Type:
Educational Exhibit
Keywords:
Diagnostic procedure, MR, CT, Spleen, Abdomen, Trauma
Authors:
M. Dimarco1, V. Putortì1, F. Arnone2, R. Cannella1, D. Giambelluca1, M. Midiri1; 1Palermo/IT, 2Partinico/IT
DOI:
10.26044/ecr2019/C-3201
Findings and procedure details
Imaging can be useful for the detection and differential diagnosis of splenosis.
Patient history should take into account abdominal surgery or prior splenic trauma.
Sometimes,
splenosis nodules can be discovered as incidental findings during an US or CT exam performed for other reasons.
The diagnostic procedure may be integrated by using contrast-enhanced CT and MRI to reach a correct diagnosis.
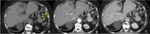
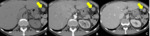
On CT,
splenosis nodules may be rounded or sessile,
with similar density and contrast enhancement of the spleen [2,3].
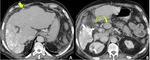
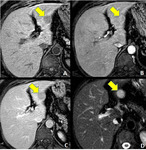
Like their appearance on CT,
even on MRI,
intensity and enhancement of splenosis nodules are the same as those of normal splenic tissue,
as they show hypointense and hyperintense signal on T1-weighted and T2-weighted sequences,
respectively,
and heterogeneous contrast enhancement [3].
Moreover,
after administration of hepatobiliary contrast agent,
they will be hypointense on hepatobiliary phase and hyperintense in the high-diffusion sequences,
however,
without diffusion restriction on the ACD map,
thus presenting the typical behavior of the origin splenic tissue.
When the splenosis nodules are adjacent to other solid abdominal organs,
the diagnosis is particularly challenging and they may mimic primary neoplastic lesions.
Superparamagnetic iron oxide (SPIO) contrast agents have been successfully used in the diagnosis of splenosis as they are specific to the reticuloendothelial system of the liver and spleen [4].
The diagnosis of splenosis may be confirmed non-invasively with scintigraphy or PET/CT with Tc99m-tagged heat-damaged RBC scan (Tc-99m-DRBC) with autologous erythrocytes,
which shows high uptake of damaged erythrocytes in the ectopic splenic tissue.