Although the majority of rectal tumors are histologically characterized as adenocarcinomas,
there is a wide spectrum of tumors and tumor-like conditions that may be found in the rectum and peri-rectal area.
We will divide these into neoplastic,
inflammatory,
traumatic,
vascular and congenital lesions as well as foreign bodies found in the rectum [1-5].
- Malignant neoplasms
- Primary rectal tumors
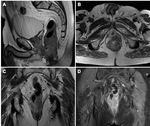
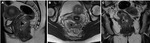
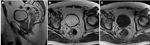
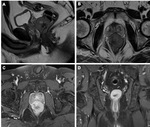
- Rectal adenocarcinoma (Fig. 1, Fig. 2 and Fig. 3)
The vast majority of rectal tumors are adenocarcinomas (98%).
These appear in many forms – as ulcerating lesions,
polypoid lesions protruding into the rectal lumen,
infiltrating lesions and stenosing lesions.
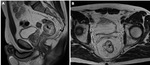
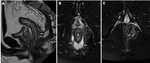
- Mucinous rectal adenocarcinoma (Fig. 4 and Fig. 5)
Mucinous adenocarcinomas are a subtype that can be identified on imaging due to the characteristic presence of mucin occupying > 50% of tumor.
This is seen on magnetic resonance (MR) as markedly high signal intensity (SI) on T2W images with corresponding low SI on T1W.
On computed tomography (CT) low attenuation is identified and some small calcification foci may be present.
- Neuroendocrine carcinoma of the rectum (Fig. 6)
This lesion is usually a small polyp or localized wall thickening,
that are more frequently found incidentally,
and have not specific features to help distinguish them from adenocarcinomas.
- Gastrointestinal stromal tumor of the rectum (Fig. 7)
GIST arises from the cells of Cajal and is the most common mesenchymal tumors of the gastrointestinal tract.
GIST is more frequently found in the stomach and small intestine.
GIST most likely presents as large,
well-circumscribed eccentric masses without invasion of adjacent organs and absent lymphadenopathy.
- B-cell Lymphoma of the rectum (Fig. 8)
Lymphomas of the rectum are rare and are more frequently of B-cell origin or of MALT-type.
Lymphomas have a variable appearance on imaging,
with the hallmark of absent obstruction despite the presence of a large mass,
which is distinctive from adenocarcinoma.
- Melanoma
Melanoma can be confidently diagnosed by imaging thanks to the identification of high SI on T1W images that remain high on fat suppressed images,
due to the presence of melanin.
Amelanocytic melanomas cannot be confidently diagnosed on imaging.
- Secondary tumors
Secondary involvement of the rectum by adjacent tumors or tumor recurrence in the pelvis can be identified on imaging with variable appearances.
- Prostate cancer invading the rectum (Fig. 9)
- Peri-rectal necrotic metastasis of lung cancer (Fig. 10)
- Rectal cancer recurrence in the pelvis with sacral invasion (Fig. 11)
- Benign neoplasms
- Tubulo-villous adenoma of the rectum (Fig. 12)
Adenomas are precursors to adenocarcinomas due to a step-wise malignant transformation.
This carcinomatous transformation is related to tumor size (more frequent in larger lesions) and histological type (more frequent in the villous adenoma).
- Leiomyoma of the rectum (Fig. 13)
Leiomyomas of the rectum are extremely rare mesenchymal tumors that present as intraluminal polypoid masses.
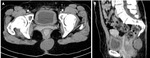
- Neurofibromas of the pelvis (Fig. 14)
Neurofibromas present on imaging as symmetric bilateral presacral masses with lobulated contour on T2W images,
along the location of the lumbosacral plexus (plexiform neurofibromas),
virtually diagnostic of type I neurofibromatosis.
Special attention should be given to the symmetry of these findings as marked asymmetry should raise the suspicion of malignant transformation.
- Ulcerative colitis (Fig. 15, Fig. 16 and Fig. 17)
Ulcerative colitis is a continuous mucosal inflammatory state that affects the rectum and the colon.
Ulcerative colitis shows circumferential and diffuse mural thickening,
though this is non-specific,
needing correlation with a clinical context of abdominal pain,
bleeding and diarrhea.
When the disease is controlled there are typically no significant finding on CT.
- Crohn’s disease (Fig. 18)
Crohn’s disease is a chronic inflammatory muti-systemic disease with transmural inflammation anywhere along the gastrointestinal tract.
When Crohn’s disease is suspected the remainder of the gastrointestinal tract should be carefully evaluated,
particularly the terminal ileum.
On imaging the rectum may be spared or be involved in a focal and eccentric fashion and at the ano-rectal level perianal abscesses and fistulae are the most common complications,
though rectal strictures and deep pelvic abscesses may also be seen.
- Deep peri-rectal abscess in patient with Crohn’s disease (Fig. 19)
Abscesses are identified on imaging as well-defined collections with rim enhancement.
These are frequently associated with fistulous tracts but may be found isolated as atypical presentations,
particularly in patients with Crohn’s disease.
- Endometriosis (Fig. 20)
Endometriosis is due to the presence of endometrioid glands and stroma outside of the uterus.
Endometriomas are frequent ovarian manifestations,
deep pelvic endometriosis affects the Douglas cul-de-sac and the anterior rectal wall may also be involved.
- Peri-rectal hydatic cyst (Fig. 21)
Hydatic cysts result from an echinococcal infection with formation of cysts anywhere in the body.
Hydatic cysts typical imaging findings are of a cyst with multiple daughter cysts inside.
- Fournier’s gangrene (Fig. 22)
Fournier’s gangrene is a necrotizing fasciitis of the perineum,
caused by an anorectal and less commonly a genitourinary infection or perineal trauma.
Imaging may be performed to assess the extent of disease.
On imaging with CT there is fascial thickening and soft tissue stranding along with soft tissue gas.
CT is the primary imaging modality in the trauma setting,
allowing the assessment of injury extent as well as of other associated injuries.
- Rectal perforation (Fig. 23)
- Active rectal bleeding (Fig. 24)
Bleeding is detected on CT images as spontaneously hyperdense content in close proximity to the area of hemorrhage or by extravasation of contrast media on enhanced images.
- Ischemic rectal changes (Fig. 25)
Ischemic proctitis is an unspecific finding on imaging,
usually with ulcer or erosion of the mucosa.
- Anal imperforation and recto-urethral fistula (Fig. 26)
Anorectal malformations are due to the abnormal development of the uro-rectal septum.
In the setting of imperforate anus,
the rectum and anus may fistulize (95% of cases) to the perineum,
vagina,
urethra or bladder or may end in a blind-ending pouch.
Imaging can aid in depicting the abnormal anatomy and the presence of fistulous tracts.
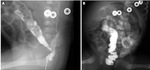
- Hirshprung disease (Fig. 27)
Hirshprung disease is characterized by the failure of ganglion cell precursor to migrate to the hindgut with aganglionosis of the distal colon and rectum,
causing functional partial colonic obstruction.
The most frequently involved segment is the recto-sigmoid.
Fluoroscopic studies with contrast enema are used for the diagnosis and assessment of the length of the involved segment.
On imaging the affected segment is of small caliber with a proximal dilatation and saw-tooth irregularity is frequently seen in the aganglionic segment.
- Tail-gut cyst (Fig. 28 and Fig. 29)
Tail-gut cyst (or hamartomas) are retrorectal multilocular cystic lesions that originate from remnants of the embryonic hindgut and are lined by intestinal mucosa.
These lesions are relevant due to their potential of malignant degeneration,
but their imaging findings are nonspecific.
- Duplication cyst of the rectum (Fig. 30)
Duplication cysts at the level of the rectum correspond to <10% of gastrointestinal duplication cysts.
These are cystic lesions along the rectal wall,
that contain intestinal mucosa and may or may not communicate with the rectal lumen.
The cyst content depends on the presence or absence of communication with the intestinal lumen.
Occasionally on the emergency setting rectal foreign bodies can be imaged,
namely to determine if these have any associated internal injury.