Although the utility of imaging is limited in NF,
currently it is accepted its role with the following objectives:
- Confirm the diagnosis in clinically doubtful cases.
- Identify complications.
- Anatomic information useful for the surgery.
- Depicting the extent of tissue involvement.
Importantly,
in patients who are severely compromised or with high clinical suspicion,
surgical treatment should not be delayed for the performance of imaging.
In our hospital center over the last two years studied,
we have observed that all the cases diagnosed of NF underwent imaging tests (mainly computed tomography) which evidence the usefulness of these in view of the difficult management of this disease.
Although MRI is the modality of choice for detailed evaluation of soft-tissue infection,
it is not usually the first cross-sectional test available in the emergency department for FN,
because its acquisition is time-consuming and will delay treatment,
taking into account the bad prognosis and aggressive course of this disease.
Therefore,
we dispose of several imaging tests in the management of this pathology:
Radiography
It shows low sensitivity,
since radiographs can be normal until the infection and necroses are established.
However,
despite its limitations,
radiographs can be more sensitive than a physical examination for the detection of soft-tissue gas.
Therefore,
it is considered useful as the first imaging modality if clinical examination suggests the presence of soft-tissue gas.
Moreover,
it can exclude other causes of soft-tissue swelling,
such as bone fractures.
-Initially,
its findings are similar to cellulitis:
- Soft-tissue swelling and thickening.
- Soft-tissue opacity and effacement of fat planes.
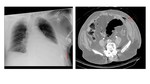
-The best diagnostic clue is gas tracking in the soft tissues and fascia without previous trauma,
although its absence does not exclude NF.
Fig. 4
Computed Tomography
CT provides analysis of compartmental anatomy and shows good accuracy in evaluating the extent of tissue or osseous involvement.
Moreover,
it helps to identify underlying infectious sources and detect other complications.
The rapidity of CT compared with MRI makes its great advantage in the assessment of an emergent necrotizing fasciitis evaluation.
There are some renowned signs which suggest necrotizing infection of soft tissues [3,4]:
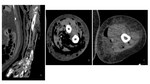
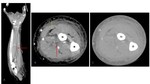
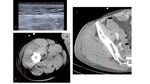
- Subcutaneous and subfascial emphysema:
CT is the most specific imaging test for the diagnosis of NF if soft-tissue gas is present,
as gas along subfascial planes without prior trauma is the hallmark of NF.
However,
it is not frequent: it may be absent in up to 50% of cases,
especially in early stages,
diabetes or nonclostridial microorganisms.
Hence,
its absence does not exclude the diagnosis of NF.
( Fig. 5 Fig. 6 )
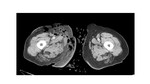
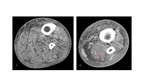
-Asymmetric fascial thickening and deep fascial (intermuscular septa) fluid collections:
These findings,
which traduce fascial fluid and inflammatory changes,
are the most frequent finding in necrotizing soft-tissue infections.
However,
they lack specificity since they can be present in nonnecrotizing fasciitis.
( Fig. 7 Fig. 8 )
In order to increase specificity there are criteria that support NF against other nonnecrotizing fasciitis,
which do not require emergency surgery:
- Extensive deep fascia (intermuscular septa) involvement.
- Thickness of > 4 mm.
- Three or more muscle compartments involved.
- Focal or diffuse nonenhancing portion of the deep fascia.
This finding is very demonstrative of necrosis,
and hence of FN.
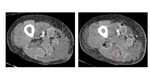
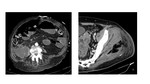
-Muscle involvement:
Muscles demonstrate edema as a sign of involvement in NF,
as muscle enlargement associated with decreased attenuation.
( Fig. 9 )
Muscle tissue in CT tends to be spared compared to fascia in NF because of its generous blood supply,
thus the presence of intramuscular fluid or gas collection loculated inside a muscle supports a suppurative stage of pyomyositis.
( Fig. 10 )
-Skin thickening,
septation of the subcutaneous fat and thickening of the superficial fascia,
findings that we can also find in cellulitis.
Entities which result in fluid retention (as congestive heart failure or renal disease) may produce subcutaneous infiltration and will have a similar appearance,
nevertheless,
it tends to be symmetric and diffuse. Moreover,
subcutaneous edema in necrotizing fasciitis tends to be less extensive than in patients with cellulitis.
Ultrasonography
Ultrasound (US) is generally nonspecific in the assessment of infection,
since it cannot differentiate properly between infectious and inflammatory collections.
Moreover,
given that the lack of resolution for deeper structures,
US has a high risk of misdiagnosis in this context.
Consequently,
its role is limited in the work-up of necrotizing fasciitis.
In current guidelines it is accepted that US may be useful to differentiate simple cellulitis from NF in unstable patients where other imaging modalities cannot be performed.
Apart from this,
it may help excluding noninflammatory causes of soft-tissue swelling,
such as deep venous thrombosis and soft-tissue tumors.
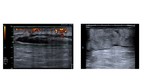
-Early NF can resemble soft tissue changes of cellulitis.
These are:
- Diffuse hyperechoic skin and subcutaneous tissue thickening.
( Fig. 11 )
- Subcutaneous edema: “Cobblestone pattern”: hypoechoic regions within hyperechoic soft-tissue.
( Fig. 12 )
- Hypervascularity at color Doppler evaluation,
although it may be absent. ( Fig. 13 )
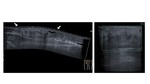
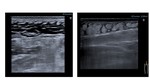
-The most representative US findings in NF are those derived from the involvement of deep tissues:
- Deep fascia irregularity and thickening (>4 mm).
- Accumulation of fluid within the fascia or in deep tissues.
- Emphysema: an echogenic layer of gas above the deep fascia with posterior dirty acoustic shadowing.
( Fig. 14 )
-Furthermore,
US shows other advantages in the evaluation of a soft-tissue infection,
being useful for the assessment of:
- Articular involvement
- Fluid collections
- Foreign bodies
- Ultrasound guided drainages