximately 20 minutes after the administration of intravenous contrast,
with a better visualization at 60 minutes,
enough time for contrast to be excreted to bile ducts,
improving visualization of dilated sites,
communication of dilatations with bile duct and additionally detection of anomalous pancreaticobiliary junction (Fig. 11) [5-10].