Facet joints are symmetrical synovial-lined joints with a fibrous capsule.
They connect the articular facets of the vertebrae and are innervated by the medial branches of the dorsal rami of the spinal nerves.
Patients with FS may complain of low back pain that radiates to the thigh or iliac crest.
Exacerbation of pain commonly occurs during hyperextension,
torsion and lateral bending movements,
being it worse when getting up from bed or standing up after long sitting periods.
Initial management of these patients should be always conservative.
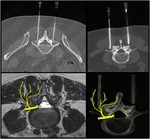
Imaging findings in FJ syndrome include:
- Joint space narrowing and osteophytes.
- Subchondral sclerosis and erosions.
- Hypertrophy of articular processes.
- Intra-articular vacuum phenomenon or fluid.
- Synovial cyst formation.
- Hypertrophy of the ligamentum flavum.
In FS,
injection of the FJ is indicated for diagnostic purposes and to reduce pain and improve mobility.
In most cases,
a mixture of a long-acting corticosteroid with a local anesthetic is used.
Imaging guidance to locate the inferior portion of the joint improves technical and clinical efficacy.
Meanwhile,
medial branch infiltrations are done next to the medial branch of the dorsal ramus of the spinal nerve,
where the superior articular process joins the base of the transverse process.
Patients with significant pain relief after infiltrations will benefit from FJ denervation using techniques in which nerve fibers are destroyed by heat (RF ablation) or cold (cryoablation).
Since each FJ in the lumbar spine is innervated by nerve fibers from two levels RF electrodes or cryoprobes have to be placed in two subsequent levels.
Another technique for FJ denervation is endoscopic rhizotomy,
which uses a small cannula and endoscope to directly visualize and ablate the medial branch nerve.
The procedures mentioned before can be performed under fluoroscopic or CT guidance.
CT has the benefit of extremely accurate positioning of needles and probes without exposing the operator to ionizing radiation.
The method used will depend on the operator’s preferences and local availability.
Other alternatives include MR-guided high-intensity focused ultrasound (HIFU) and percutaneous fixation techniques.
Techniques
Placement of the patient independently from the imaging technique used should be in prone decubitus with a pillow or some blankets under the patient’s abdomen in order to reduce lumbar lordosis,
thus improving comfort.
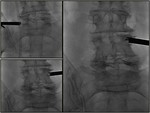
Fluoroscopic approaches
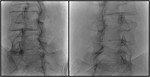
Oblique approach: with the patient in prone decubitus the x-ray tube is centered with a slight caudal angulation (10-15⁰) eliminating the double contour of the inferior margin of the vertebral bodies.
From this position,
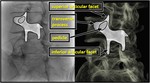
the x-ray tube is tilted 25-30⁰ laterally to the side been treated to obtain an oblique view of the spine where the typical “Scotty dog” image can be seen.
PA approach: with the patient in prone decubitus the x-ray tube is angled caudally (10-15⁰).
The transverse process and pedicle are identified.
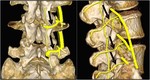
CT approach
The positioning of the patient is similar to that of fluoroscopy.
A radiopaque marker is placed over the patient’s skin that will guide us to establish the point of entry of the needle in the X-axis and to locate the Z-axis using the CT scanner laser marker.
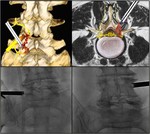
FJ infiltrations
A spinal needle (commonly 22G) is advanced towards the intra-articular or periarticular space for each joint treated.
In cases of severe joint space narrowing or osteophytes that interfere with the procedure,
the needle should be directed towards the lower portion of the joint were the synovial recess is usually accessible.
Contrast can be injected to confirm intra-articular positioning but with an adequate technique,
this can be unnecessary.
Once the needle is placed correctly,
a solution of an anesthetic and a long-acting corticosteroid is injected (1-2 mL).
Injection of larger volumes inside the articular capsule should be avoided because it can lead to its rupture and overdistention can also cause pain.
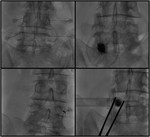
Medial Branch Block
Medial branches lie nearby the junction of the transverse and superior articular processes.
In the oblique view,
this point corresponds to the eye of the “Scotty dog”.
A small amount of anesthetic is used for diagnostic blocks,
usually,
0.5 mL and correct needle placement can be confirmed by injecting a small amount of contrast.
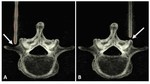
Under CT guidance the tip of the needle should be placed in the angle formed by the transverse process and the neck of the medial aspect of the superior articular process.
Ultrasound guide for branch blocks has also been used with the same accuracy as fluoroscopy.
Neurolysis
After successful medial branch diagnostic blocks,
neurolysis is the next step.
The approaches for these techniques are similar,
but CT guidance is preferred due to precise needle placement and complications that may occur.
Neurolysis can be done using different methods including injection of ethyl alcohol,
radiofrequency or cryotherapy,
being RF the most used technique.
Radiofrequency ablation (RFA)
The term radiofrequency (RF) refers to the least energetic portion of the electromagnetic spectrum.
It is a type of wave or electromagnetic radiation with high frequency (400-500 Hz) that is in the category of non-ionizing radiation.
There are several systems and ways of applying radiofrequency for therapeutic purposes.
RF can be applied by brief pulses of high voltage,
reaching temperatures around 40-42⁰C.
Heat dissipation between pulses avoids tissue coagulation,
therefore the effect is not very destructive,
producing mainly a neuromodulatory effect.
The continuous RF,
also called thermal or conventional is administered continuously,
without periods of heat dissipation and temperatures reaching up to 80-82⁰C.
Its biological effect consists in the destruction of the tissue on which it is applied.
(from 50-55⁰C cellular damage is irreversible).
This procedure can be done under fluoroscopic or CT guidance as described with medial branch block.
A 22G cannula (RFA) is inserted reaching the target point.
To achieve optimal results,
the needle is placed tangentially to the target point parallel to the nerve to be treated.
Sensitive and motor stimulation must be done before the ablation.
During sensitive stimulation (frequency 50-100Hz) a tingling sensation will be noticed in the painful area,
meanwhile,
during the motor stimulation (frequency 2-5 Hz) leg muscle contraction should not be provoked.
If there is leg motor contraction this indicates that the tip of the electrode has motor nerves nearby and repositioning is mandatory.
Once the electrodes are adequately positioned local anesthesia is applied (we use 10mL Mepivacaine with 80mg of Triamcinolone Acetonide) bilaterally in the levels being treated.
Next,
the rhizolysis is initiated with an automatic program with a maximum temperature of 80⁰C for 90 seconds.
One to three cycles may be performed and once the procedure has ended the patient is put under observation during one hour.
Later the patient can return to his normal life with the recommendation of not doing harsh exercises for around 2-3 weeks.
Complications and inconveniences of radiofrequency
- Radiation iatrogenic ablation of the motor branch or even spinal cord (rare with CT).
- Worsening of baseline pain after RF.
- Post-denervation neuralgia.
- Decreased skin sensitivity.
- Transitory leg pain or permanent weakness.
One of the main disadvantages of radiofrequency is the reappearance of pain due to nerve regeneration.
Cryoablation
Cryoneurolysis consists in the application of cold to the nerve to cause its denaturation.
This technique relies on the physical principles of the Joule–Thompson effect,
and consist of rapid decompression of gas (N2O or CO2) at the extremity of the probe,
delivering very low temperatures (-70⁰).
An ice ball is formed at the tip of the probe causing a conduction block and vascular damage of the vasa vasorum that translates in long-term pain relief.
Accurate probe placement as in RFA is very important but a tangential approach of the probe is not mandatory.
The degree of cold and length of application will determine also the extent and duration of the effect.
Local anesthesia usually is not necessary during the procedure.
Endoscopic Rhizotomy
Endoscopic facet joint denervation rhizotomy is a minimally invasive procedure.
Imaging is used to identify the exact point of entry and a small needle is inserted.
A guide wire is inserted through the needle,
the needle is removed and a small incision is made.
The skin is gently dilated to insert a small cannula and the dilators are removed.
This creates a portal to access the nerve and a specially designed endoscope is used to identify the small branches to be treated.
A RF probe is inserted through the endoscope for the ablation,
disrupting the pain signal transfer.
The scope is moved to adjacent spinal levels and the RF probe is once again used.
This procedure has the benefit that nerve fibers causing pain are identified and selectively treated.
Also,
tissues are spared and muscles and ligaments are prevented from damage,
thus preserving the stability of the spine.
The joint capsule can also be treated during the same procedure depending on the indications.
Under endoscopic view,
the joint can either be punctured,
infiltrated or tissue can be removed using forceps,
shaver blades and RF probes.
Some of the indications for Endoscopic Rhizotomy are:
- Chronic lumbar back pain.
- Facet hypertrophy.
- Facet joint arthritis and osteoarthritis.
- Failed back surgery syndrome.
- Post-discectomy syndrome.