Cornea: it is the frontal continuation of the sclera and covers the anterior chamber,
the iris and the pupil.
It is formed by surface mesenchyme.
It refracts the light and is responsible for 2/3 of the power of the eye but its focus is fixed.
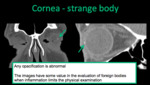
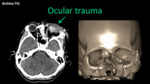
- Strange body: any opacification of the cornea is abnormal.
The images (CT) have some value in the evaluation of foreign bodies when inflammation limits the physical examination.
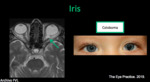
Iris: It´s a circular diaphragm,
contractile and pigmented with a central hole (pupil) that regulates the passage of light in to the eye.
It is the anterior region of the vascular tunic of the eye (choroid - ciliary body - iris).
Its periphery is attached to the ciliary body and it separate the anterior from the posterior chamber.
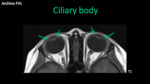
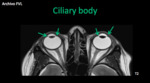
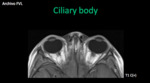
Ciliary body: It´s a wedge-shaped,
annular structure with ciliary muscles that help lens accommodation (focus) - III PC. It is attached anterior to the iris and posterior to the lens (zonula).
It is formed by retinal neuroectoderm and mesenchyme of the pupillary membrane and it produces aqueous humor.
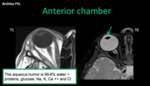
Anterior chamber: It is a small crescent-shaped cavity,
anterior to the lenses with an approximate diameter of 3mm AP.
It contains aqueous humor - 0.2 ml (produced by ciliary body).
It is formed by a mesenchyme cleft between the surface ectoderm and the Iris.
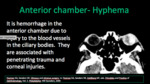
- Hyphema: it is hemorrhage in the anterior chamber (injury of the blood vessels of the ciliary bodies).
They are associated with penetrating trauma and corneal injuries.
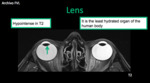
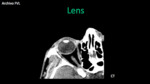
Lens: It´s a biconvex structure consisting of multiple fibers and proteins that form a liquid crystal (chemically: 66% of water and 34% proteins).
It is the least hydrated organ of the human body (Hypointense in T2).
It is deformed with the contraction of ciliary muscles and focus objects.
It is formed by surface ectoderm.
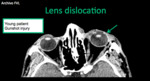
- Lens dislocation: penetrating trauma (direct injury) or closed trauma (increased intraocular pressure and injures of the suspensory ligaments). Contralateral comparison helps to find any irregularity in position that suggests zonule injury. It is associated with fracture of orbit.
- Cataracts: it is the first cause of blindness in the world (30 million people blind in the world - 50% cataracts).
Acquired - most cases (age,
trauma,
infection).
Congenital - TORCH (especially rubella).
The pathogenesis is not well understood.
The lenses are an epithelium that does not replace their non-viable cells (prone to degeneration with age).
Risk factors: age,
smoking,
alcohol,
exposure to light,
low educational level,
DM and steroids.
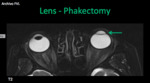
- Phakectomy: it´s the surgical removal of the lens through an incision in the sclera or phacoemulsification and suction.
Insertion of new lens - intraocular implant (hypointense thin lines).
Vitreous: the vitreous body occupies the space between the lenses (hyaloid fossa) and the retina.
It is 2/3 of the volume of the eye and contains the vitreous humor (4 ml).
It transmits the light,
supports the lenses and helps support the sensory retina against the pigmented epithelium of the retina.
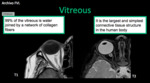
The vitreous is water (99%) joined by a network of collagen fibers.
It is the largest and simplest connective tissue structure in the human body.
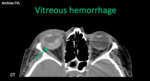
- Vitreous hemorrhage: secondary to trauma - pain is often due to another concomitant injury.
Spontaneous in anticoagulated patients or with SAH (decreased vision without pain).
Most of it have spontaneous resolution.
It is a suggestive sign of child abuse (shaken baby syndrome).
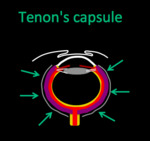
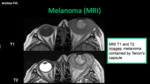
Tenon's capsule (Fascia bulbi): it covers the eye and separates it from adjacent fat.
It attaches in to the sclera and continues with the sheath of the optic nerve (episcleral or Tenon's space).
It has an strong union with eye muscles (that's why they do not retract after a tenotomy).
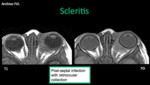
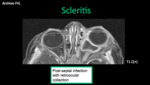
The Tenon´s capsule can be distended in a semicircular shape by transudate / exudate.
Processes that affect the capsule: inflammatory and neoplastic (scleritis,
Tenon's fasciitis,
pseudotumor,
retinoblastoma and melanoma).
Sclera (external layer): elastic collagen fibers that wraps the eye.
In its anterior region it continues with the cornea and posterior with the optic nerve sheath.
- Scleritis: clinically presents with pain and photophobia (unilateral 66%).
There are many causes: infectious (bacteria,
viruses and fungi),
autoimmune disease (AR,
polyarthritis nodosa,
SLE and Crohn),
metabolic disorders (gout),
trauma and other causes (sarcoidosis).
Choroid (middle layer): it is a vascular and pigmented tissue.
It provides vascular irrigation (pigmented retinal epithelium) and regulate the eye temperature.
In its anterior region it continues with the ciliary body and the iris (uveal tract).
Its posterior region is inserted where the ciliary vessels enter the globe (lateral to the optic disc).
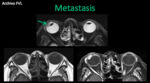
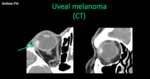
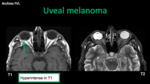
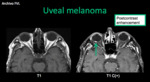
- Uveal melanoma: it is the most frecuent malignant intraocular tumor in adults (5.2 - 7.5 / 1'000,000 habitants).
The incidence increases with age (<2% in <20 years).
Clinically it presents in patients with 50 - 70 years old and unilateral eye discomfort.
It is 15 times more frequent in african american.
Location: choroid (85%),
ciliary body (9%) and iris (6%).
In MRI it presents as a soft tissue mass that bulges into the vitreous (Bruch's membrane),
hyperintense in T1 (melanin and hemorrhage).
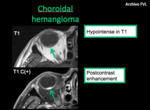
- Choroidal hemangioma: it is a benign vascular lesion that simulates other intraocular masses. In images its presents as a lenticular mass,
hypointense in T1 with intense enhancement after the administration of Gadolinium.
There are 2 classes: solitary (focal thickening usually in posterior region of the eye) and diffuse (choroid-ciliary body-iris),
associated with Sturge – Weber syndrome.
Retina (inner layer): it has two layer (inner neural and external pigmented).
The neuronal layer in its anterior region is attached to the ora serrata and posterior it is continued with the optic nerve.
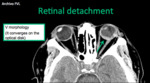
- Retinal detachment: it is the separation of sensory and pigmented retina.
The retinal pigment epithelium injury creates a leak that accumulated fluid in sub-retinal space.
Causes: retraction due to neoplastic lesion (choroidal melanoma),
vitreous proliferative disease,
DM,
trauma and infection.
Treatment: laser beam delivers energy to pigmented retinal epithelium and the resulting heat closes the lesion.
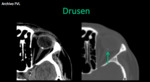
- Drusen: spherical,
acellular hyaline bodies with calcifications,
located on the optical disc (bilateral 73% of cases).
Clinically it is confused with papilledema.
Is it thought to be an accumulation of substances by axonal degeneration of the retina / optic nerve.
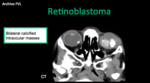
- Retinoblastoma: it is the most common tumor of the eye in pediatrics (1 / 15,000).
It has no predilection for gender or laterality (H: M and Right: Left).
Clinically it is presents in pediatric patients (<3 years old) with leukocoria,
strabismus,
visual disturbance,
pain or proptosis.
It is origin in retinal neuroectoderm cells.
It is associated with mutation in the Rb gene (chromosome 13).
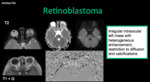
Sporadic (unilateral) or familiar (autosomal dominant- bilateral 85%).
1/3 of all retinoblastomas are bilateral. The patient have a high probability of other neoplasms (osteosarcoma).
Diagnostic Imaging: calcification (90%) + soft tissue mass T1 iso - hyperintense to the vitreous T2 hypointense with postcontrast enhancement.