Acute mesenteric ischemia evolves through different stages of severity,
from an early mucosal involvement to a more extensive transmural damage which clearly significantly impacts the patient’s prognosis.
Based on a classification of the American Gastroenterological Association [4],
arterial and venous ischemia are usually defined,
with different characteristics at CT scan.
Arterial ischemia is by far the most common etiology.
In most of the cases it is secondary to superior mesenteric artery (SMA) emboli or SMA thrombosis,
usually localized in the proximal third of the vessel [5].
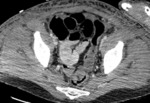
A particular form of ischemia,
occurring in almost 30% of the cases,
is due to low-flow states (the so-called non-occlusive mesenteric ischemia),
such as in hypovolemic shock in trauma patients [fig.
1].
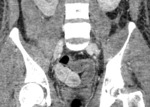
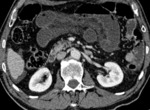
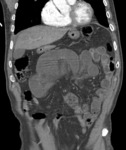
Characteristic CT finding of arterial occlusive ischemia is the well-described “paper-thin-walled” bowel,
with low contrast enhancement,
that appears quite early during the pathologic process and represents the consequence of a significant reduction in vascular volume [fig.
2].
If the etiology is not removed,
the damage evolves towards the disruption of the bowel walls,
inducing intramural air to fill the portal vessels [5].
Venous mesenteric ischemia represents less than 20% of all mesenteric ischemic events.
It is due to venous thrombosis,
which may be primary or secondary to inflammatory conditions,
recent surgery,
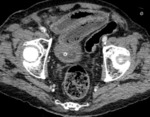
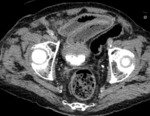
and hypercoagulable states in general [6]. Its characteristic feature on CT scan is a marked thickening of the bowel walls,
due to mural oedema or haemorrhage [fig.
3; fig.
4]; in the latter case,
as aforementioned,
an unenhanced scan could be of value to highlight the spontaneous hyperattenuation.
Vascular signs are also sometimes recognizable,
including venous filling defect,
vein enlargement and venous engorgement up to the appearance of collateral circulation,
particularly when the thrombotic event involves the proximal venous traits [6].
Mesenteric fat stranding and ascites may be common findings in acute mesenteric ischemia,
though they are not specific and their presence is not related to the severity of injury [fig.
5,
fig.
6].
The progression from initial ischemia to infarction is usually associated with dilatation of the ischemic loops due to fluid exudation and disappearance of peristalsis.