We retrospectively review pediatrics BVM in our department since 2010.
Imaging explorations were acquired according to institutional protocol and documented by CT,
MRI,
US or DSA.
Developmental Venous Anomaly (DVA) was the most common BVM.
Arterio-Venous Malformations (AVM) was the most frequent entity among the group with AVS.
BVM WITH AV SHUNT
1.- FOCAL LESIONS (late triggering event)
1.1.- Pial AV shunt
Pial arteriovenous shunts are abnormal connections between arteries that would normally supply the brain tissue (pial arteries) and veins that normally drain the brain, within the brain parenchyma and lack of a capillary network,
resulting in rapid arteriovenous shunting.
The connection between artery and vein can take place via a tangle of abnormal vessels called nidus (pial AVMs) Fig. 4 or can be direct/fistulous (pial AVF) Fig. 5.
1.2.- Dural AV shunt: Dural AV fistulas(DAVFs)
DAVFs are abnormal connections between arteries that normally not supply the brain (these arteries feed the meninges,
the bone,
and the muscle),
and small venules situated within the walls of the dural sinuses.
DAVFs account for 10%-15% of all intracranial AV shunts in children.
Nevertheless,
they present characteristic features in this age group.
Lasjaunias described three main dural AV shunts:
a) Dural sinus malformation (DSM) Fig. 6
In DSM the AV shunts are secondary and usually accessory to the sinus malformation. Most authors postulate that DSM is a disease of sinovenous development,
with sinus wall overgrowth that continues to develop after birth.
There is an abnormal development of epidural confluence of venous spaces leading to segmental giant lakes,
followed by secondary thrombosis of the spaces and subsequent remodeling if the venous drainage of the brain can be rerouted.
DSMs represent 2 % of all the AV shunts in the pediatric population,
but they have very poor prognosis and only 10% of patients will have normal brain development.
The most common clinical symptom is macrocrania,
followed by intracranial hemorrhage,
seizures,
and mental retardation.
Acute cardiac failure due to volume overload is seen in 20 % of the patients.
Rapid spontaneous sinus thrombosis may lead to consumption coagulopathy and venous infarction.
b) Infantile form of DAVFS (IDAVFS)
They are characterized by high-flow multifocal DAVFs without sinus malformation (there arenВґt venous lakes which differentiates them from DSM).
Also,
in IDAVs spontaneous venous thrombosis almost never occurs.
The high-flow shunt produces a venous sinus sump effect,
which may lead to a pial AVM and may regress after occlusion of the primary shunt.
c) Adult form of DAVFS (ADAVFS)
Almost all are located at the cavernous venous plexus,
but they may rarely involve the sigmoid sinus.
The affected sinuses are normally small and sometimes partially thrombosed.
No multifocal lesions have been described in this entity,
which is the rarest type of dural shunts in pediatric population.
1.3.- Vein of Galen Aneurysmal Malformation (VGAM) Fig. 7
VGAM is a diencephalic AVM draining into a dilated vein of Galen (represented by the embryonic precursor of the vein of Galen,
called as median prosencephalic vein).
The arterial disposition (persistent limbic arch) and persistent venous embryonic routes (dorsal diencephalic vein and the falcine sinus) support the embryonic nature of this AV shunt.
The nidus of the lesion is located on the midline,
and often receives bilateral and symmetrical supply. According to angioarchitecture,
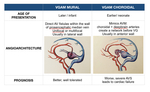
two forms of VGAM are defined Fig. 8 :
-VGAM Choroidal type: mimics an AVM,
so it has a contribution of several choroidal arteries (and usually deepbrain arteries) with small nidus-like draining into the anterior aspect of the prosencephalic median vein.
This condition is encountered in most neonates with poor clinical outcome.
-VGAM Mural type: has a direct AV fistula,
with a hole in the persistent median vein accepting arterial inflow (uni or multifocal).
The mural type is frequently encountered in infants,
who usually have a better prognosis.
There are several physiopathologic consequences of the VGM related to high flow left to right shunt (cardiac insufficiency),
vascular steal (progressive brain atrophy) and venous hypertension (leads to progressive hydrocephalus). Indeed,
no cardiac failure,
no brain atrophy,
normal resistivity index (sylvian artery) and a simple angioarchitecture are good prognosis factors.
2.- SEGMENTAL LESIONS (intermediate triggering event)
a) Cerebral Proliferative Angiopathy (CPA) Fig. 9 Fig. 10
Cerebral proliferative angiopathy (CPA),
previously known as “diffuse nidus-type AVM” or “holohemispheric AVM”.
CPA represents 2–4 % of all brain AVMs,
with median age of presentation of 20 years. CPA is separate from the "classic” brain AVMs,
because are different in its clinical presentation,
natural history,
angioarchitecture and treatment.
The characteristics features of CPA are the normal size of multiple feeder arteries,
the presence of proliferative-type nidus with normal brain tissue interspersed throughout the vessels.
The absence of early venous drainage on dynamic images is the clue in differential diagnosis from classic brain AVMs.
CPA usually involves large areas of brain parenchyma (often an entire lobe or even a hemisphere is affected).
Most common clinical manifestations include progressive neurologic deficits,
transient ischemic attacks,
seizures,
and headaches,
with hemorrhage being extremely rare.
b) Hemorrhagic Angiopathy
This entity must be considered different from CPA.
These malformations are characterized by small,
scattered “niduslike” lesions in subcortical/white matter regions.
Clinically it presents with intracerebral hemorrhage,
with a high tendency to recur in the first 6 months
3.- METAMERIC LESIONS (early triggering event)
a) Cerebrofacial arteriovenous metameric syndrome / CAMS
Also known as Wyburn-Mason syndrome or Bonnet-Dechaume-Blanc disease,
CAMS is one of the segmental neurovascular syndromes which result from a somatic mutation before the migration of the endothelial precursor cells, defined by multiple AVMs with characteristic segmental distribution.
Three types are described depending on location CAMS I (medial prosencephalic group),
CAMS II (lateral prosencephalic group), CAMS III (rhombencephalic group).
Both components, intracranial and maxillofacial,
are required for diagnosis.
b) Cerebrofacial venous metameric syndrome / CVMS
CVMS is a group of diseases classified on the basis of the embryologic concept that an anomaly in one body segment simultaneously causes failure of nerves,
skin,
and blood vessels within that segment.
CVMS is defined by multiple VMs with metameric distribution,
which has the same classification that CAMS (CVMS 1,
CVMS 2 and CVMS 3).
-Sturge-Weber syndrome / encephalotrigeminal angiomatosis Fig. 11
ItВґs part of a wide spectrum of possible phenotypes included in metameric lesions.
This condition is a congenital syndrome (not inherited) based on a failure of the cortical veins developing,
leading to numerous long-term intracranial manifestations as a result of chronic ischemia and expanded alternate routes of venous drainage.
The diagnosis is usually obvious due to a congenital facial capillary malformation ("port wine stain" or "facial naevus flammeus").
This feature is almost always present and involves the ophthalmic division of the trigeminal nerve (V1).
Leptomeningeal angiomatosis is the brain involvement of this syndrome (almost always unilateral at the same side of the facial stain).
The main features on neuroimaging studies are cerebral lobar atrophy (Dyke-Davidoff-Masson like) with cortical/subcortical calcification ("tram-track" sign),
leptomeningeal enhancement and enlarged ipsilateral choroid plexus.
The most common clinical manifestation is seizures that usually begin in the first few years of life.
Other symptoms are hemiparesis,
stroke-like episodes,
neurological deficit,
headaches and intellectual disability.
-Blue rubber bleb nevus syndrome or Bean syndrome
ItВґs a rare condition characterized by multifocal venous malformations (VMs) in any tissue,
which is most prominent in skin,
soft tissues,
and gastrointestinal tract (which could lead to lower gastrointestinal bleeding).
In head and neck region are typical the involvement of submandibular,
parotid and masticator spaces,
thymus and cranium (sinus pericranii).
BVM WITHOUT AV SHUNT
a) Developmental venous anomalies (DVAs) Fig. 13
DVAs,
formerly called cerebral venous angiomas,
are congenital malformation of veins which drain normal brain.
DVAs are composed by one or more dilated vein(s) and their smaller tributaries.
The converging arrangement of veins draining into a single larger central collecting vein results in the typical “caput medusae” pattern.
DVAs are the most common BVM (approximately 55%).
A single lesion is the typical presentation,
though multiple DVAs have been described in some syndromic disorders as the blue rubber bleb nevus syndrome.
DVAs usually represent an incidental finding and are clinically silent.
Thus,
the obstruction of venous outflow may be related to a number of clinical manifestations,
like headaches,
seizures and transient neurologic deficits.
Hemorrhage is very rare (<5%) and this finding should raise the suspicion of an associated cavernous venous malformation.
b) Cavernous Venous Malformation (CVMs) Fig. 14
CVMs are venous malformations composed of a "mulberry-like" cluster of hyalinized dilated thin-walled capillaries,
with surrounding hemosiderin and no nervous tissue interposed between the vascular spaces.
CVMs may occur as sporadic or familial cases.
While most sporadic CVMs are isolated lesions,
familial CVMs are multiple in nearly 80% of cases.
The possible association with DVAs is well-known.
The typical “salt and pepper” or “popcorn-like” pattern on imaging studies is caused by old hemorrhages,
cholesterol crystals,
hemosiderin pigmentation,
calcification,
and hyaline thickening of the vessel walls.
Most CVMs remain asymptomatic throughout life and are found incidentally.
Presentation due to hemorrhage may cause headache,
seizure or focal neurological deficit.
The risk of hemorrhage is 1% per year.
c) Capillary telangiectasia
Capillary telangiectasia is a vascular malformation that consists of localized collections of abnormal thin-walled vascular channels interposed between normal brain parenchyma (distinguishing them from CVMs).
Most capillary telangiectases are incidental findings.
Capillary telangiectasia is nearly always a single lesion.
ItВґs often located in the midline and significantly more frequent in the posterior fossa (60%-70%).
Contrast-enhanced MRI is the only imaging modality that displays capillary telangiectases (CT and DSA are negative for telangiectasia) and it appears as a contrast-enhancing lesion with early contrast washout.
d) Sinus pericranii Fig. 15
This entity is a rare venous anomaly characterized by communication between intracranial dural sinuses and extracranial venous structures (epicranial veins),
usually via an emissary transosseous vein.
Sinus pericranii can be isolated or associated with other malformations (secondary),
including craniosynostosis or intracranial venous abnormalities such as dural sinus hypoplasia.
Symptoms are infrequent but include headache,
vertigo,
feelings of fullness,
or local pain.