We designed a retrospective study which reviewed imaging findings in hematology-oncology patients with splenic involvement hospitalized in our clinic in the period covering 2011-2018.
The CT and MRI findings were further sub-classified based on the patient’s disease and the accompanying splenic complications.
Classification:
Concerning the hematologic malignancies,
many entities affect the spleen by:
- tumoral infiltrating
- immunosuppressive or hemostasis disorders
- hematopoiesis changes
Among these,
splenic implication is either specific or not,
depending on the causative pathology and its complications 1,4,5
Splenomegaly in onco-hematology is a current pattern and it can be either homogenous,
either heterogeneous.
Causes: Variate causes, may present with different physiopathology, reason why its aspects are unspecific in the absence of other information.
Physiopathology. The main physiopathologic mechanisms are: 4,6
1.Hypersplenism;
2.Splenic infiltration;
3.Vascular congestion;
The most frequent focal splenic nodular lesions are due to onco-hematological etiologies.
Those are polymorphous nonspecific lesions that require differential diagnosis (see table 2).
Every diagnosis requires specific management of the patient.
I.
TUMORAL IMPLICATION
1.
Lymphomas
Lymphomas are a group of hematologic malignancies that starts in the lymphocytes.
There are two main types of lymphomas:
Both types involve the lymph nodes,
the lymphatic organs (the spleen is the most important) or and others organs with lymphoid tissue. 1,3,4
Lymphomas affect the spleen in one-third of the cases.
The involvement can be:
- primary
- secondary (most common).
Primary splenic lymphoma is encountered (1-2% of lymphomas) 1,4,5,9
There are 4 patterns of splenic involvement:
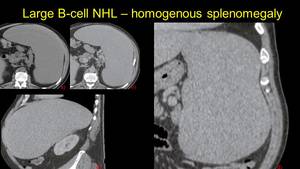
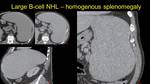
Fig. 1: Homogenous Splenomegaly in a pacient with B cell non-Hodkin lymphoma. Image a) NECT and b) CECT axial view, images c) and d) sagital and coronal view.
Table 2 - Splenic lymphoma:CT and MRI aspects
|
Lymphoma
features
|
Size,
number,
shape
|
Splenic lesion aspect |
| Computed tomography |
MRI |
| NECT |
CECT |
T1w |
T2W |
Other |
| Homogenous splenomegaly |
- |
- |
- |
- |
- |
- |
|
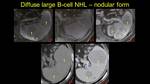
Multiple nodular
lesions
|
1-10cm
> 2
irregular
round
|
low/
medium
attenuation
|
low
enhancement,
usually homogenous
|
low intensity |
high intensity |
diffusion restriction,
possible necrosis or bleeding foci |
| Diffuse miliary infiltration |
< 5mm
miliary
round
|
isodense |
low
enhancement,
usually homogenous
|
low intensity |
high intensity |
unreliable |
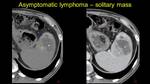
| Large solitary mass |
> 3cm
1
irregular
|
low/ medium
attenuation
|
low
enhancement,
usually heterogeneous,
possible invasive
|
low intensity |
high intensity |
diffusion restriction,
possible necrosis or bleeding foci,
possible
invasive
|
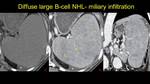
- Diffuse infiltration with miliary lesions < than 5 mm; Fig. 2
Fig. 2
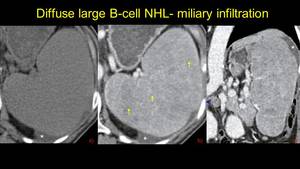
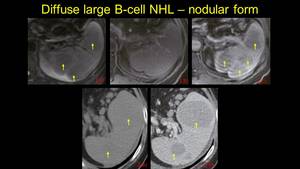
Fig. 2: Another pacient with B cell Lymphoma, with homogenous splenomegaly on NECT (image a), but with multiple visible miliary nodules after contrast enhancement - axial and coronal view (b and c) - arrows. Note the presence of the peritoneal fluid - asterix
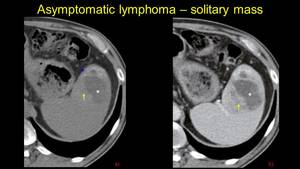
Fig. 4: Pacient known with cirrhosis. Echography finds an incidental heterogenous single splenic lesion. CT exam is performed – a) nonenhanced hypoattenuating lesion, b) contrast enhanced CT reveals an enhanceing heterogenous solitary lesion – lymphoma is confirmed by medulary bipopsy.
Lymphomas can also affect other organs simultaneously or not with the spleen. Fig. 6 Fig. 7
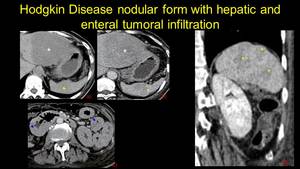
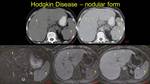
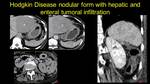
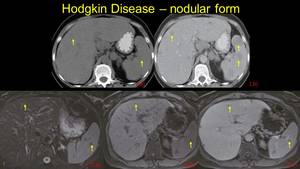
Fig. 6: Hodkin lymphoma – a) hepatic - asterix and b) splenic - arrow hypodense contrast enhanceing lesions; c) duodenal and enteral tumoral implication - arrowhead and d) note that in the coronal view the spleen has normal size.
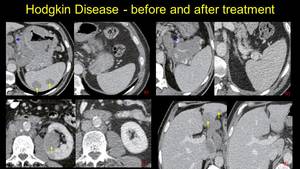
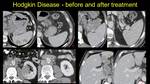
Fig. 7: Aggressive Hodkin disease, at diagnose presents splenic involvement, adenopathic blocks on the small gastric curvature and splenic hillum (arrowheads) – a and b; left kidney tumor (arrow) and retroperitoneal adenopathic block – image c), and finally liver lesions – image d). On the right of these images we note the complete regression at 1 year after the treatment.
2.
Leukemias
In leukemias,
the spleen can be involved (homogeneous splenomegaly Fig. 8 or miliary infiltrates),
in association with lymph nodes enlargement. 1,3,5,6,9
As an exception,
leukemia can cause the appearance of focalized lesions in the spleen,
but rarely,
this form is found often in lymphomas;6 Fig.
9
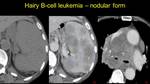
Hairy cell Leukemia is a rare form of leukemia,
which causes often the appearance of nodular focalized splenic lesions.9 Fig. 10
CT and MRI aspects in leukemias (table 3)
|
Leukemia
form
|
Size,
number,
shape
|
Splenic lesion aspect |
| Computed tomography |
MRI |
| NECT |
CECT |
T1W |
T2W |
Other |
|
Homogenous
enlarged
spleen
|
- |
- |
- |
- |
- |
- |
|
Multiple
nodular
lesions
|
>3 mm
> 2
round
regular
|
low
medium
attenuation
|
low
enhancement
|
low intensity |
high intensity |
possible
diffusion
restriction
|
|
Diffuse
infiltration
|
< 5 mm
miliary
|
isodense |
low
enhancement
|
low intensity |
high intensity |
unreliable |
|
Hairy B cell
leukemia
|
any
any
round
infiltrative
|
low
medium
attenuation
|
low
enhancement
|
low intensity |
high intensity |
possible
diffusion
restriction
possible necrosis
|
Table 3
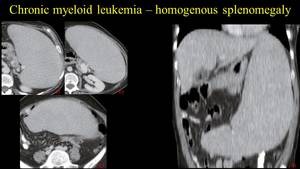
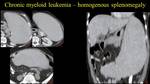
Fig. 8: Chronic myeloid leukemia – homogenous splenomegaly – axial view at the celiac trunk, kidney and pelvic level – a, b c; coronal view - d
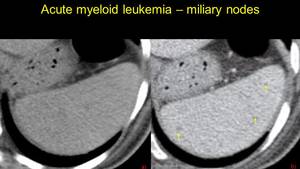
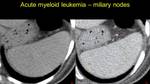
Fig. 9: Pacient with acute myeloid leukemia – multiple isodense hypovascular splenic microlesions.
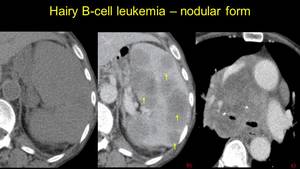
Fig. 10: Nodular splenic lesions in a Hary B cell Leukemia – a) isodense on NECT, b) hypovascular on CECT, which associates a mediastinal tumoral mass.
3. Myeloproliferative disorders:
There are three types:
-
Polycythemia Vera - characterized by an increased number of red blood cells in the bloodstream that can cause blood clotting disorders.
Imaging findings reveal splenomegaly and sometimes splenic infarction.1,5,9,12
-
Essential Thrombocytosis - characterized by megakaryocytes proliferation in the bone marrow leading to hemostasis disorders. 9,12 Fig. 13
-
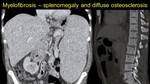
Myelofibrosis - the bone marrow is replaced by fibrous tissue, leading to extramedullary hematopoiesis,
progressive splenomegaly and thrombocytopenia.12 Fig. 11
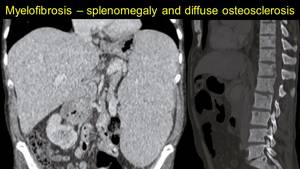
Fig. 11: In myelofibrosis, the bone marrow is replaced by fibrotic tissue, causing the appearance of extramedullary haematopoiesis, progressive liver and spleen enlargement (image a) and diffuse osteosclerosis (image b).
4. Myeloma
Is a type of cancer that involves malignant plasma cells.
There are multiple types of myeloma,
the most frequently encountered is the multiple myeloma (>90% of the cases).
It can be localized in tissues like bone,
skin,
muscle and lung.1,4,6
- Splenomegaly is seldom associated in multiple myeloma,
but when present,
it is severe.
- Focalized nodules in extramedullary myeloma (a rare form) is exceptionally rare.1
5. Myelodysplastic syndromes
Refer to a heterogeneous group of hematopoietic stem cells disorders,
consisting of anemia,
neutropenia,
thrombocytopenia or pancytopenia.1,4,6
Imaging findings can reveal:
- localized osteomyelosclerosis.
- splenomegaly is encountered in just a quarter of cases.
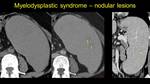
- nodular splenic lesions are very rare; as it is stated in medical literature,
they are especially marks of dyspoiesis rather than marks of proliferation.1,4,6 Fig. 12
Fig. 12
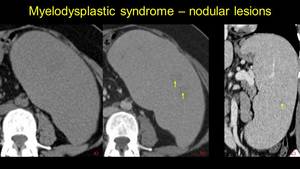
Fig. 12: Pacient diagnosed with myelodysplastic syndrome performes a CT examination for upper left abdominal pain, wich reveals severe splenomegaly, unhomogenous by the presence of isodense lesions on NECT, vizbile after contrast enhancement, slightly hypoenhancing (images b and c) that suggest extramedullary haematopoiesis.
II.
SPLENIC EMERGENCIES IN ONCO-HEMATOLOGY PACIENTS
1.
Bleeding disorders
Thrombocytopenia associated with onco-hematological pathology,
but also the anticoagulant and antiplatelet therapy are the main causes of hemorrhagic complications;7,8
Hemorrhagic complications involving the spleen:
The main cause is trauma,
spontaneous non-traumatic etiology is rare,
and usually associated with blood coagulation disorders.7,8
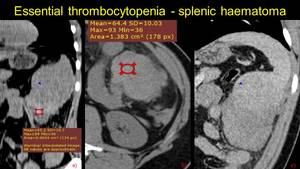
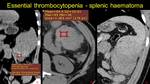
Fig. 13: We mentioned before the essential thrombocytopenia. We present the case of a young male known by our clinic with the disease, which presents at the emergency room for upper left abdominal acute pain sindrome. An emergency CT exam is performed, revealing a macronodular lesion at the inferior splenic pole and a hyperattenuating fluid accumulation (marked by the ROI) – images a and b. No signs of acute bleeding after contrast administration (image c). Splenectomy is performed and the hystopathological exam confirms the hematoma with capsular rupture.
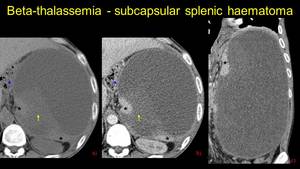
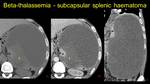
Fig. 14: Pacient known with beta-thalassemia – a) axial NECT – fluid accumulation (arrowhead) with b) spontaneous hyperattenuating areas, which in coronal view c) extends on a length of 30 centimeters associating parenchimal compresion (asterix) – degraded subcapsular haematoma, no extracapsular effraction
In oncohematological patients,
those complications can occur due to thrombocytopenia,
anticoagulant and antiplatelet therapy,
splenic infarction Fig. 15,
chemotherapy and moderate and severe splenomegaly.
5,7,8,12
Although in some cases the hematoma can be autolimitated and degrade (cystic aspect),
in splenic hemorrhage/rupture the diagnosis and treatment are urgent,
reason why CECT is the imaging method of choice.
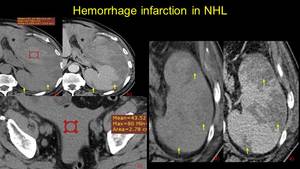
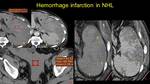
Fig. 15: Non-Hodkin lymphoma. Splenic spontaneos hyperdense accumulation (ROI) with extracapsular effraction (asterix), NECT - a and CECT – b, asscoiating haemoperioneum at pelvic level – c. Note the triangular hipodense lesions – d, unenhancing – e, suggestive for splenic infarction
2. Ischemic disorders
Nowadays there is are a few little data about thrombotic complications in patients with hematological malignancies.
Recent studies prove a higher risk of thrombosis in patients with lymphoma,
multiple myeloma or acute leukemias,
especially in recently diagnosed patients or in patients undergoing chemotherapy.12
The incidence of thrombotic events is influenced by the type and the stage of the disease,
antitumoral therapy and by the widely used central venous catheters.12
Ischemic complications are due to perfusion defects followed by splenic infarction Fig. 16 Necrosis is the result of arterial or venous occlusion.
Splenic infarction is a rare cause of abdominal pain,
even if the prevalence is unknown,
the most incriminated etiologies being hematological causes.12
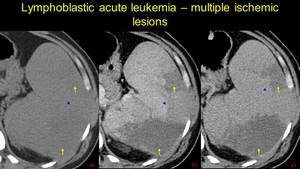
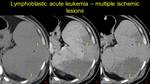
Fig. 16: Acute lymphoblastic leukemia known patient. Triangular spontaneos hypoattenuating areas (a), unenhancing, sugesstive for splenic infarction (arrows), and another hypodense area, slighthly enhancing in venos phase – arrowhead (b) which is homogenized in the parenchymal phase – suggestive for a perfussion disorder.
CT is the examination of choice in splenic infarct evaluation.
Imaging findings: a non-enhancing triangular lesion with the apex targeted to hilum and the base positioned to the capsule; chronic lesions can transform into a fibrous lesion with capsular retraction Fig. 17 or can liquefy Fig. 18.
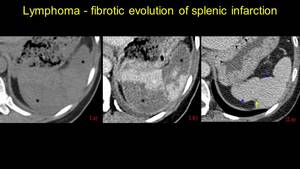
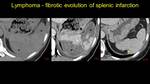
Fig. 17: Pacient known with lymphoma, presents at the emergency room for upper left pain. I – splenic infarction, NECT (a), and CECT (b) – asterix. II after 2 years, reevaluation CT shows chronic lesions – arrowhead, with decreased dimensions and capsular retraction with thin fibrotic area – arrow.
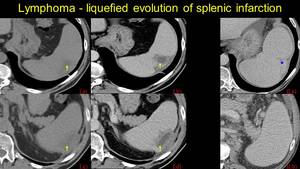
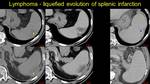
Fig. 18: Pacient known with Non-Hodkin Lymphoma – liquefied splenic infarction at the upper pole (NECT – I.a and CECT – I.b) and middle of the spleen (NECT – I.c and CECT – I.d). Four years later, disease relapse is suspected – chronic aspect of the infarction with fibrotic bands and capsular retraction. Note the enlarged spleen and peritoneal fluid.
3. Splenic abscess in immunosupressed patients
Infections are frequent in hematological patients and in those who underwent allogeneic bone marrow transplant; 9,10,11
Neutropenia,
altered B-cell and splenic functions predispose to a high risk of severe infections 9,10,11 Fig. 19; Fig. 20
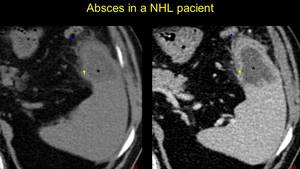
Fig. 19: NHL pacient presents at the emergency room with fever, chills and pain – echography reveals a decreased echo-reflectivity lesion with thick increased echo-reflectivity walls. A CT is performed – hypoattenuating unenhanceing lesion (asterix), with enhanceing thick walls, and fat stranding (arrowhead) – splenic abscess with Candida Albicans.
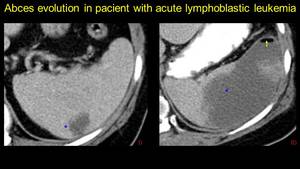
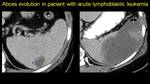
Fig. 20: Pacient known with acute lymphoblastic leukemia: image I – splenic abscess (arrowhead) – antibiotic treatment for five days is performed, but because of bad evolution, another CT exam for reevaluation is decided – image II – fulminant progression of the absces, with gas-fluid level (arrow). Interventional drainage is practiced – Meticillin resistant Staphylococcus Aures)
Often immunocompromised patients develop multi-organic abscesses,
either of bacterial or fungal etiology.10,11 Fig. 21
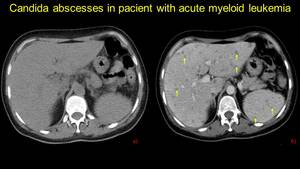
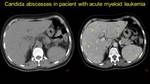
Fig. 21: Acute myeloid Leukemia in treatment with cytostatics, presents at the emergency room for long history of fever and chills – diagnosed with sepsis – NECT (a) and CECT (b) – izodense hypoenhancing lesions suggestive for abscesses and microabscesses – blood tests confirm Candida Albicans
The definitive diagnosis often requires a histopathological examination of a biopsy specimen of the involved organ involved.
Unfortunately obtaining a biopsy sample is rarely possible.10,11 Fig. 22
Both CT and MRI are helpful in the diagnosis of splenic abscesses.
CT: abscesses are normally low-density lesions (20-40 HU),
that associate peripheral contrast uptake.
MRI: T1w images show a low signal,
which may increase if there is proteinaceous content; high T2w signal,
and peripheral slight contrast uptake similar to CT.
Ascites and pleural effusion may be associated.
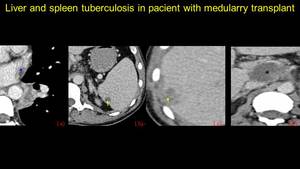
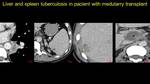
Fig. 22: Pacient who underwent medullary allotransplant, presents at the emergency room with fever and weight loss – CT examination for diagnosis: I.a - Necrosing lesion at the left pulmonary hillum (arrowhead), I.b – hypovascular splenic and I.c - liver lesions and I.d – a necrosing adenopathy. A liver biopsy is performed for the lesion in segment VI and the result is liver tuberculosis. The patient is treated in a dedicated hospital and after one year, a reevaluation CT is performed: note the liquefied aspect of the hepatic and splenic lesions and the regression of the hepatic hillum adenopathy.
III.
DIFFERENTIAL DIAGNOSIS
The patient`s medical history,
the imaging and clinical findings can determine help guide the clinician through the differential diagnoses.
1
There is no standardized diagnosis protocol for the management of focal splenic lesions,
and the definitive diagnosis requires histopathological examination.1,3,5
The diagnostic splenectomy is rarely used,
because of a mortality and morbidity rate of 3%,
respectively 37%.
Fine needle aspiration biopsy has a lower risk,
but significant,
it's used being limited.1
Therefore,
among the acquired trauma,
infections,
infarctions and onco-hematological malignant lesions,
the differential diagnosis includes:
- primary (angiosarcoma)
- secondary malignant causes (up to 50% of metastases due to melanoma and other due to lung,
breast and colon cancer) Fig. 23,
- benign lesions such as cysts,
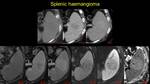
haemangioma Fig. 26,
- hamartomas and lymphangiomas,
- infiltrative disease such as sarcoidosis Fig. 24,
amyloidosis,
haemosiderosis,
Gaucher's disease Fig. 25 or extramedullary hematopoiesis Fig. 27 .1,2,3,4,5
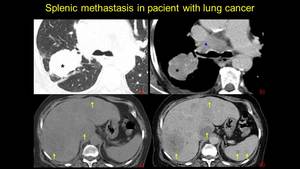
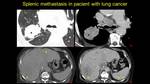
Fig. 23: Female pacient known with pulmonary tumor, post-chemotherapy evaluation: - I a) lung window, b) mediastinum window – enhancing macronodular tumor with mediastinal adenopathy. Images c and d – NECT and CECT – metastases in the liver and spleen.
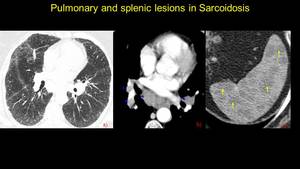
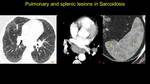
Fig. 24: Pacient known with pulmonary and splenic sarcoidosis. A) lung window – difuse interstitial pulmonary infiltrates, b) CECT mediastinum window – multiple enlarged limph nodes at the pulmonary hillum (arrowhead), c) multiple hypovascular splenic nodules.
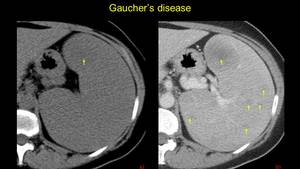
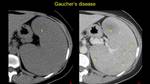
Fig. 25: Female pacient known with Gaucher’s disease – heterogenous spleno-megaly with multiple hypodense, hypoenhancing nodules (arrow)
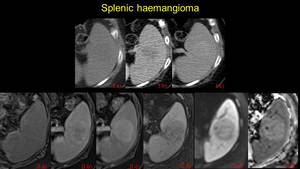
Fig. 26: Pacient with hyperecogene lesion identified by ultrasound. I CT examination: the lesion is a) hypoattenuating spontaneous, with centripete enhancing in venous phase (b), silghtly hyperenhancing in late phase. II MRI examination: a) isointense on T1w images, with similar enhancing pattern (b, c), low signal T2fs (d) and high signal on DWI and ADC (e and f) – splenic haemangioma.
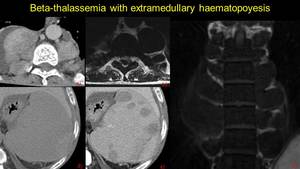
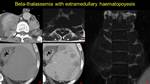
Fig. 27: Pacient know with beta-thalassemia – nodes of paravertebral extramedullary haematopoiesis a) CECT axial, b) MRI T2w axial and c) MRI T1w coronal view and splenic extramedullary hematopoiesis – NECT d) and CECT e) in axial view
IV.
STRUCTURED REPORT
1.
Dimension,
shape,
and contours of the spleen
2.
A detailed description of splenic/perispenic lesion (s)
- localization
- number
- shape
- contour/outline
- structure (attenuation/signal) - delineation between hemorrhagic,
cystic,
air,
or tissular lesions
- contrast enhancement/effraction (in active bleeding)
3.
Other changes involving the abdominal viscera
4.
Permeability of the abdominal vessels
5. Lymph node enlargement
6. Ascitis or pleural effusion
7.
Bones lesions
8.
Anatomical variants