Epidemiology
Although this disorder can affect anyone it is mostly seen in young and middle-aged adults.
The localized form affects most commonly the fingers and wrists of individuals between the ages 30 and 50 with a 2:1 female predominance.
The diffuse form is typically seen in the knees,
hips,
and ankles of individuals below the age of 40,
with only a slight female predominance.
Clinical presentation
The clinical presentation is relatively nonspecific and varies depending on the site and disease progression.
The progression of symptoms is usually slow,
although a torsion of a pedicular nodule can cause an acute onset of symptoms.
An extraarticular lesion often manifests as a painless swelling that may occasionally progress to erode the adjacent bone and cause pain.
The intraarticular form causes at first joint swelling with discomfort and as it progresses the increasing joint destruction is accompanied with a decreased range of motions,
increased pain and potentially locking of the joint.
Etiology and pathohistological findings
TSGCT were historically considered to be of non-tumoral reactive etiology.
Further research has discovered that a small proportion of cells within these lesions has a translocation causing overproduction of colony stimulating factor 1 (CFS 1).
These tumor cells recruit other CFS1 receptors bearing cells (monocytes,
giant cells,
foamy macrophages,
and osteoclasts).
The recruited cells are the ones that cause the inflammatory changes typical for these tumors.
Localized TSGCT usually measures up to 4 cm,
are well circumscribed and lobulated.
Diffuse type TSGCT are usually larger than 5 cm and the intraarticular forms have a recognizable villous pattern of growth,
whereas the extraarticular forms have a multinodular appearance.
Radiological findings
The distinction between a localized/diffuse and intraarticular/extraarticular form is made radiologically since the histological features are virtually the same in all lesions.
Although plain radiography,
ultrasound,
and computed tomography can give us certain information,
MRI presents the most comprehensive imaging method,
indispensable to diagnosis and treatment planning.
Plain radiographs can contribute to the diagnosis mostly in cases where there is damage or degeneration of the surrounding bones (erosions and cysts) and cartilage.
But occasionally also joint effusion or a soft tissue mass can be seen on a plain radiograph.
Similar findings as on radiographs can also bee seen on CT scans.
The lesions appear as hyperdense,
hemosiderin-laden masses.
Ultrasound can be helpful especially in characterizing extraarticular lesions.
Those appear predominantly as homogeneously hypoechoic formations through which the adjacent tendons move freely.
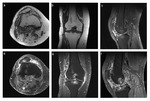
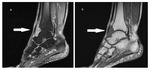
Hemosiderin accumulation accounts also for the MR appearance.
MRI images demonstrate low to intermediate signal intensity of lesions on both T1 and T2 weighted images with variable enhancement on T1 weighted postcontrast images. On gradient-echo images,
magnetic susceptibility artifacts with disproportionately lower signal intensity ("blooming") can be seen.
Treatment and prognosis
Local excision is the treatment of choice for localized TSGCT.
The recurrence rate is low and recurring lesions can be usually controlled with surgical reexcision.
Due to fairly common recurrences of the diffuse form of TSGCT,
which may severely compromise joint function, a wide excision is the treatment of choice.
Radiotherapy is the most commonly used adjuvant therapy in such cases,
but as new evidence emerge targeted therapies are also being increasingly utilized.