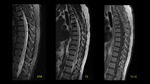
We report some cases presented to the emergency department with acute myelopathy.
CASE 1
We report a 81-year-old man,
with a history of prostatic adenocarcinoma,
who presented with sensory and motor disturbances of both lower extremities.
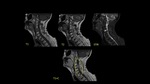
On MRI,
compression fracture of D4 with soft tissue mass was observed.
Sagital T1-weighted image showed vertebral body compression and soft tissue component with cord medullaris abnormal signal intensity related to spinal-cord compression.
CASE 2
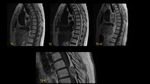
We report a 74-year-old man with history of non-small cell lung carcinoma with multiple osseous metastases who presented with acute onset paraplegia.
MRI showed intramedullary metastasis at C4 level with edema.
CASE 3
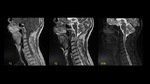
We report a 72-year-old woman with history of vulvar melanoma who presented acute sensory and motor disturbances of both lower extremities.
MRI revealed an extradural mass,
with heterogeneous contrast enhancement due to melanoma metastase.
A significant proportion of painful myelopathy is caused by tumoral compressive myelopathy.
It is important to obtain images after administration of gadolinium to evaluate the enhancement. Tumors compressing the spinal cord may be divided into extradural and intradural.
Extradural tumors may be classified as follows:
- Benign: sinovial cyst,
osteoma,
osteoblastoma,
giant cell tumor,
hemangioma,
eosinophilic granuloma,
schwannoma and meningioma.
- Malignant: metastasis,
multiple myeloma,
lymphoma and chondrosarcoma.
Intradural tumors are classified as follows:
- Extraespinal: neurofibroma,
meningioma,
lipoma,
schwannoma and arachnoid cyst.
- Intraspinal: astrocytoma,
ependymoma,
hemangioblastoma and metastasis.
CASE 4
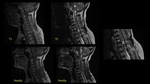
We report a 54-year-old man presented to the emergency room with quadriparesia after jerking neck movement.
MRI revealed a huge C5-C6 herniated posterocentral disc with spinal cord compression.
Post-traumatic myelopathy is four times more frequent in males,
in particular between 15 and 30 years of age.
The most mobile segments are more often affected,
in particular C5-C7 (as seen in our case) and T10-L2.
Clinically,
quadriplegia predominates in 30-40% of cases and paraplegia occurs in 6-10%.
Motor vehicle accidents are the most common cause,
accounting for 50% of the events.
Imaging findings may differentiate those patients who will benefit from emergency surgical decompression.
CASE 5
We report a 64-year-old woman presented to the emergency room with nuchal pain,
weakness in upper right limb and hypoesthesia in the left region of the D2-D3.
MRI revealed spontaneous epidural hematoma from C3 to D2 in patient treated by anticoagulant drugs with compression of the spinal cord and myelopathy signs.
CASE 6
We report a 54-year-old patient with subacute paraplegia.
MRI revealed serpent-like and dilated intervertebral veins with high signal intensity in the central part of the spinal cord related to edema.
Diagnosis was spinal dural arteriovenous fistula.
The spinal cord may be affected by compressive and non-compressive vascular diseases, of which the most common are malformations of the spinal dural arteriovenous fistula (SDAVF) type.
SDAVF is the most common spinal vascular malformation,
however it is still rare are often underdiagnosed.
In the early stages,
the clinical symptoms can be nonspecific and initially is misdiagnosed.
The exact etiology is unclear,
however,
the majority of patients become symptomatic in middle age suggesting that it is an acquired disease.
Male prediction is also well known.
On MRI the cord edema is most clearly shown as hyperintensities with peripheral sparing on T2-weighted images.
Vascular diseases should be suspected in any patient who undergo anticoagulation therapy.